1. Vascular Access and Patient Preparation
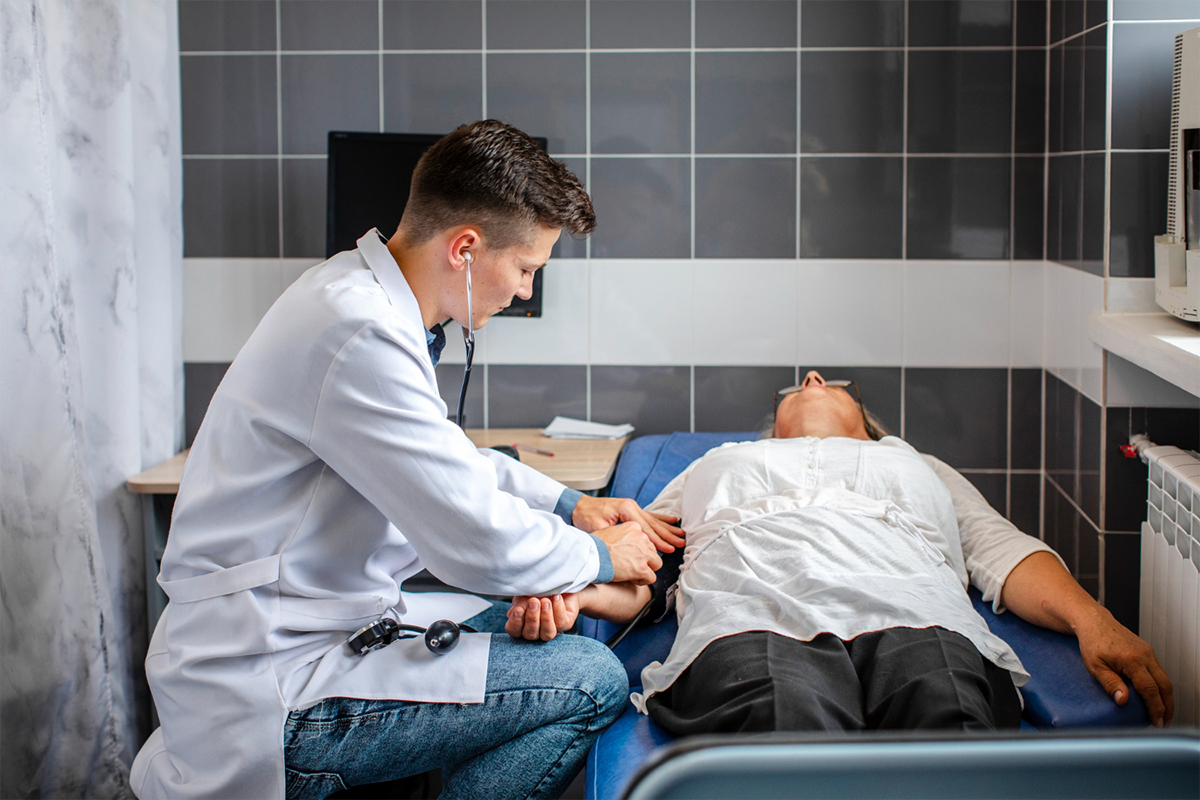
Vascular access is usually achieved through the femoral artery under sterile settings. Depending on the situation, either general anesthesia or sedation is given.

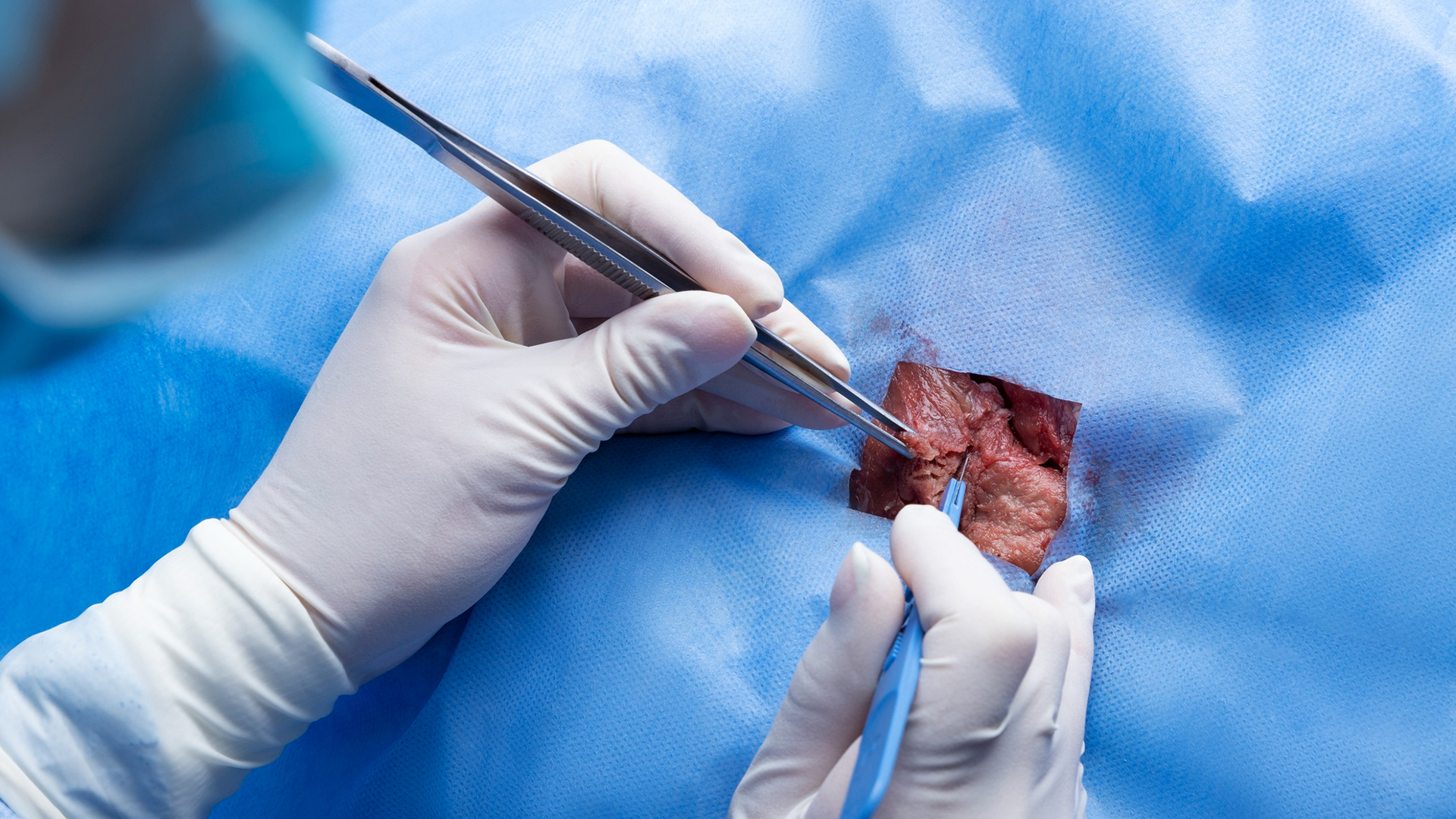
Vascular access is usually achieved through the femoral artery under sterile settings. Depending on the situation, either general anesthesia or sedation is given.
A microcatheter is carefully guided through the artery system to the location of the lesion that has to be embolized using fluoroscopic guidance.
To maximize the accuracy of embolic agent distribution, the microcatheter is placed as close to or inside the target vessel or nidus of the arteriovenous malformation (AVM).
Onyx (ethylene vinyl alcohol copolymer) or n-butyl cyanoacrylate (NBCA) glue is made. While glue quickly polymerizes when it comes into contact with blood, onyx is a non-adhesive liquid embolic agent dissolved in dimethyl sulfoxide (DMSO).
For Onyx: Under continuous fluoroscopy, the embolic agent is administered slowly to enable for a slow precipitation and solidification that forms a cast that blocks the vessel.
To prevent non-target embolization, the operator keeps a close eye on the degree of embolic agent penetration. Injection is stopped or the microcatheter is moved if reflux or excessive proximal filling happens.
Angiography verifies the successful blockage of the target vessels or nidus following embolization while maintaining flow in non-target arteries.
With caution, the microcatheter is removed. Closure devices or manual compression are used to produce access site hemostasis.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





used to lessen the risk of bleeding in hypervascular lesions or devascularize tumors prior to surgery.
management of arterial bleeding, such as peripheral or gastrointestinal hemorrhages.
Off-label use for angiomyolipomas, varicocele, aneurysm embolization, type II endoleaks following aortic repair, and other peripheral vascular abnormalities.
Onyx is used for embolizing high flow lesions and situations where catheter stability and reflux control are crucial because of its non-adhesive, gradual polymerizing qualities.

Because onyx is viscous and non-adhesive, it can be injected slowly and carefully, lowering the danger of catheter adhesion and unintended embolization. Although glue polymerizes quickly, it works particularly well in intranidal aneurysms and relatively small vessels.

Larger areas of the lesion can be occluded in a single session thanks to Onyx’s greater penetration into the nidus of AVMs. For some intranidal aneurysms where catheter access is restricted, glue may be preferable.

Because Onyx’s radio-opacity enables continuous visibility during injection, operators can accurately monitor embolization to prevent complications. This makes embolization safer and more thorough.

Compared to earlier embolics, these drugs offer more treatment options with less risks for brain AVMs, dural arteriovenous fistulas, vascular tumors, and peripheral lesions.

Compared to glue, onyx causes less vascular inflammation and vessel wall damage, which improves patient tissue tolerance and may result in fewer problems.

Compared to quick polymerizing glue, onyx makes the process safer and more flexible by enabling the operator to pause injections without catheter trapping.

Research indicates that the combination or selective use of these medications improves the overall prognosis of patients by achieving greater cure rates for AVMs and fistulas with minimal morbidity and mortality.