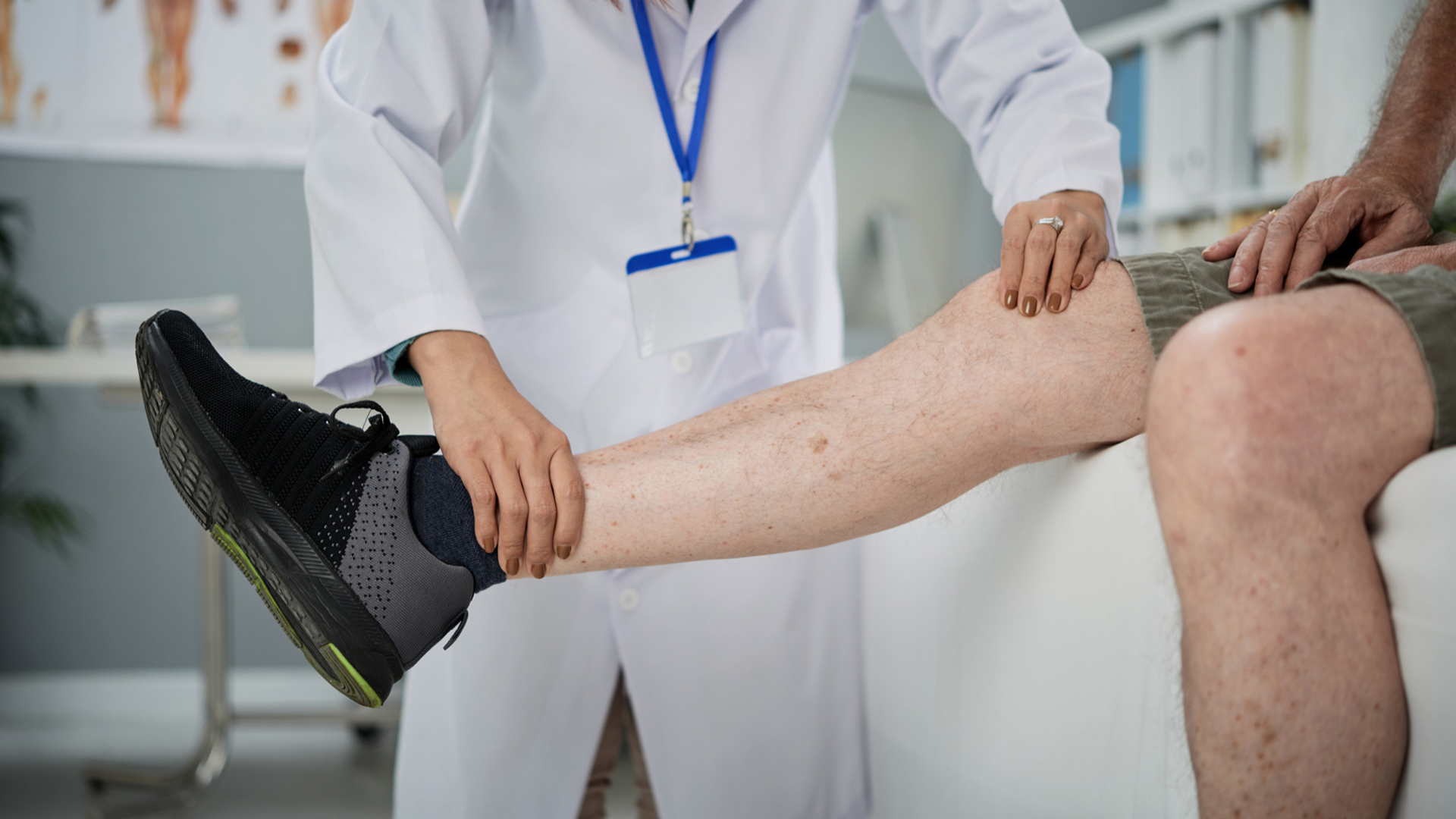
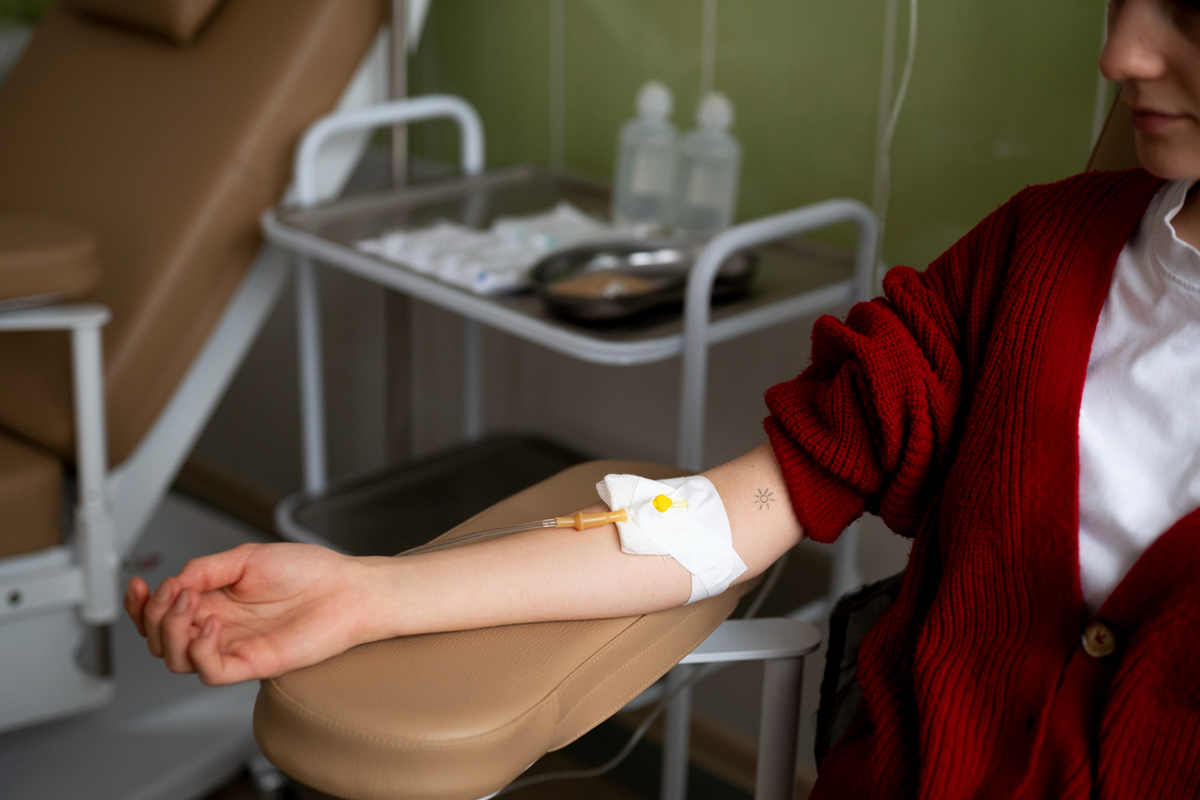
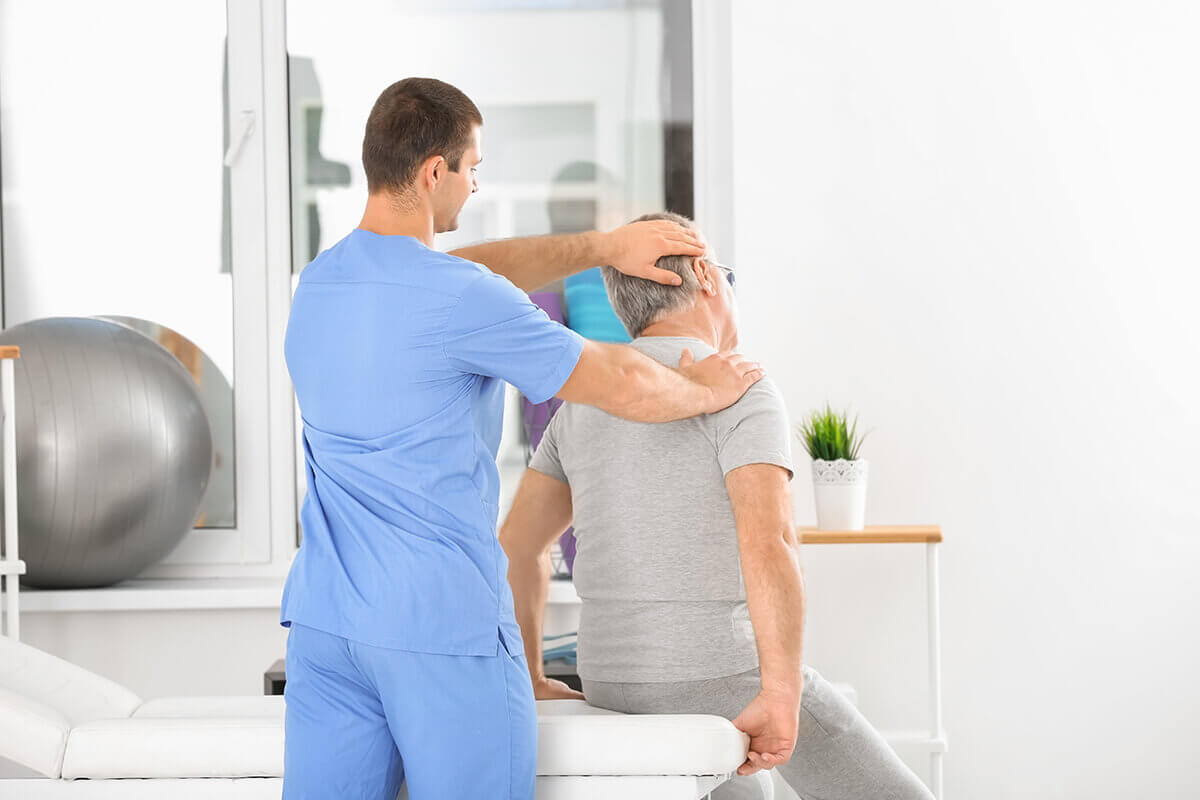
1. Preparing and Evaluating Patients
In order to validate the location and degree of thrombus, patients receive comprehensive clinical evaluation and imaging studies prior to the treatment. Medication may be changed, and informed consent is acquired.