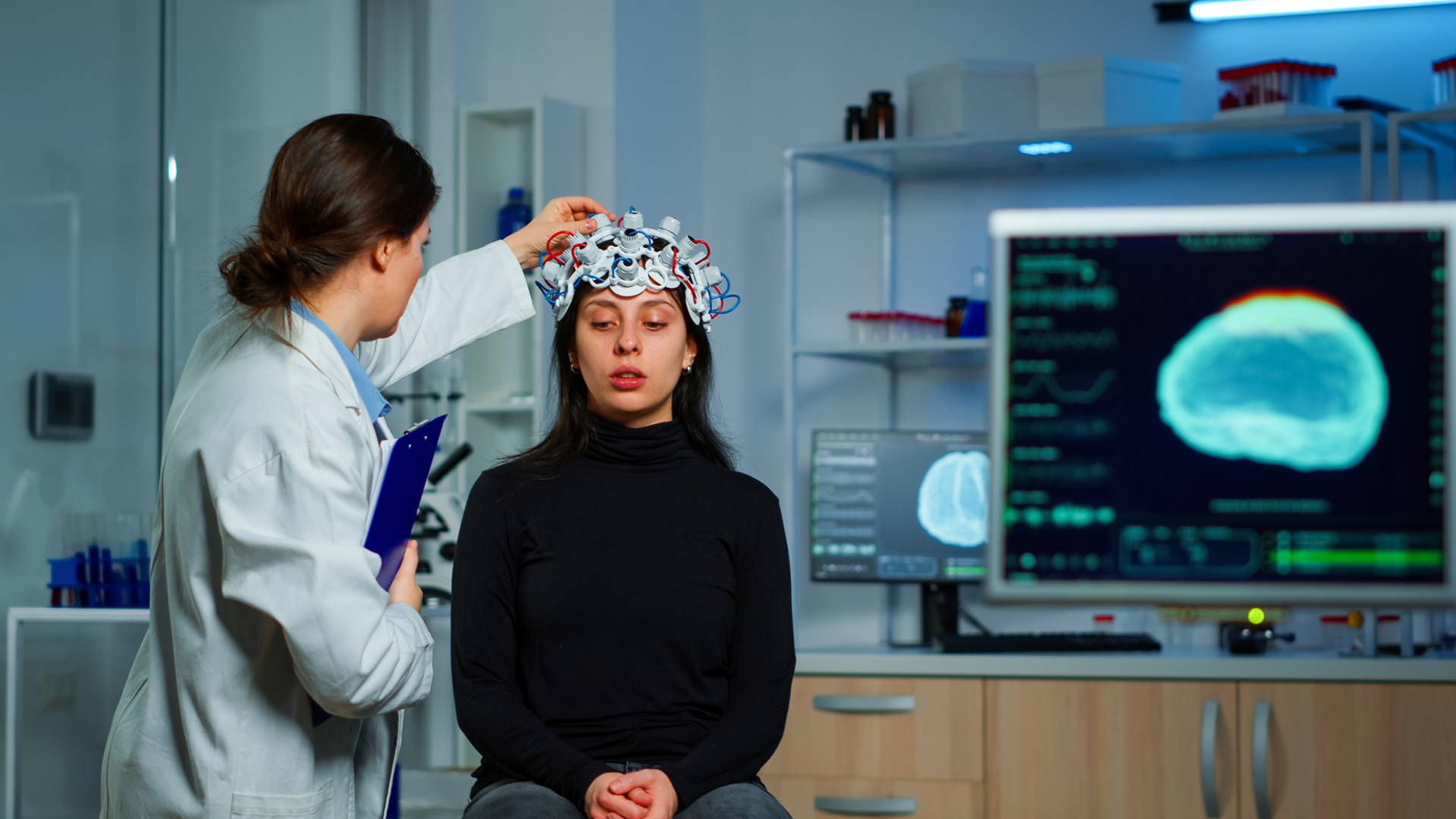
1. Patient Preparation
In order to lower the risk of thromboembolism, patients are given antiplatelet treatment prior to the surgery, typically aspirin and clopidogrel. Clinical considerations determine whether to deliver conscious sedation or general anesthesia.