1. Patient Preparation
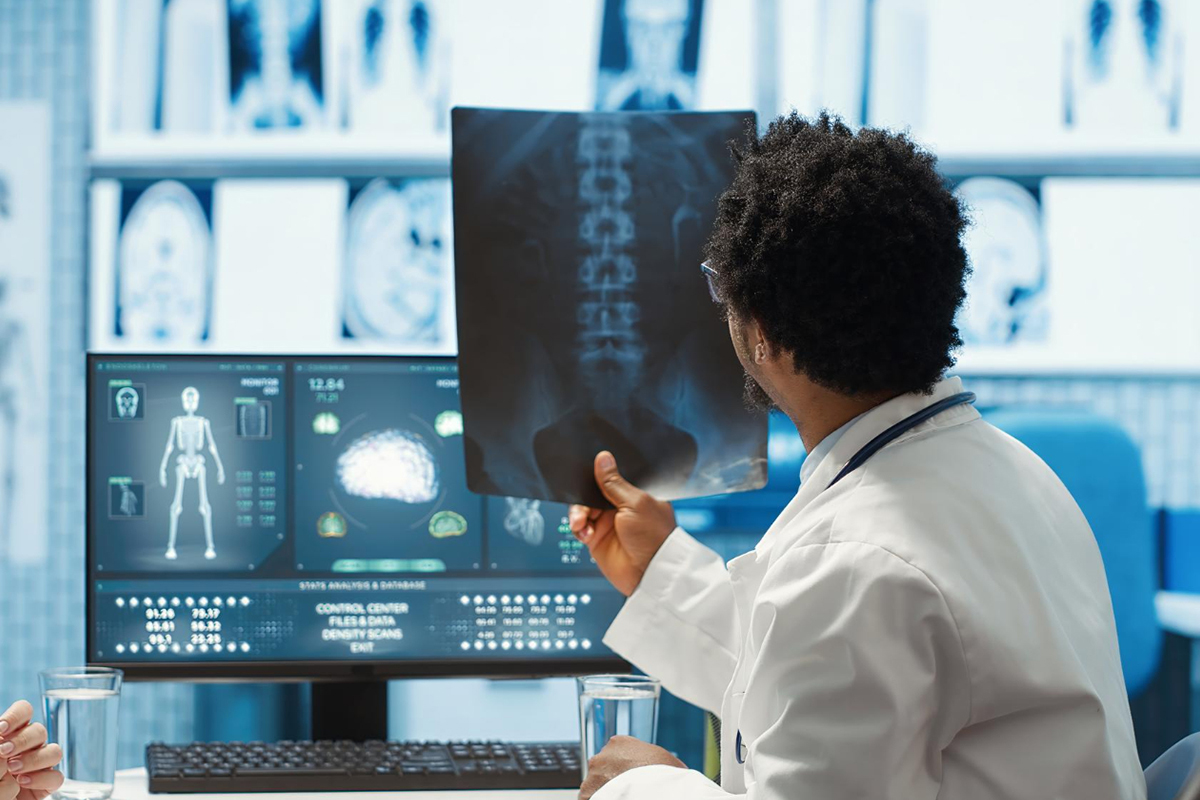
Detailed imaging (CT, MRI, angiography) is used in pre-procedural evaluation to evaluate the size, location, and vascular anatomy of aneurysms. To lower the risk of thromboembolism, dual antiplatelet therapy (aspirin and clopidogrel) is initiated several days before the surgery.