1. Mapping and Marking Ultrasounds
To properly arrange the treatment, a duplex ultrasound is used to identify and mark the target troublesome vein.

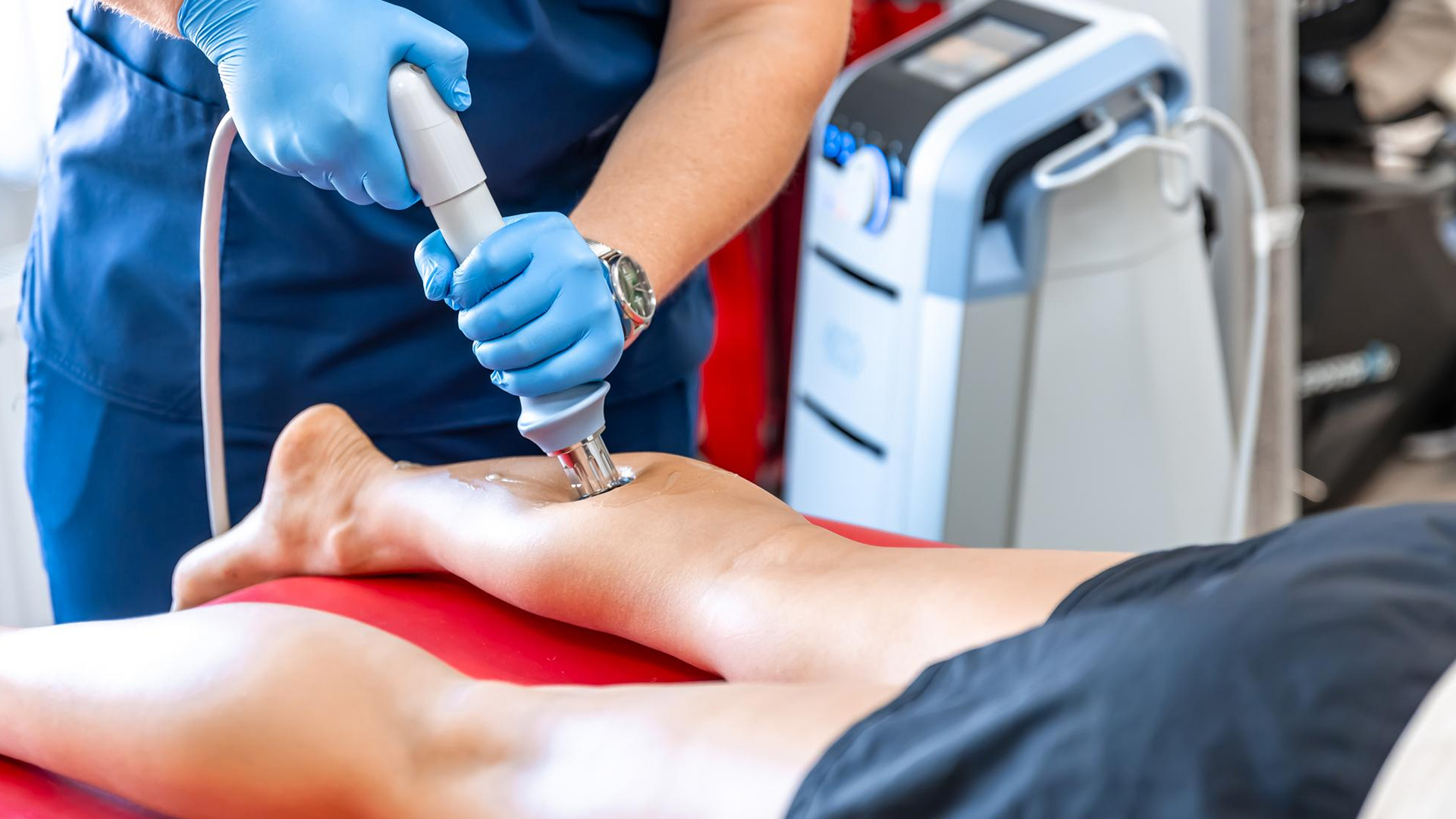
To properly arrange the treatment, a duplex ultrasound is used to identify and mark the target troublesome vein.
To numb the area and shield surrounding tissues from the heat, local anesthetic is administered down the vein's length and around the treatment site.
A narrow catheter with a radiofrequency probe is introduced into the damaged vein under ultrasound guidance after a tiny skin puncture is created, generally close to the knee.
Under ultrasound supervision, tumescent anesthetic is administered around the vein, compressing it and serving as a heat sink to protect surrounding tissues.
The radiofrequency fiber causes the vein to collapse and seal permanently by delivering regulated heat energy to the vein wall in segments, usually 7 cm at a time.
Radiofrequency energy is applied along the whole length of the targeted vein while the catheter is gradually removed.
The leg is covered with bandages or compression stockings to promote healing and lessen swelling. Following the surgery, patients are urged to walk.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





RFA is particularly beneficial for people with venous insufficiency symptoms include leg pain, swelling, heaviness, skin discoloration, ulceration, or inflammation.
Ideal for treating perforator veins with reflux verified by ultrasonography, the great saphenous vein (GSV), and the small saphenous vein (SSV).
Recommended for veins with a diameter more than 3 mm and reflux times longer than 0.5 seconds.
Those who continue to experience symptoms even after using compression stockings and other non-invasive treatments.
For patients seeking an efficient substitute for surgery with less discomfort, no need for general anesthesia, and a speedy recovery, RFA is perfect.For patients seeking an efficient substitute for surgery with less discomfort, no need for general anesthesia, and a speedy recovery, RFA is perfect.
Helpful in reducing symptoms and accelerating ulcer healing in cases with severe venous illness.
Additional surface varicosities can be addressed with supplementary techniques while both legs are being treated concurrently.
RFA has a low likelihood of complications and is safe for people with cardiovascular problems or those on anticoagulant therapy.

RFA is a minimally invasive process that is carried out under local anesthesia, lowering the risks of infections and severe bruising that come with standard surgery.

Because RFA uses tumescent anesthetic and moderate thermal radiation, it produces less post-procedural discomfort, bruising, and swelling than endovenous laser ablation and surgical vein stripping.

As an outpatient “walk-in, walk-out” operation, patients typically have little downtime and return to their regular activities in 24 to 48 hours.

RFA improves the quality of life for patients by effectively reducing symptoms such leg pain, edema, weariness, and heaviness. It also aids in the healing of venous ulcers.

By removing protruding varicose veins, the closure of defective veins improves the appearance of the legs.

Safe for people with comorbid conditions who would not be able to handle surgery or general anesthesia, as well as those on anticoagulant therapy.


















