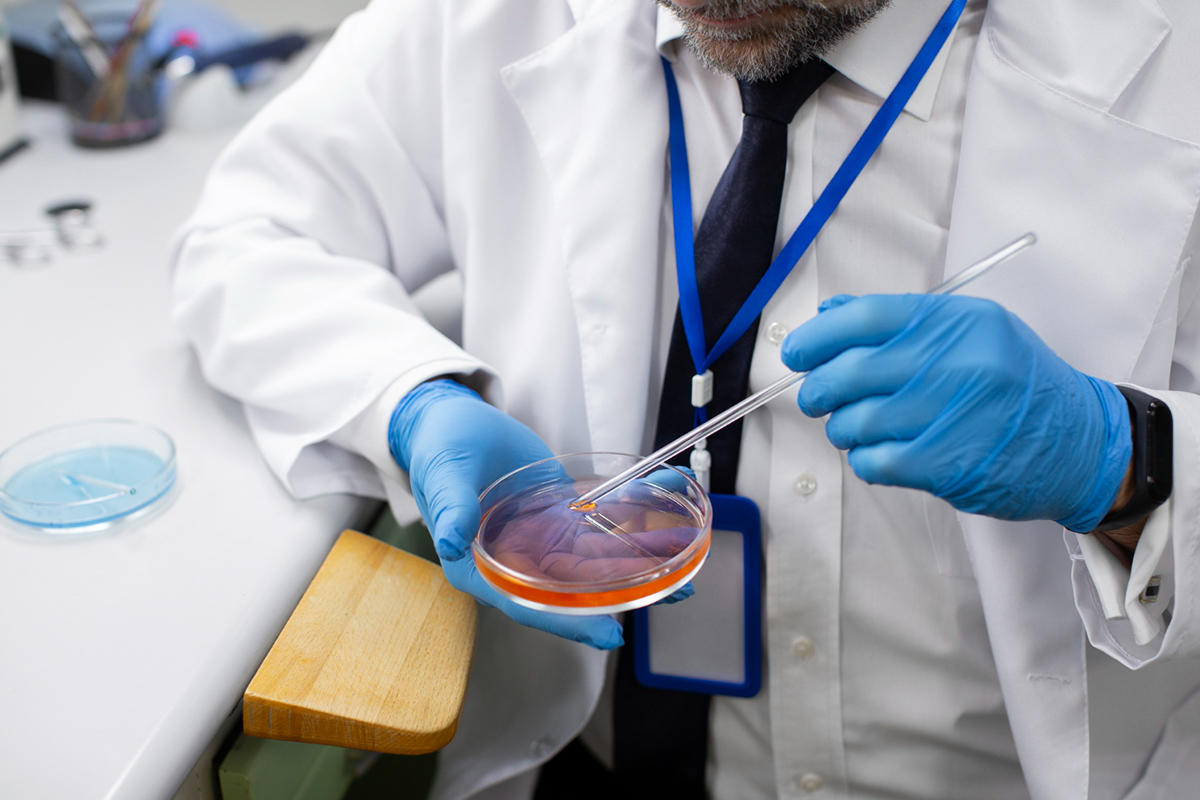
1. Positioning and Preparing the Patient
In order to expose the breast area that will be biopsied, the patient lies comfortably on the examination table, usually supine or slightly turned to the side.

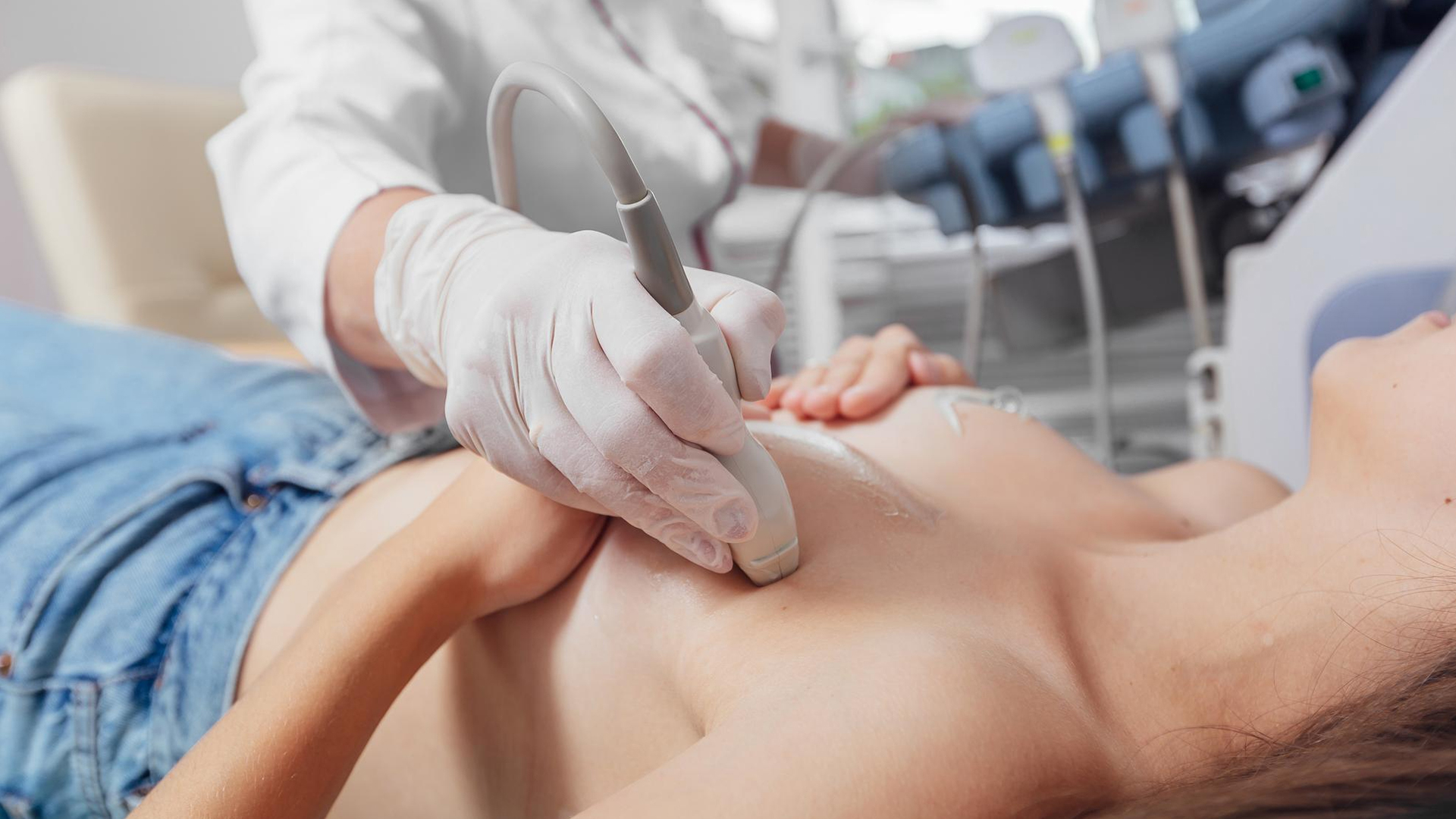
In order to expose the breast area that will be biopsied, the patient lies comfortably on the examination table, usually supine or slightly turned to the side.
The skin over the mass is treated with ultrasound gel. To locate and see the lump in real time, a high-frequency linear ultrasound transducer is applied to the breast.
An antiseptic solution is used to clean the biopsy site. To numb the lesion location, local anesthetic is injected into the surrounding skin and deeper tissues.
To make it easier for the biopsy needle to get through, a little (2–3 mm) skin incision is made. The biopsy needle is carefully inserted into the lesion through the incision while being continuously guided by ultrasonography.
Tissue samples are extracted using vacuum-assisted biopsy equipment or core needle biopsy. Repositioning the needle within the lesion allows for the collection of many samples (often 6–12) for sufficient representation.
For histological examination, tissue cores are gathered in formalin containers. To capture heterogeneity, samples may be obtained from several lesion locations.
To reduce bleeding and hematoma formation, pressure is applied over the biopsy site for five to ten minutes after the needle is removed. A sterile dressing is applied to the area.
For a limited while, the patient is monitored for any consequences, such as blood, discomfort, or allergic responses. Avoiding physically demanding activities and maintaining the site's cleanliness are two possible instructions.
The patient returns for a follow-up visit to discuss the results and future treatment after the tissue is sent to pathology.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Ideal for palpable or non-palpable solid masses seen after a physical examination, mammography, or ultrasound that are suggestive of cancer or have an unclear diagnosis.
High suspicion lesions that require a histological diagnosis include masses, architectural deformation, or aberrant tissue alterations.
When aberrant or enlarged lymph nodes are found during breast cancer staging or metastatic assessment, an ultrasound-guided biopsy is recommended.
may be biopsy targets if stereotactic biopsy is not practical or accessible, particularly if the results are associated with mammography.
enables a conclusive pathology diagnosis to direct treatment, preventing needless surgery when benign or quickly confirming cancer.
Ideal for people who need a less invasive alternative to open surgical biopsy with less scarring and a speedier recovery.

By employing a tiny needle guided by ultrasound instead of an open surgical biopsy, the method reduces tissue damage and scarring.

Real-time imaging via ultrasound enables accurate needle insertion into the lesion, improving sampling safety and accuracy.

Because ultrasonography employs sound waves instead of mammography-guided biopsy, it is safer and radiation-free, especially for younger or pregnant women.

Appropriate for masses that are palpable and visible on ultrasonography but not felt clinically.

It lowers healthcare expenditures since it is less costly than surgical biopsy or MRI-guided biopsy.

helps with prompt and proper treatment planning by providing trustworthy tissue samples for diagnosis.

useful when sampling lesions close to the nipple, axilla, or chest wall, where other methods might be difficult.