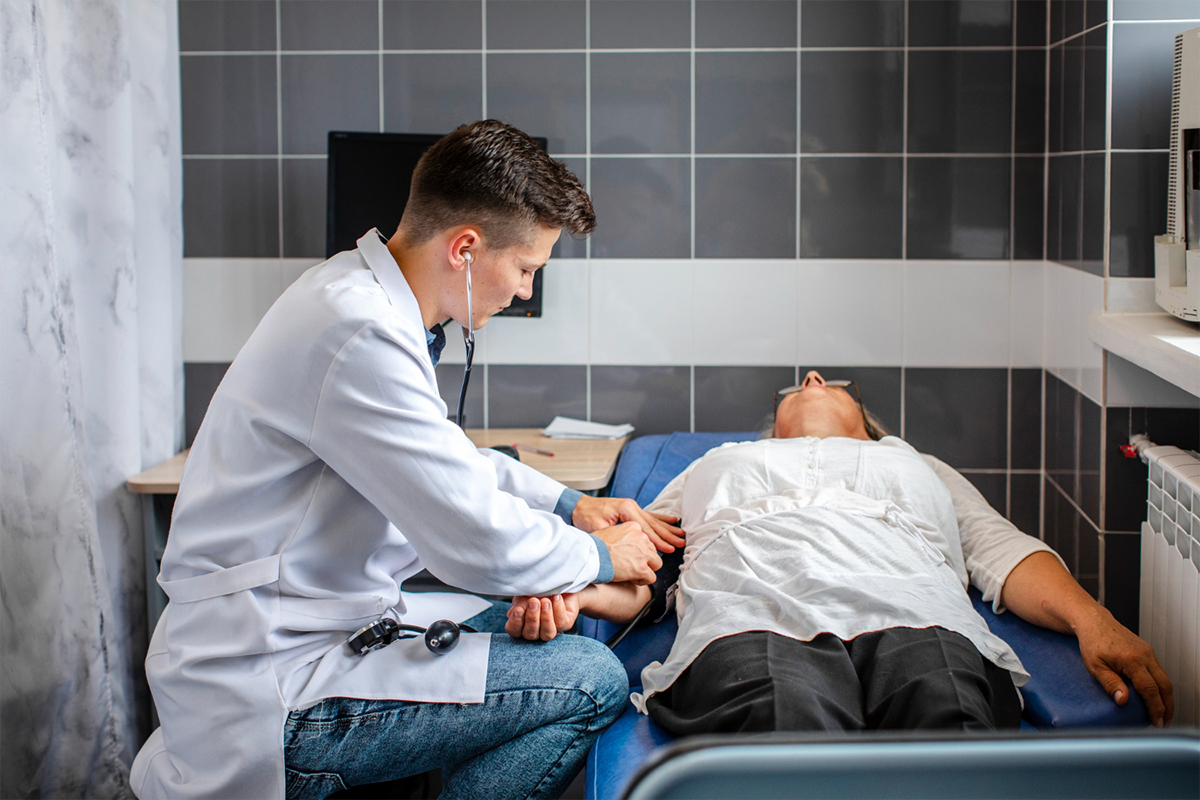
1. Positioning and Preparing the Patient
To help with fluid outflow, the patient is seated either upright or at a 45-degree angle. Cleaning and sterilization are done in the procedure area on the chest wall.

To help with fluid outflow, the patient is seated either upright or at a 45-degree angle. Cleaning and sterilization are done in the procedure area on the chest wall.
To numb the insertion site, local anesthetic is injected into the skin, subcutaneous tissue, and pleura.
To aspirate pleural fluid, a small-bore catheter or needle is placed between the ribs into the pleural space under fluoroscopic or ultrasound guidance.
To relieve symptoms, pleural fluid is gradually drained; if the patient coughs or has chest pain, the procedure usually stops. The Seldinger procedure can be used to introduce a chest tube for bigger effusions.
A dilator is inserted into the pleural cavity by a tiny incision and a guidewire. The wire is then withdrawn after a chest drain tube has been advanced over it and positioned correctly. Sutures are used to secure the tube.
To enable constant drainage and keep air out of the pleural space, the chest tube is attached to a water-seal drainage system. Imaging and clinical evaluation are used to track the position and function.
After sufficient drainage, a sclerosing substance, such as talc or doxycycline, is injected into the pleural space via the chest tube if pleurodesis is planned (to avoid recurring effusions). In order to evenly disperse the agent, the patient is moved while the tube is momentarily constricted.
Patients are watched for discomfort, respiratory status, and problems while the drain site is wrapped and the line is fastened. Once drainage is low and imaging confirms lung growth, the chest tube is withdrawn.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Peritoneal catheter implantation is the best option for patients with recurrent or refractory ascites brought on by cancer, liver cirrhosis, or other conditions that necessitate frequent draining for symptom relief.
It is appropriate for individuals with end-stage liver disease or advanced cancer who have severe discomfort, distension in the abdomen, trouble breathing, or early satiety due to ascitic fluid accumulation.
Tunneled indwelling peritoneal catheters are beneficial for patients who need or prefer to treat ascites at home in order to avoid invasive procedures and recurrent hospital stays.
This method is appropriate for patients in whom repeated large volume paracentesis is impractical, inefficient, or linked to problems including bleeding or infection.
used prior to procedures such as liver biopsy or TIPS to maximize ascitic fluid outflow.

Ascitic fluid can be drained continuously or intermittently thanks to the catheter, which quickly relieves symptoms including breathing difficulties, discomfort, and distension in the abdomen.

By enabling patients to control fluid drainage at home, it lessens the need for invasive large volume paracentesis and recurrent hospital stays.

Patients have better appetite, mobility, and quality of life with fewer hospital admissions when ascites build-up is adequately controlled.

Indwelling catheter drainage lowers the risks of infection, hemorrhage, and protein loss associated with many punctures when compared to repeated paracentesis.

beneficial for individuals who need long-term fluid management due to intractable ascites, particularly those with severe liver disease or cancer.

The timing and volume of drainage can be adjusted by patients or caregivers, providing flexibility based on symptoms.