1. Setting Up and Positioning
Usually in a comfortable position, the patient lies down. Depending on how visible the lesion is, ultrasonography, mammography, or MRI guidance are used to pinpoint its location.

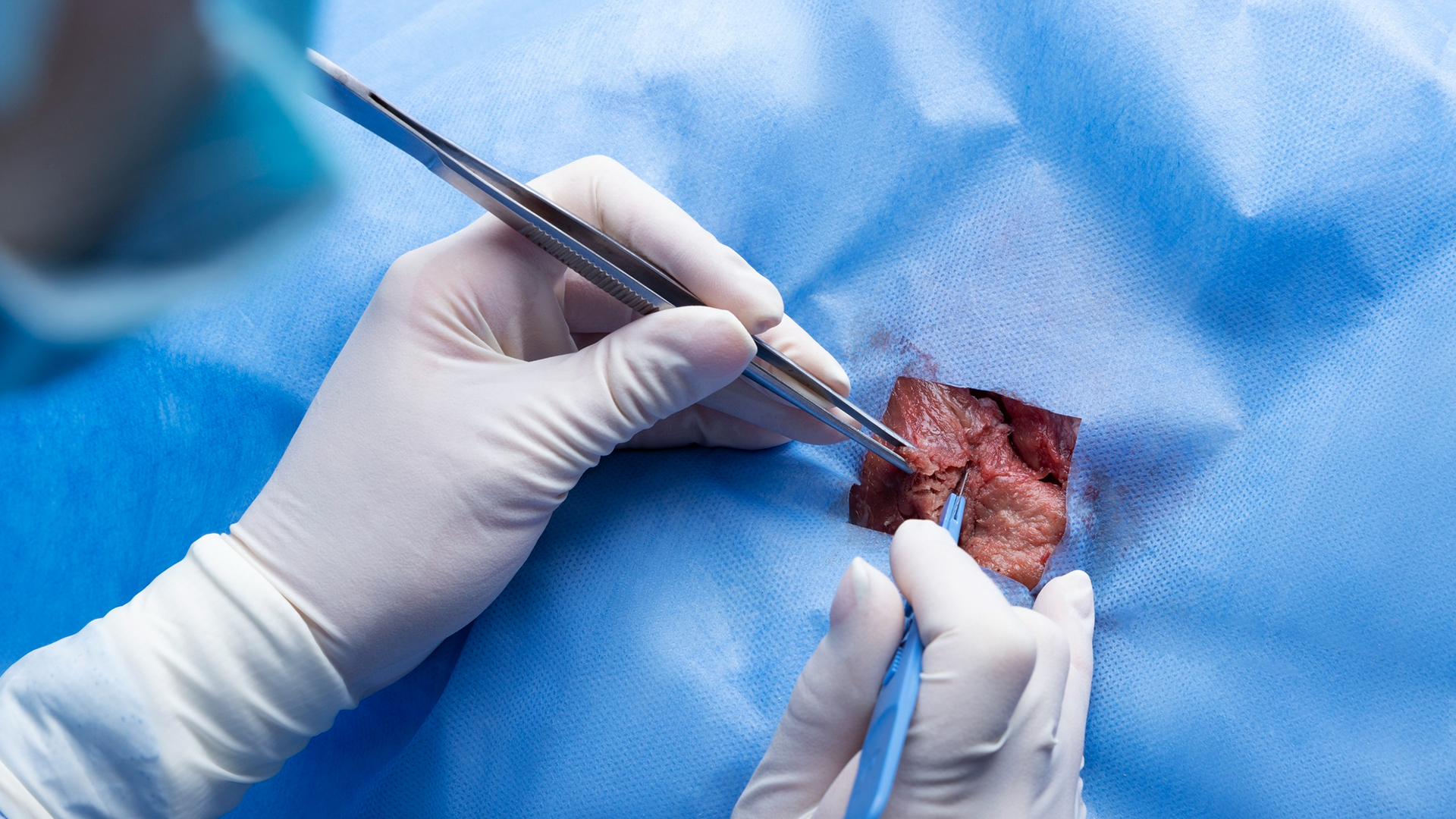
Usually in a comfortable position, the patient lies down. Depending on how visible the lesion is, ultrasonography, mammography, or MRI guidance are used to pinpoint its location.
To ensure a painless operation, local anesthetic is given around the biopsy site to numb the skin and tissue.
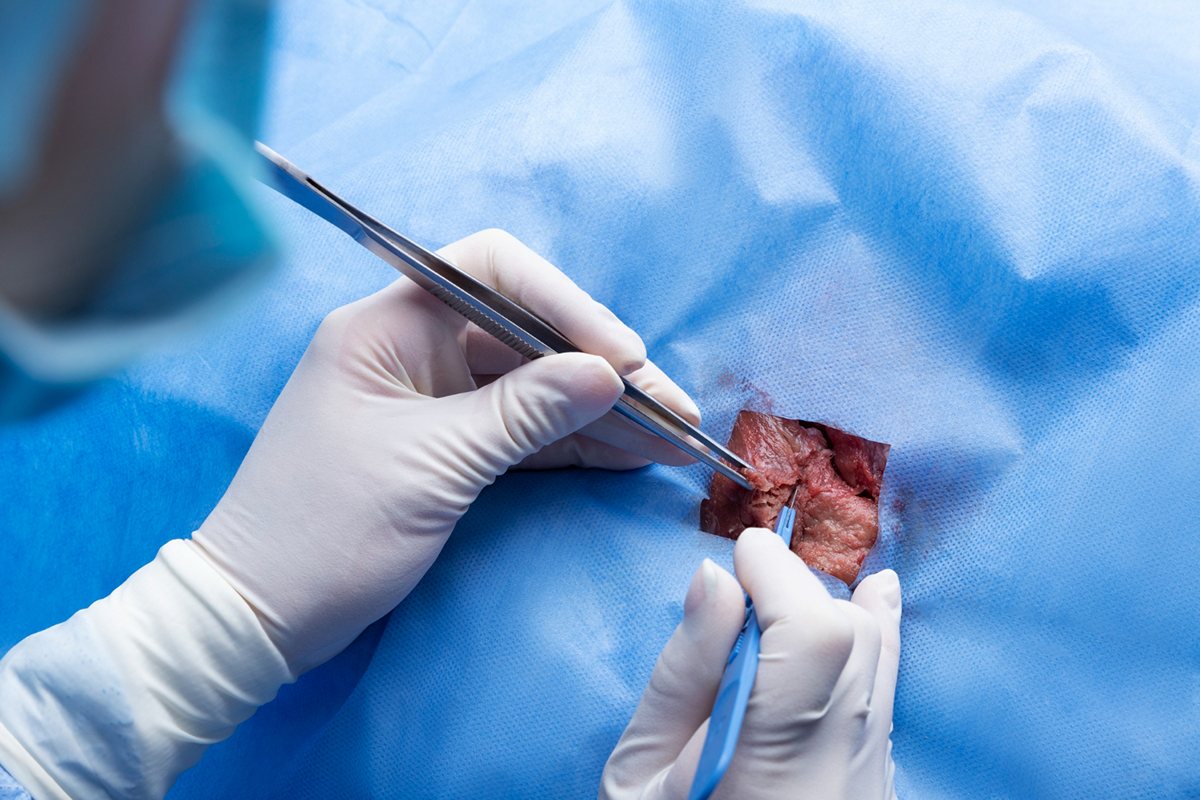
A little (3–5 mm) skin incision is made. Through this incision, a specialized vacuum-assisted biopsy needle is introduced and precisely guided to the lesion being imaged.
Tissue is drawn into the needle chamber by the device's suction mechanism, and the tissue sample is removed by a revolving cutter. One needle insertion can be used to collect many samples.
Excision biopsies minimize the necessity for surgical removal by sequentially sampling the whole lesion or aberrant tissue.
If the lesion is entirely excised, a small titanium marker may be positioned at the biopsy site to pinpoint the area for future reference.
To stop any bleeding, the needle is removed and pressure is administered. The site of the incision is covered with a little bandage.
Patients usually return home the same day after a brief observation for bleeding or problems. Over-the-counter medications are used to manage the slight pain.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Benign breast tumors such as fibroadenomas, tiny cysts, papillomas without atypia, radial scars, and other benign lesions that do not require surgical removal are best removed with VAEB.
In order to minimize the necessity for open surgery, it is utilized for biopsies and the excision of high-risk or borderline lesions like papillomas, lobular neoplasia, flat epithelial atypia, and atypical ductal hyperplasia.
Suitable for lesions found by imaging that need to be diagnosed or removed, such as ultrasound-visible lesions and clustered microcalcifications under stereotactic guidance.
Compared to core needle biopsy, VAEB offers bigger, more representative tissue samples, improving diagnostic precision and lowering sampling error.
especially helpful for people who wish to avoid the risks, healing period, and scars that come with typical surgical excision.
Lesions less than 2.5–3 cm are best suited for the device’s full excision.
This is helpful when previous biopsies were inconclusive or when clinical suspicion endures in spite of negative or unclear results.

VAEB causes less tissue damage and scarring because it only requires a tiny incision (3–5 mm) and does not require open surgery.

improves diagnostic accuracy, particularly for tiny, non-palpable, or microcalcified breast lesions, by enabling bigger, contiguous tissue samples with fewer needle insertions.

Benign and some high-risk lesions can be fully removed with VAEB, frequently eliminating the need for further surgical excision.

Compared to traditional core needle biopsy, VAEB reduces the likelihood of false negatives and the need for repeat biopsies because of the quality and quantity of tissue collected.

Compared to surgical biopsy, patients recover more quickly and with less pain and suffering, enabling them to return to their regular activities sooner.

Compared to surgical excision, the precision method and little incision produce better cosmetic results with less scarring.

High patient satisfaction with less anxiety as a result of quicker diagnosis and treatment and less invasive techniques.