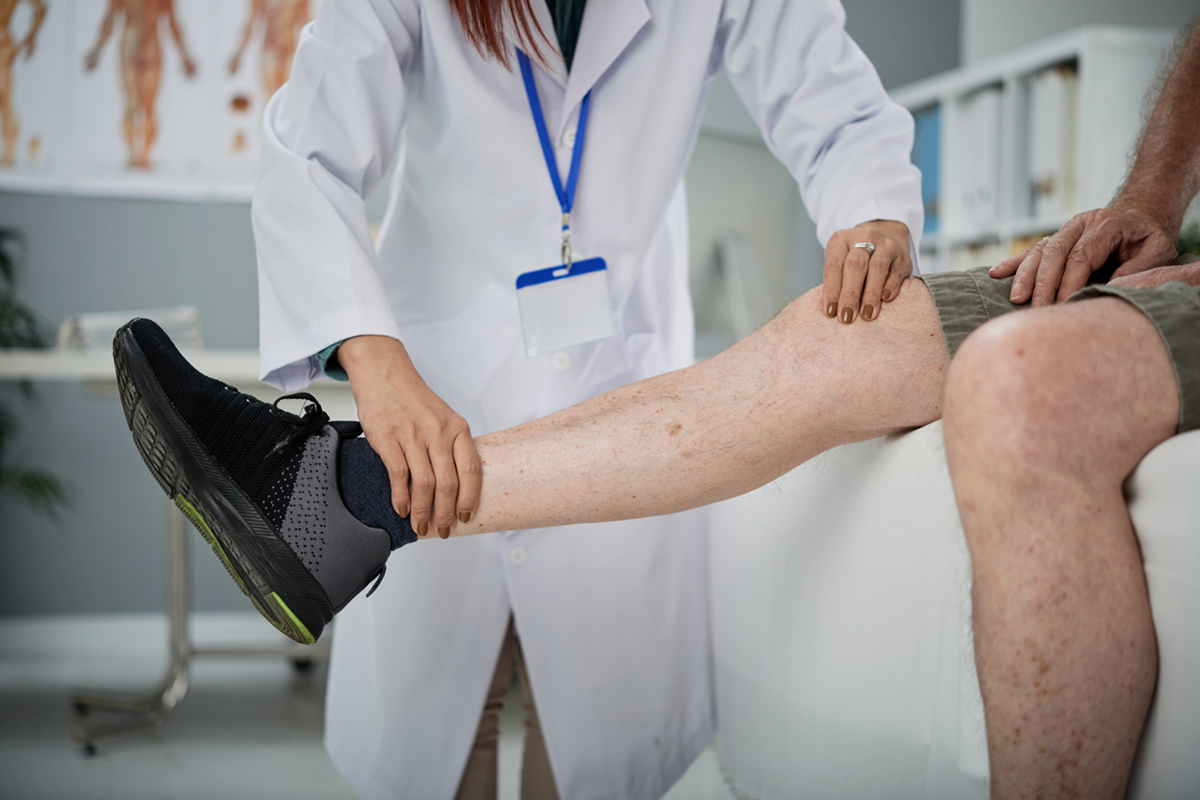
1. Insertion of the Catheter
To guarantee precise placement, a tiny catheter is placed into the afflicted vein under ultrasound guidance.


To guarantee precise placement, a tiny catheter is placed into the afflicted vein under ultrasound guidance.
Through the catheter, a specially made medical adhesive (glue) is administered to close the dysfunctional vein by sealing the vein walls together.
To help the glue seal the vein, the physician gently presses the treated area to keep the vein walls together. Along the vein's length, this is repeated.
After the vein has sealed, the catheter is taken out and the puncture site is covered with a little bandage.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Venaseal treatment is beneficial for people with symptoms such leg pain, edema, heaviness, cramping, or obvious varicose veins.
Patients who want a minimally invasive, non-thermal technique without the need for repeated needle injections or general anesthesia can benefit from venaseal.
For patients who cannot tolerate compression stockings because of their lifestyle or skin sensitivity, this treatment typically doesn’t require continuous use after the procedure.
Venaseal’s low pain and safety profile may be advantageous for people with medical issues that make surgery or thermal ablation dangerous.
Larger veins (2 cm or more) or veins deep within the leg that might be difficult to reach with other methods work well with venaseal.
Appropriate for treating more severe venous disease with skin alterations or venous ulcers in order to alleviate symptoms and stop the disease’s progression.
Venaseal’s quick recovery profile appeals to patients who want less rest and a speedy return to regular activities.
In certain situations, it is also used to treat upper gastrointestinal tract varices in order to stop bleeding.

Without the need for general anesthesia or sedation, foam sclerotherapy is a minimally invasive outpatient technique that causes no discomfort and permits an instant return to everyday activities.

Larger varicose veins that liquid sclerosant cannot cure as well can benefit from the foam’s ability to displace blood and expand inside the vein, increasing contact with the vein walls for more successful closure.

Studies reveal that foam sclerotherapy, which has success rates between 80 and 90 percent, has greater vein closure rates and fewer recurrences than liquid sclerotherapy.

With no downtime needed, sessions usually last 30 to 45 minutes, enabling patients to resume their regular activities and jobs right away.

Unlike liquid sclerotherapy, which is mostly seen as cosmetic, foam sclerotherapy is frequently reimbursed by health insurance for medical grounds.

Precise targeting is made easier by the foam’s echogenicity under ultrasonography. By modifying foam concentration and volume according to patient and vein parameters, treatment can be customized.

In addition to reducing the aesthetic look of varicose and spider veins, it helps lessen discomfort, swelling, heaviness, and other symptoms of venous insufficiency.