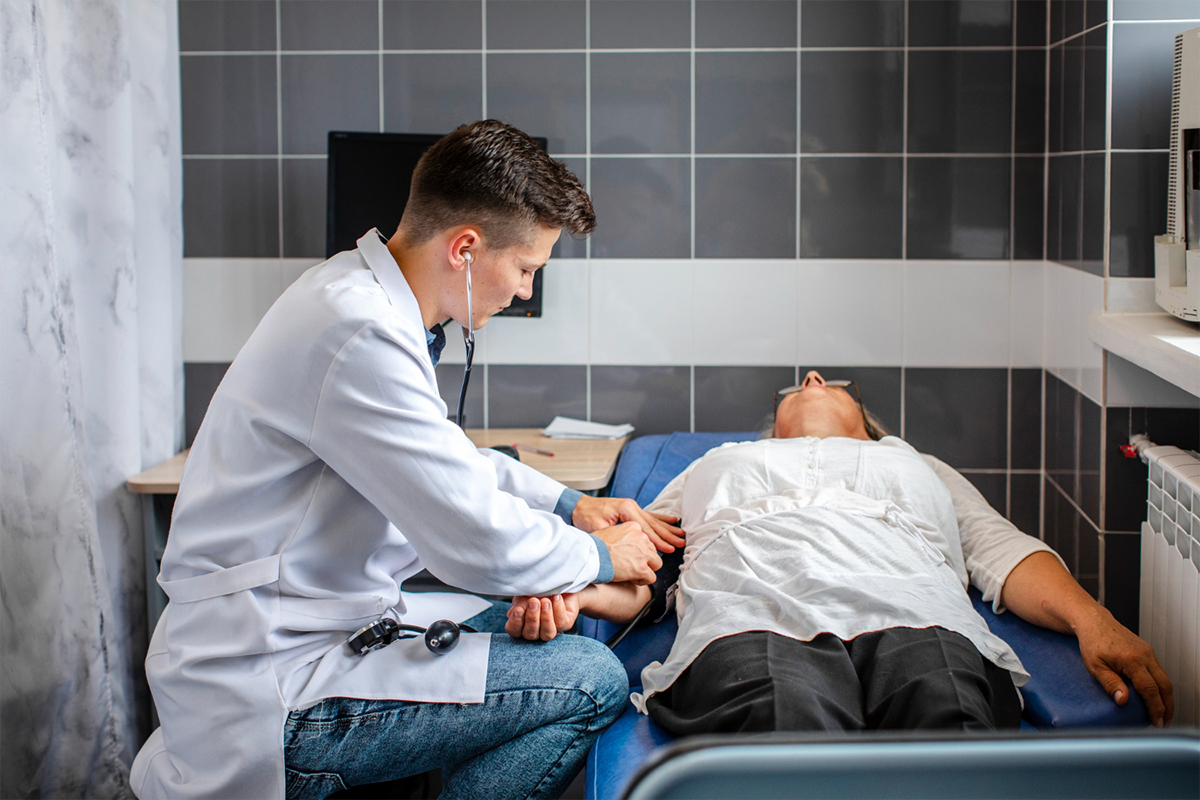
1. Getting the patient ready
To improve vein visibility, the patient lies down, usually on their back, with their legs slightly raised. To preserve sterility, an antiseptic solution is used to clean the treatment area.

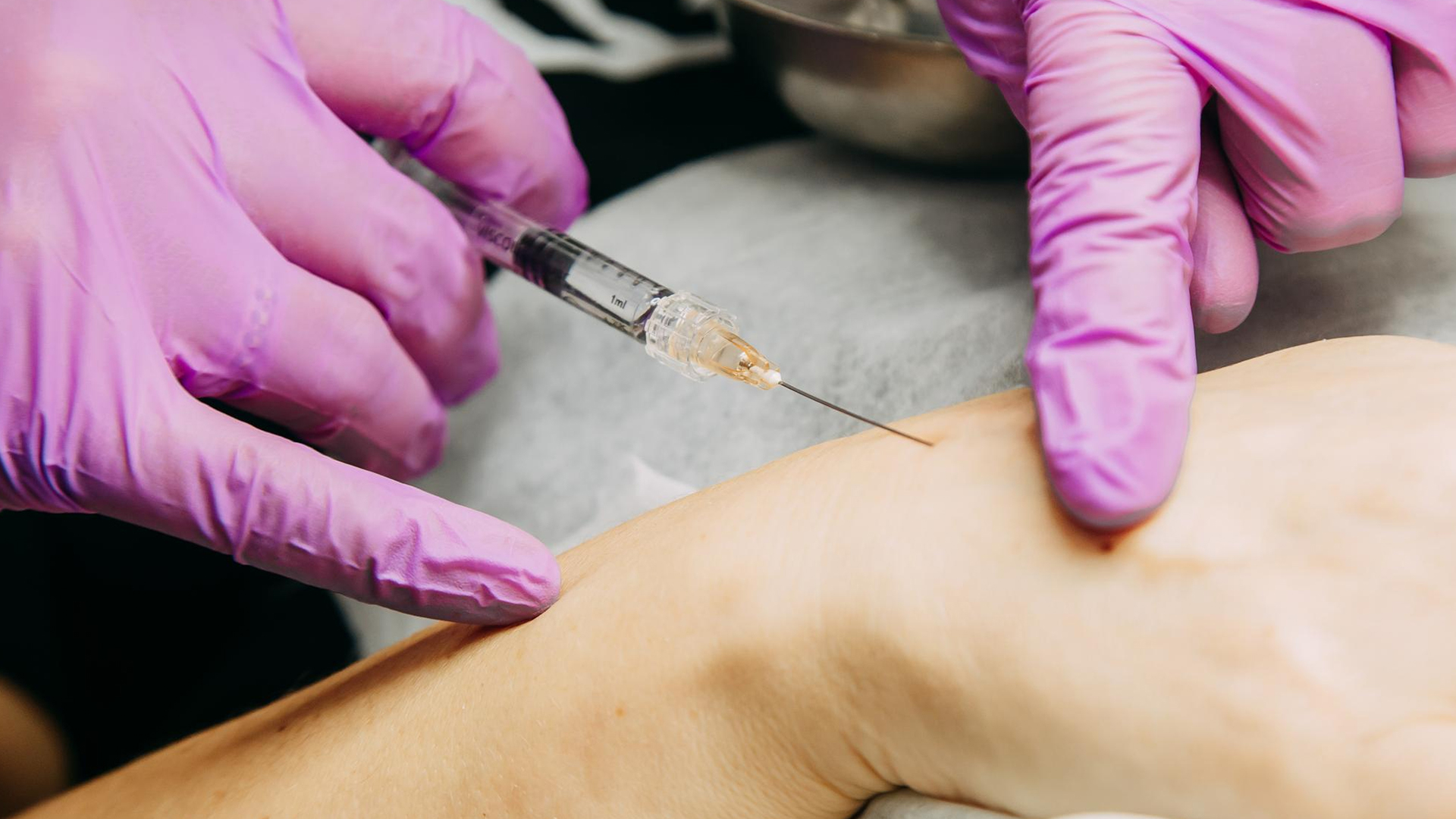
To improve vein visibility, the patient lies down, usually on their back, with their legs slightly raised. To preserve sterility, an antiseptic solution is used to clean the treatment area.
To ensure accurate targeting during foam injection, the target veins are located and mapped using a duplex ultrasound probe, especially for bigger varicose veins.
To create a microfoam, the sclerosing agent (often sodium tetradecyl sulfate or polidocanol) is combined with carbon dioxide or air using a double-syringe approach (Tessari method). For greater effectiveness, this foam extends the sclerosant's contact with the vein wall and increases its surface area.
A tiny needle is placed into the target vein while being guided by ultrasonography. By carefully filling the vein with foam, the vein walls collapse and seal shut, displacing blood.
To encourage vein closure, lessen swelling, and hasten healing, the treated leg is covered with an elasticated compression bandage or stocking after injection.
Typically, treatment sessions go between thirty and forty-five minutes. Depending on the quantity and size of veins treated, some patients could need more than one session.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Large trunk veins (such as the great saphenous vein), tiny reticular veins, and tributaries can all be treated with foam sclerotherapy. Patients with symptoms chronic venous illness can benefit from it.
Foam sclerotherapy, which successfully lowers vein diameter and reflux, is beneficial for people with superficial vein reflux that has been verified by ultrasound.
It is an excellent choice for patients whose vein anatomy prevents them from undergoing endovenous thermal ablation or surgery.
For varicose veins that return or persist after surgery or other therapies, foam sclerotherapy is frequently used.
Foam sclerotherapy helps repair venous ulcers and skin abnormalities in advanced stages (C4 to C6 CEAP classification).
Smaller veins are also treated with it to make them seem better.

Foam sclerotherapy is a minimally invasive outpatient surgery that typically doesn’t require anesthetic, resulting in little discomfort and no recovery period.

Compared to conventional liquid sclerotherapy, the foam formulation enables treatment of larger and more complicated varicose veins by displacing blood and guaranteeing improved contact with vein walls.

According to clinical research, 80–90% of patients get long-lasting venous closure, symptom relief, a decrease in discomfort and swelling, and an improvement in the vein’s overall look.

After a 30- to 45-minute treatment session, patients can immediately return to their regular activities without needing to stay in the hospital or take a significant period off from work.

Foam sclerotherapy is a dependable substitute for surgery, particularly for people who are not ideal candidates for surgery, because it has a favorable safety profile and low adverse effects.

Compared to liquid sclerotherapy, which is usually seen as cosmetic, it is frequently reimbursed by insurance when performed for medical causes.

Treatment effectiveness and customisation can be improved by adjusting the foam’s concentration and volume to the patient’s unique venous problems.


Foam sclerotherapy improves leg look and patient confidence by reducing visible varicose veins in addition to treating the underlying venous insufficiency.