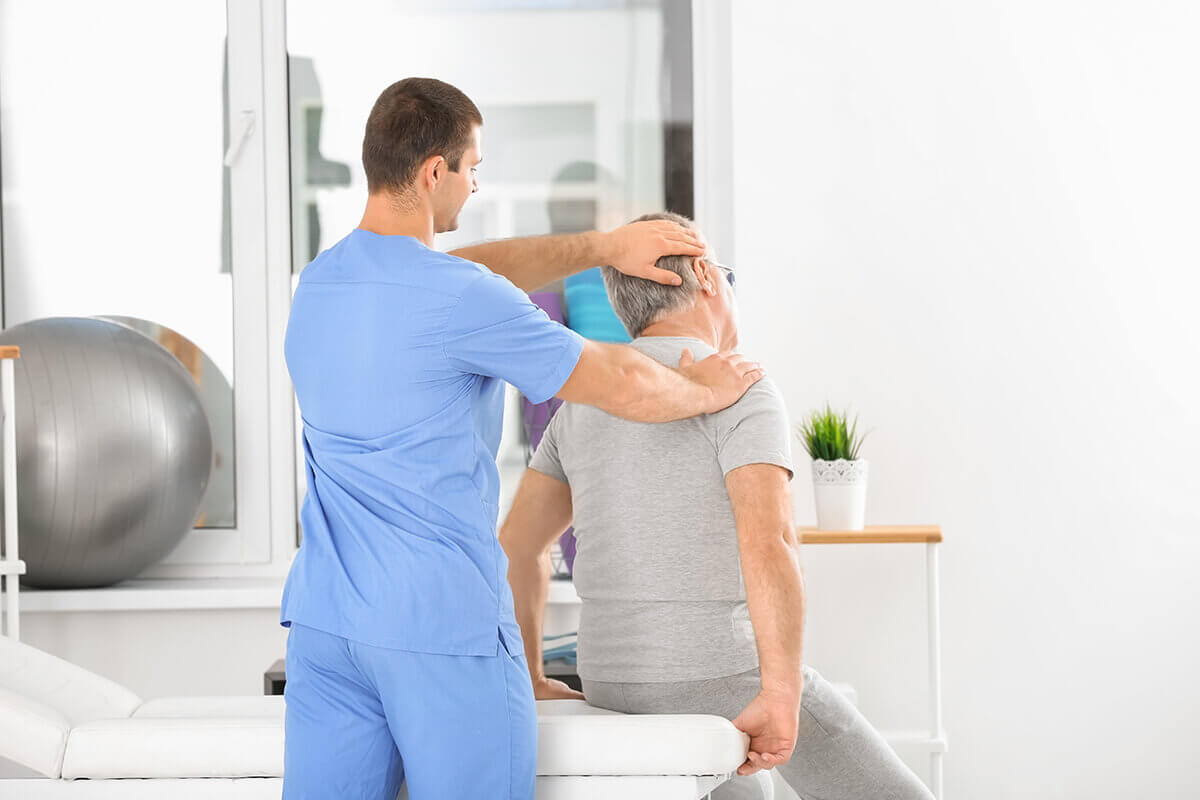
1. Preparing for the Procedure
Use ultrasound imaging to confirm the location, size, and features of the abscess. Get the patient's informed permission after outlining the procedure, its dangers, and its advantages.

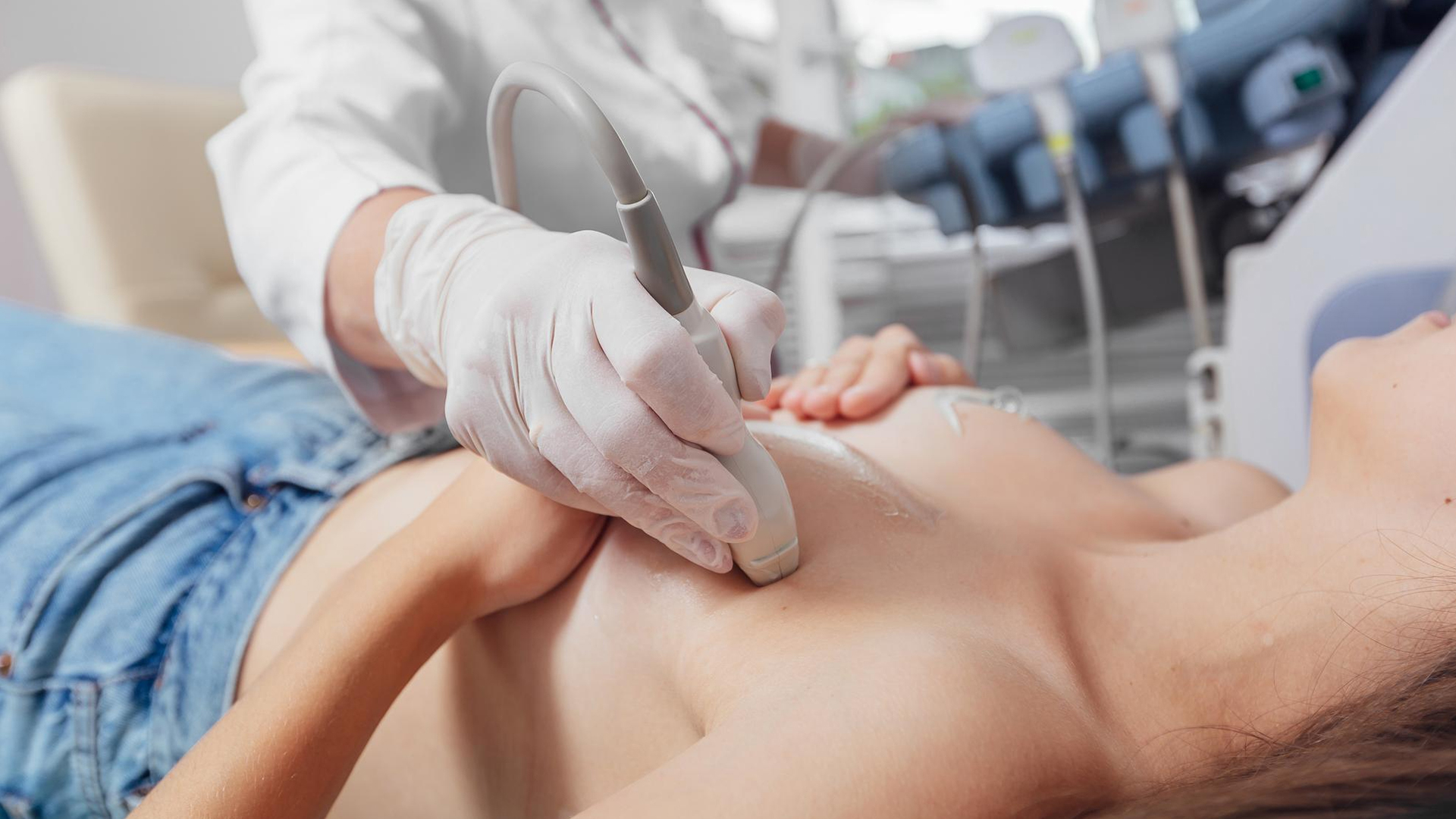
Use ultrasound imaging to confirm the location, size, and features of the abscess. Get the patient's informed permission after outlining the procedure, its dangers, and its advantages.
Place the patient in a comfortable position so that the abscess site is easily accessible Use an antiseptic solution to clean and sanitize the skin surrounding the abscess.
To numb the area surrounding the intended puncture site, apply local anesthetic (such as 1-2% lidocaine).
To determine the best puncture location and provide real-time guidance for needle placement, use an ultrasound probe.
Using ultrasound guidance, insert a needle of the appropriate gauge (usually 16–18 gauge) into the abscess cavity. Aspirate all of the pus using a syringe; the fluid is sent for sensitivity testing and culture.
Determine whether any fluid is still visible on the ultrasonography. Until the cavity is sufficiently drained, more aspirations may be made.
To reduce bleeding and hematoma formation, apply little pressure once the needle is removed. Use a sterile dressing to cover.
Prescribe the right antibiotics in accordance with the results of the culture and clinical judgment. Arrange for additional clinical and ultrasound assessments to track the clearance of the abscess.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Those with ultrasound-confirmed abscesses, such as those in the breast, abdomen, pelvis, or soft tissues where percutaneous access is possible.
Both types can be effectively managed with this less intrusive option, which has a high success rate compared to surgical incision and drainage.
can treat abscesses of any size; effective draining has been documented for abscesses greater than three centimeters. Repeated aspirations or alternate therapies may occasionally be necessary for multiloculated abscesses.
Particularly helpful for people who choose minimally invasive methods or for whom surgery is hazardous or impracticable.
Without Significant Tissue Damage or Skin Necrosis. Ideal for abscesses that don’t have extensive cellulitis or underlying skin necrosis; in these situations, traditional incision and drainage may be necessary.
Abscess resolution can be accomplished without open surgery by repeating the procedure several times with adequate patient tolerance.
Because of its affordability and accessibility, it is preferred in environments with limited surgical facilities.

minimizes stress and recuperation time by avoiding the need for an open surgical incision and drainage.

Cure rates of up to 91–100% have been reported in numerous investigations, indicating its effectiveness in draining abscesses, particularly those less than 5 cm.

minimizes scarring in comparison to surgical drainage, which is crucial in places that are sensitive to appearance, such as the breast.

Compared to surgical methods, patients have shorter recovery times and faster elimination of infection and inflammation.

Compared to surgery, there is less tissue damage and pain, allowing nursing mothers to continue nursing.

By visualizing needle insertion and drainage sufficiency, ultrasound guidance lowers the likelihood of recurrence and incomplete drainage.

In order to minimize hospital stays, the aspiration is typically done as an outpatient procedure that can be repeated if necessary.

Reduced risk of problems compared to conventional incision and drainage, including bleeding, infection, and fistula formation.

Less costly and requiring less hospital resources than surgical drainage.