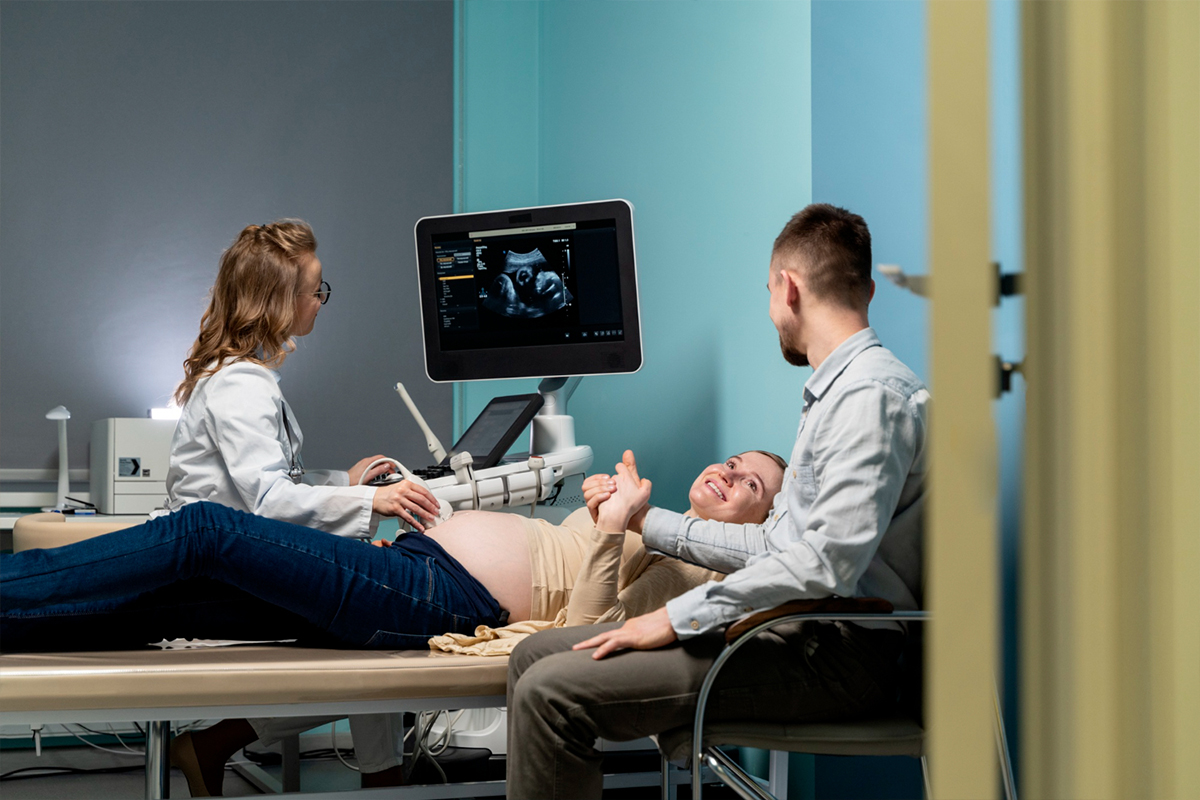
1. Positioning and Imaging of Patients
The kidney tumor is carefully located and the access site is planned using imaging, such as a CT scan, while the patient is positioned on the surgery table.

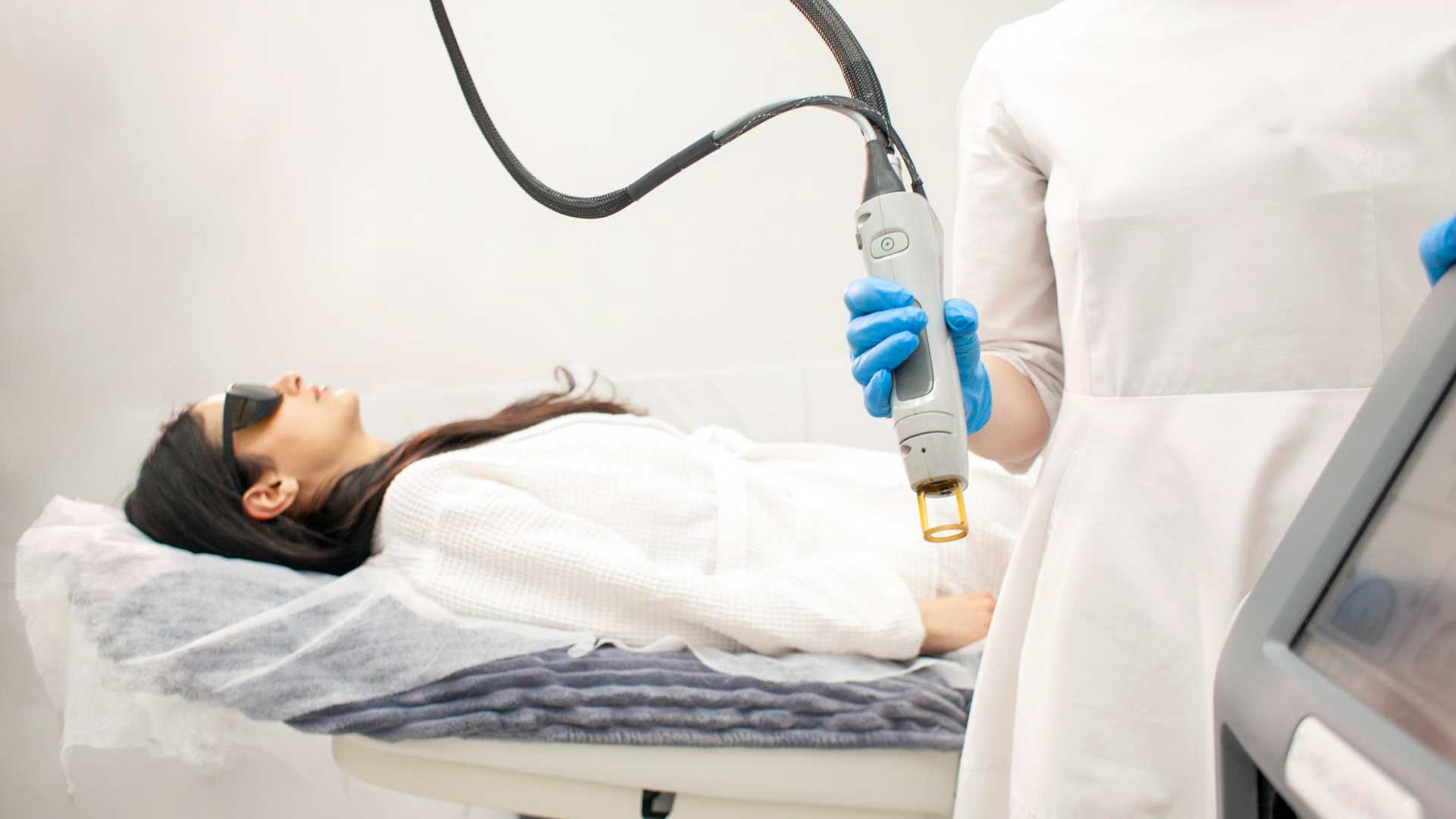
The kidney tumor is carefully located and the access site is planned using imaging, such as a CT scan, while the patient is positioned on the surgery table.
After sterilizing the skin above the access site, the area is numbed with local anesthetic. For the comfort of the patient, general anesthesia or conscious sedation may occasionally be used.
Under imaging guidance, one or more cryoablation probes are inserted directly into the tumor through a tiny skin puncture or incision.
Pressurized argon gas is delivered via the probes to produce intense cold and an ice ball that freezes the tumor. This is carried out via freeze-thaw cycles that alternate and usually last 30 minutes.
During freezing, imaging is done periodically to keep an eye on the growth of the ice ball and make sure the tumor is completely covered while safeguarding surrounding organs.
Following freezing, the probes are taken out, the entrance site is compressed, and a dressing is applied. After a brief stay or the same day, the patient is typically released after being checked for complications.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Patients with tiny kidney tumors, usually less than 4 cm in size (stage T1a or T1b), where localized treatment is effective with low invasiveness, are the main candidates for cryoablation.
Due to the increased risk of complications, it is best suited for individuals who are elderly, have serious medical conditions, or have low renal function and are therefore not candidates for standard surgery.
Because cryoablation preserves surrounding healthy tissue, it is beneficial for patients who need to preserve kidney tissue, such as those with a single kidney or genetic disorders generating many tumors.
Cryoablation is becoming a more viable alternative, even for younger or healthier patients who want to avoid the morbidity that comes with surgical removal.
To ensure that the tumor’s location and size are suitable for a safe and effective ablation, careful imaging and multidisciplinary assessment are necessary for effective patient selection.

With cryoablation, kidney tumors can be precisely targeted and frozen with little harm to the surrounding healthy tissue. As much normal kidney function as feasible is preserved by this focused strategy.

Compared to typical surgery, the operation is carried out percutaneously through tiny skin punctures, which reduces discomfort, scars, and recovery time. After a brief hospital stay, many patients return home the same day.

Even in patients with a single kidney or impaired renal function, cryoablation effectively cures malignancies while preserving overall kidney function.

According to studies, cryoablation is a safer choice for people who are unfit for invasive operations because it has less side effects than surgery, such as bleeding or urine leakage.

In cases of recurrence, cryoablation can be safely repeated, enabling continued treatment of kidney malignancies without appreciable extra risk.

Due to shorter hospital stays and fewer complications, cryoablation is more cost-effective than surgery.

Long-term monitoring shows that cryoablation has cancer control rates that are similar to those of partial nephrectomy, with excellent survival and low recurrence rates.