1. Getting the Patient Ready and Observing
Heart rate, blood pressure, oxygen saturation, and pulse monitoring equipment are linked while the patient is positioned. Anesthesia or sedation is administered as required.

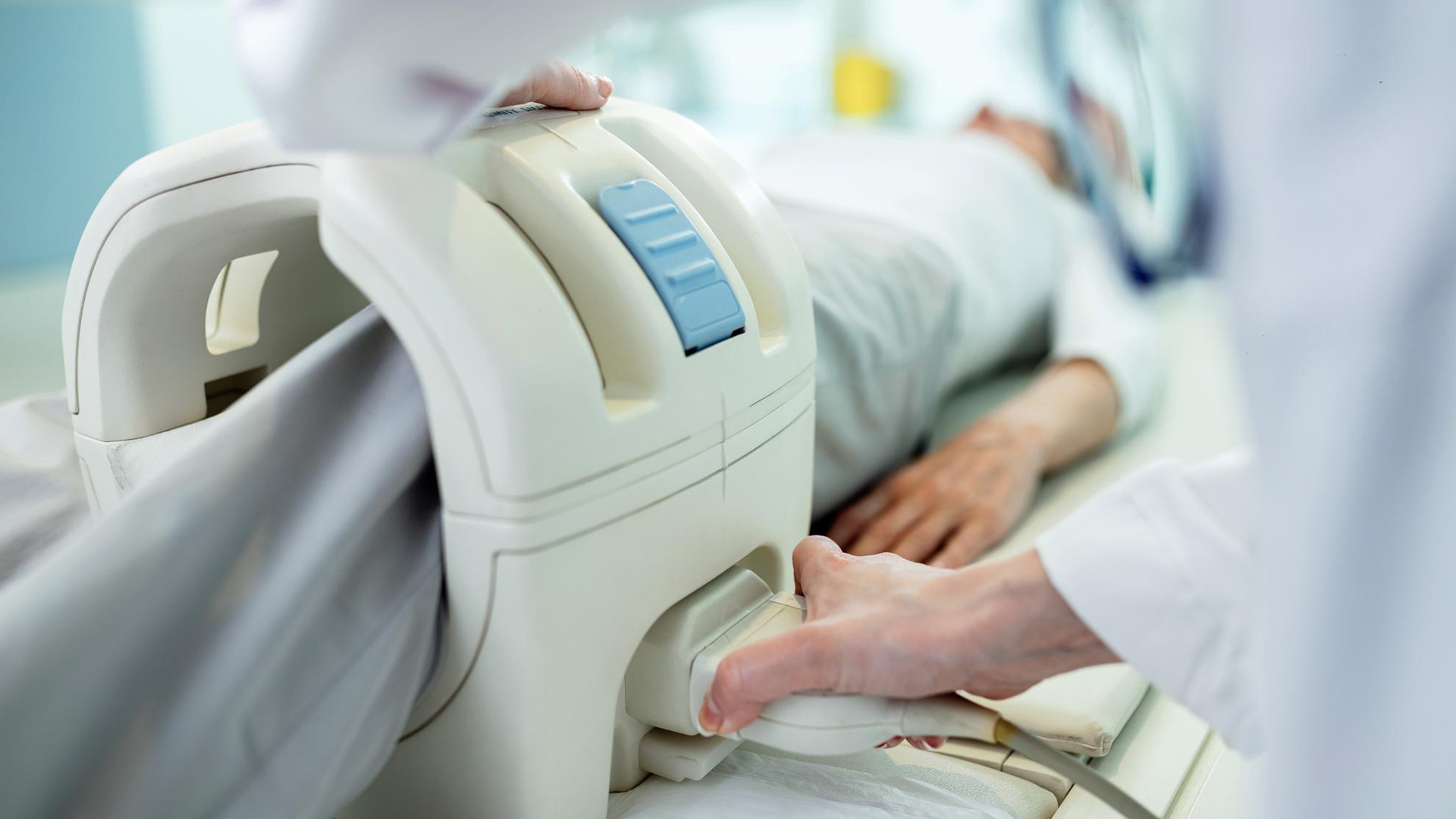
Heart rate, blood pressure, oxygen saturation, and pulse monitoring equipment are linked while the patient is positioned. Anesthesia or sedation is administered as required.
A catheter is put under local anesthesia into a blood vessel (vein or artery) after a minor incision is made, typically in the wrist or groin.
The catheter is moved through the vascular system to the target blood vessel that is causing bleeding, tumor blood supply, or vascular malformation using imaging guidance such as fluoroscopy, ultrasound, CT, or MRI.
In order to see the blood vessels and verify the location and size of the lesion or bleeding, contrast dye is injected.
Contrast is used in post-embolization imaging to verify effective blood flow stoppage and vascular blockage.
To stop the bleeding, the catheter is removed and the access site is compressed. It is possible to utilize closure devices.
For issues like discomfort, bleeding, or ischemia, the patient is closely watched. The degree and location of embolization determine the healing time.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





individuals who require targeted vascular occlusion due to aberrant blood vessel forms such as aneurysms or arteriovenous malformations (AVMs).
Patients with acute or chronic bleeding from trauma, gastrointestinal causes, or uterine fibroids not managed by traditional therapies.
tumors (such as hepatic, kidney, or uterine fibroids) that need to be devascularized in order to lessen symptoms or the danger of intraoperative bleeding.
It can alleviate symptoms and problems in certain cases of varicocele, pelvic congestion, or varicose vein embolization.
who match certain criteria and have not responded to medical therapy are considered to have benign prostatic hyperplasia (BPH).
Genicular artery embolization may be beneficial for certain individuals with persistent knee pain who are not responding to conservative therapies.

By avoiding huge incisions and significant surgery, embolization is carried out with a little needle puncture, which results in less discomfort and scars.

It minimizes harm to nearby healthy tissues for more successful treatment by accurately delivering embolic chemicals to the aberrant or bleeding arteries.

Embolization is safer for high-risk individuals and has less consequences and infection risk than surgery.

Unlike more invasive surgical procedures, most patients heal quickly and can resume their regular activities in a few days.

Embolization prevents potentially fatal bleeding by quickly controlling acute or chronic bleeding caused by trauma, tumors, or vascular abnormalities.

Embolization offers a non-surgical approach with similar efficacy and lower morbidity for a variety of disorders, including uterine fibroids, BPH, hemorrhoids, and tumors.

It decreases tumors or fibroids, lessens symptoms like pain and bleeding, and maintains organ function, often preventing removal.

In order to improve patient comfort and convenience, many embolization procedures are performed as outpatient operations or necessitate brief hospital stays.




















