1. Getting Ready and Getting Access
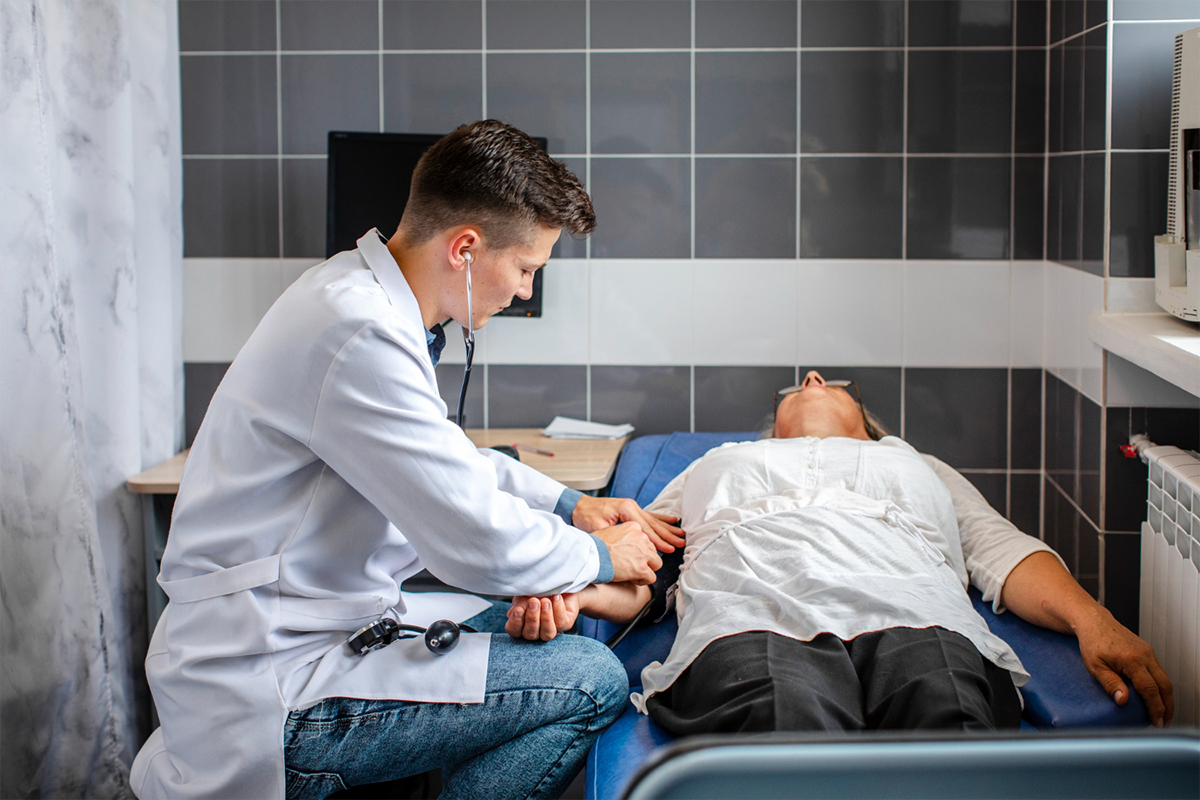
In a sterile setting, the patient is positioned and prepared. The access site, typically the wrist or groin is where local anesthetic is given. To introduce a vascular sheath, a little incision is made.


In a sterile setting, the patient is positioned and prepared. The access site, typically the wrist or groin is where local anesthetic is given. To introduce a vascular sheath, a little incision is made.
The location of the arterial constriction or restenosis is reached by carefully passing a guidewire through the blood arteries.
To widen the constricted artery and get the vessel ready for medication distribution, a normal balloon angioplasty may be carried out first. In order to push the plaque away, a standard balloon is inflated at the location.
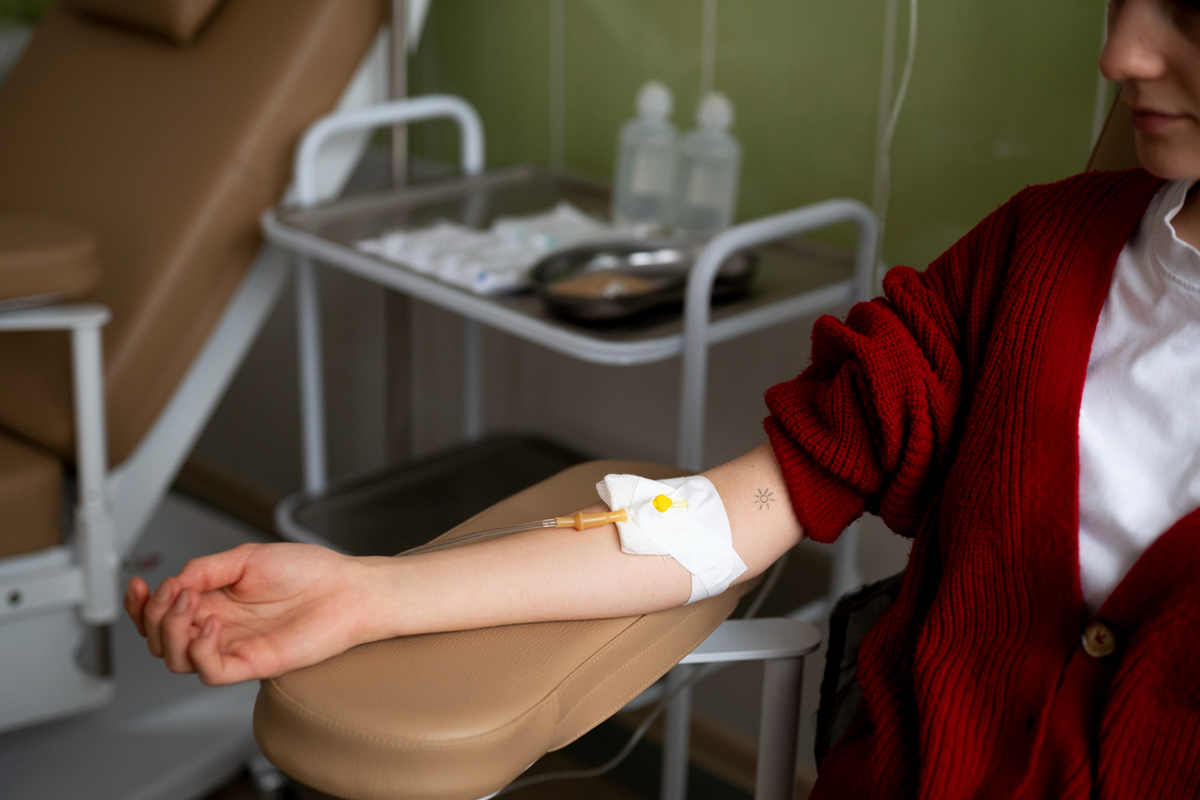
The target lesion is reached by advancing the drug-coated balloon catheter across the guidewire.
The drug-eluting balloon is inflated at nominal pressure for around 30 to 60 seconds. The antiproliferative medication (usually paclitaxel) can be directly transferred from the balloon surface to the arterial wall thanks to this inflation.
The balloon and catheter are withdrawn once the medication is administered.
The access site is bandaged when pressure is applied to halt the bleeding. If necessary, closure mechanisms may be employed.
After being checked for any immediate issues, the patient is kept under observation as they heal.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





DEB angioplasty reduces the dangers associated with multiple stents by effectively treating restenosis within previously implanted stents without the need for additional metal layers.
appropriate for coronary arteries with a diameter of less than 3.0 mm, where restenosis rates and stent insertion hazards are greater; DEB administers antiproliferative medications while minimizing vascular damage.
Drug delivery and vascular dilatation are made possible without the need for a side branch stent in complex bifurcation sites where stenting might be difficult.
There is growing evidence that DEB-only angioplasty can reduce foreign body implantation, preserve vessel vasomotion, and treat some new lesions.
Those who are at high risk of bleeding can benefit from DEB’s ability to shorten the period of necessary antiplatelet medication by avoiding stent implantation.
Additionally, DEB angioplasty is employed in peripheral arteries (such as the iliac and femoral) to minimize stent-related problems and prevent restenosis.
DEB offers a potentially safe and effective substitute for stent implantation in lesions that are prone to restenosis.

DEBs are removed after delivering antiproliferative medications directly to the artery wall during inflation, no metal scaffold is left behind. This lessens the long-term problems linked to stents by maintaining the natural flexibility and architecture of the vessels.

The danger of delayed blood clots (late stent thrombosis) and chronic inflammation associated with stent implants is reduced in the absence of a permanent foreign body.

Better spontaneous healing and constructive remodeling of the vessel wall are made possible by the absence of mechanical stress from stents.

When stent implantation is difficult or unwanted, DEBs can be used to treat in-stent restenosis, small vessel disease, bifurcation lesions, and several peripheral artery diseases.

Compared to stent-based therapies, patients frequently need antiplatelet drugs for shorter periods of time, which lowers the risk of bleeding.

DEBs improve long-term vessel patency by lowering restenosis rates when compared to balloon angioplasty alone.

DEBs help maintain vascular function, especially the capacity for vasodilation and constriction, by avoiding permanent implants.