1. Anesthesia and Preparation
Local anesthetic is given at the vascular access location, which is typically the arm or groin, once the patient has been prepared. To help the patient relax, little sedation may be administered.

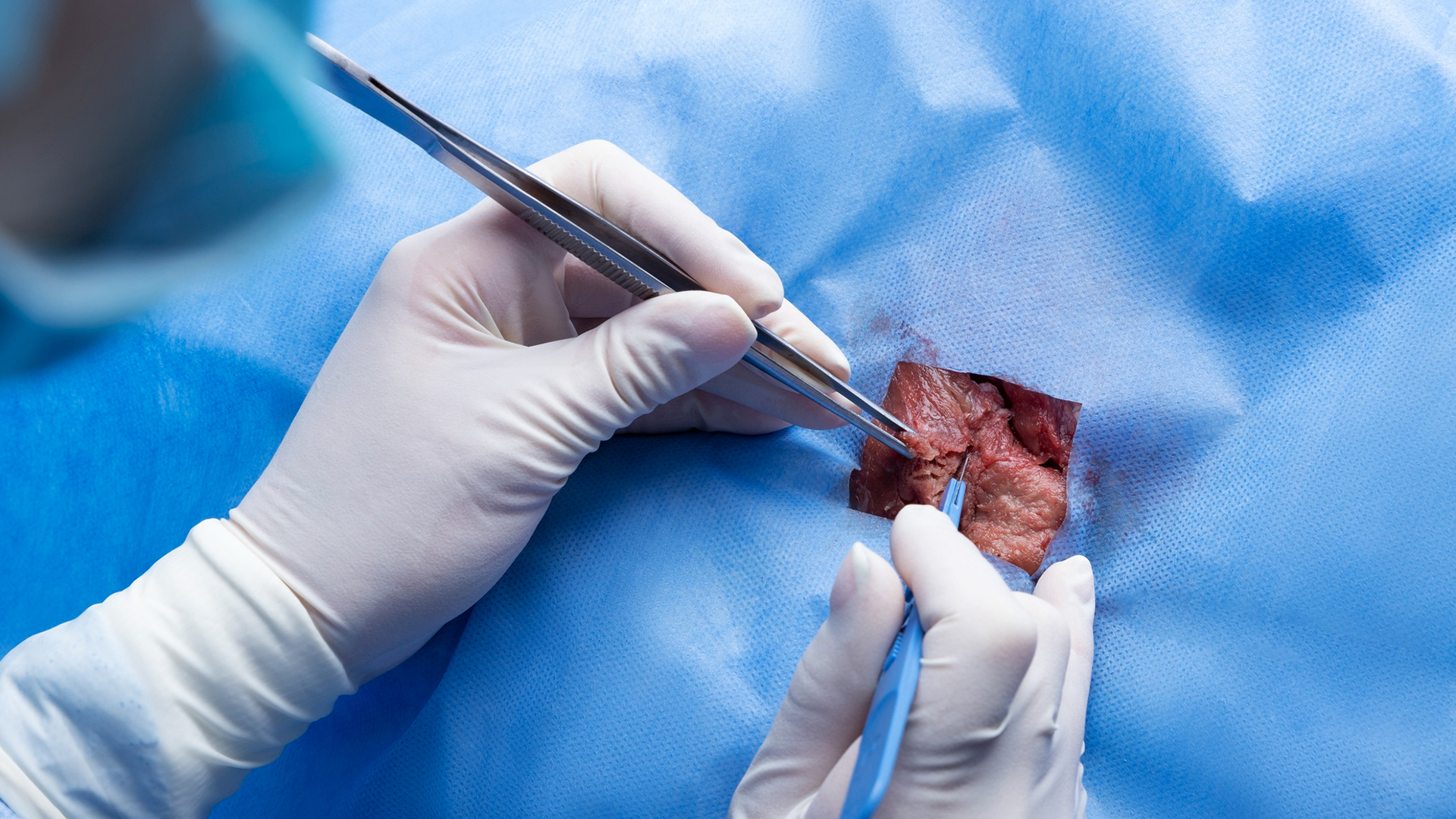
Local anesthetic is given at the vascular access location, which is typically the arm or groin, once the patient has been prepared. To help the patient relax, little sedation may be administered.
A catheter with a guidewire is introduced into the artery after a little incision is created. The guidewire is moved to the location of arterial plaque or obstruction by passing through the blood arteries.
The atherectomy catheter is guided to the constricted or calcified arterial segment using fluoroscopy, a real-time X-ray. To see the lesion, contrast dye may be injected.
A cutting, grinding, or laser device at the catheter tip is triggered based on the kind of atherectomy (rotational, directed, orbital, or laser). This restores vascular patency by shaving, grinding, or vaporizing the plaque.
To stop embolism downstream, the catheter system collects or flushes away the debris produced during plaque removal.
To further open and sustain the artery following an atherectomy, angioplasty (balloon dilation) or stent implantation may be carried out.
The catheter and guidewire are taken out after the surgery is finished. A bandage or closure device is placed on the access site when pressure is applied to halt the bleeding.
Vital signs, access site bleeding, and any consequences are all observed in the patient. Usually, recovery entails observation for several hours or perhaps overnight.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Balloon angioplasty alone may not be successful for ideal candidates with complex plaque morphology because of hard, calcified deposits that need to be modified before dilatation or stenting.
People with PAD symptoms, such as claudication or critical limb ischemia, who have lesions that are resistant to routine angioplasty or stenting, particularly lengthy or eccentric lesions.
When balloon angioplasty is unsuccessful or inappropriate, atherectomy might be used as a primary or adjunctive treatment.
For example, in chronic complete occlusions, unprotected left main disease, ostial lesions, or while getting ready to implant a bioresorbable scaffold.
By debulking proliferative tissue, atherectomy can sometimes help treat restenotic lesions inside previously implanted stents.

Instead of requiring open surgery, an atherectomy is carried out through a tiny puncture, which results in less pain, a decreased chance of complications, and a speedy return to normal activities, typically the same day or within a few days.

Atherectomy physically eliminates or debulks plaque, making the artery more open and possibly lowering the risk of restenosis, in contrast to balloon angioplasty, which presses plaque against the arterial wall.

By greatly enhancing circulation, an atherectomy relieves symptoms of peripheral artery disease, including numbness, coldness, leg discomfort (claudication), and non-healing wounds.

Athectomy lowers the risk of serious infections and tissue loss by reestablishing blood flow to the limbs, which can ultimately avert limb amputation in cases of severe PAD.

It improves technical success and results by treating stubborn, calcified, or long-segment blockages that are challenging to treat with balloon angioplasty alone.

When necessary, plaque removal with atherectomy can maximize stent expansion and make stent implantation simpler.

For many people, atherectomy is a safer option than open surgery since it causes less blood loss, less discomfort, and fewer infections.