1. Getting Ready for Patients
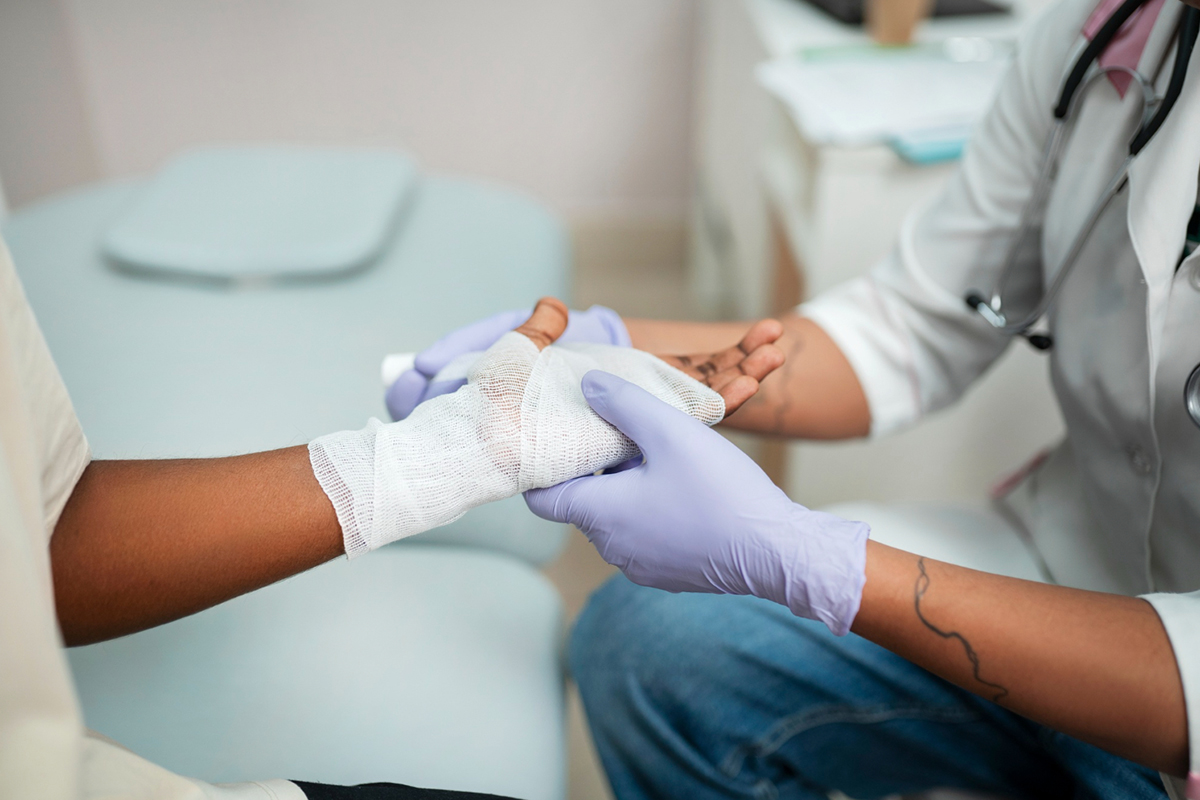
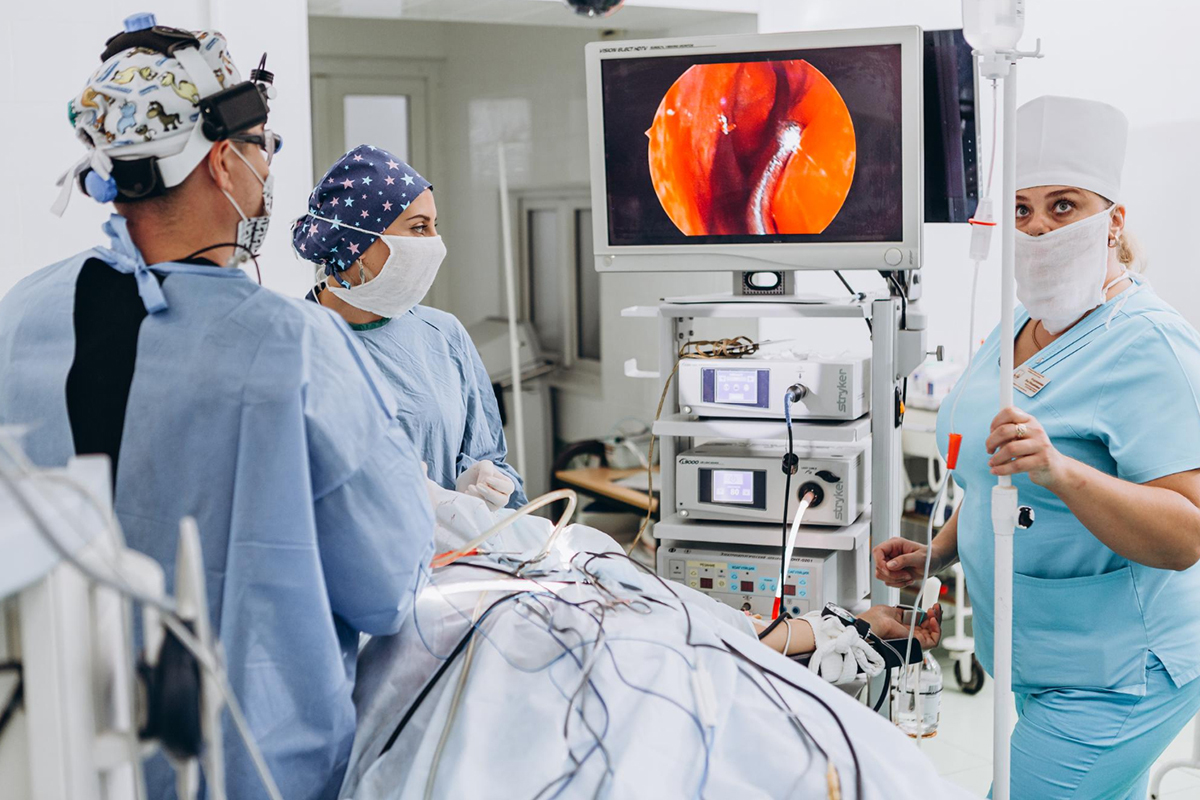
The patient is placed in a comfortable position, usually on their back. After cleaning and sterilizing the abdomen, local anesthetic is injected at the puncture site.


The patient is placed in a comfortable position, usually on their back. After cleaning and sterilizing the abdomen, local anesthetic is injected at the puncture site.
Usually beneath the umbilicus, a little skin incision measuring two to three centimeters is created. The anterior rectus sheath or peritoneum can be reached by blunt dissection in a sterile manner.
A needle or cannula is carefully placed into the peritoneal cavity while avoiding the bowel and vasculature using ultrasound guidance. Free fluid aspiration or saline infusion/aspiration are used to confirm entrance.
The needle or cannula is used to implant a guidewire into the peritoneal space. To make catheter passage easier, the tract is serially dilated using dilators.
Using tunneling devices, the catheter is subcutaneously tunneled to the exit site, and cuffs are deployed at specific points to prevent infection and provide a secure position.
Sterile saline is used to flush the catheter in order to assess its patency and drainage capabilities. Sterile dressings are placed when sutures or adhesive strips are used to seal incisions.
Patients are given instructions for catheter maintenance and warning signals of problems, and the catheter exit site is bandaged. As needed, the catheter enables recurrent draining of ascitic fluid.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Patients with recurrent malignant ascites that cause symptoms like nausea, dyspnea, discomfort, and distension of the abdomen can benefit from this surgery, particularly if repeated large volume paracentesis is necessary.
Tunneled peritoneal catheter implantation is beneficial for symptom palliation in patients with advanced abdominal or pelvic cancers who frequently accumulate ascitic fluid.
Peritoneal catheters are helpful for those who need frequent ascitic fluid drainage to regulate their symptoms but want to avoid frequent hospital stays or invasive procedures.
Peritoneal catheter drainage is an option for patients who do not respond well to diuretics or who are not suitable for medical treatment of ascites.
Tunneled catheter systems that permit intermittent drainage are beneficial for patients who can manage their ascitic fluid at home on their own or with the assistance of caretakers.
Refractory ascites instances with crippling symptoms can be successfully treated for both malignant and non-malignant conditions (such as cirrhosis).

Ascites-related abdominal distension, pain, breathing difficulties, and early satiety can be relieved continuously or sporadically by using a peritoneal catheter for ascitic fluid drainage.

It lessens the need for invasive big volume paracentesis procedures and frequent hospital visits by enabling patients to manage ascites drainage at home.

Compared to recurrent needle paracentesis, the insertion of tunneled peritoneal catheters is less intrusive, has a favorable safety profile, and causes less pain and problems like infection or leaking.

Patients’ overall quality of life is enhanced by symptom control, fluid management autonomy, and avoidance of the discomfort brought on by recurrent fluid accumulation.

When ascites recurs quickly, the catheter can be utilized for continuous draining in cases of refractory or malignant ascites, offering a useful and patient-friendly option.

Modern catheter systems are made to drain easily and need little technical expertise, enabling patients and caregivers to administer the device at home.

Although there is a chance of consequences like infection or catheter malfunction, these risks are usually outweighed by the overall advantages in terms of symptom management and improved living.