1. Access to Vascular
A vascular sheath is inserted after a little incision is made in the groin (usually the femoral artery) or occasionally the wrist. This allows a catheter to be inserted into the artery system.

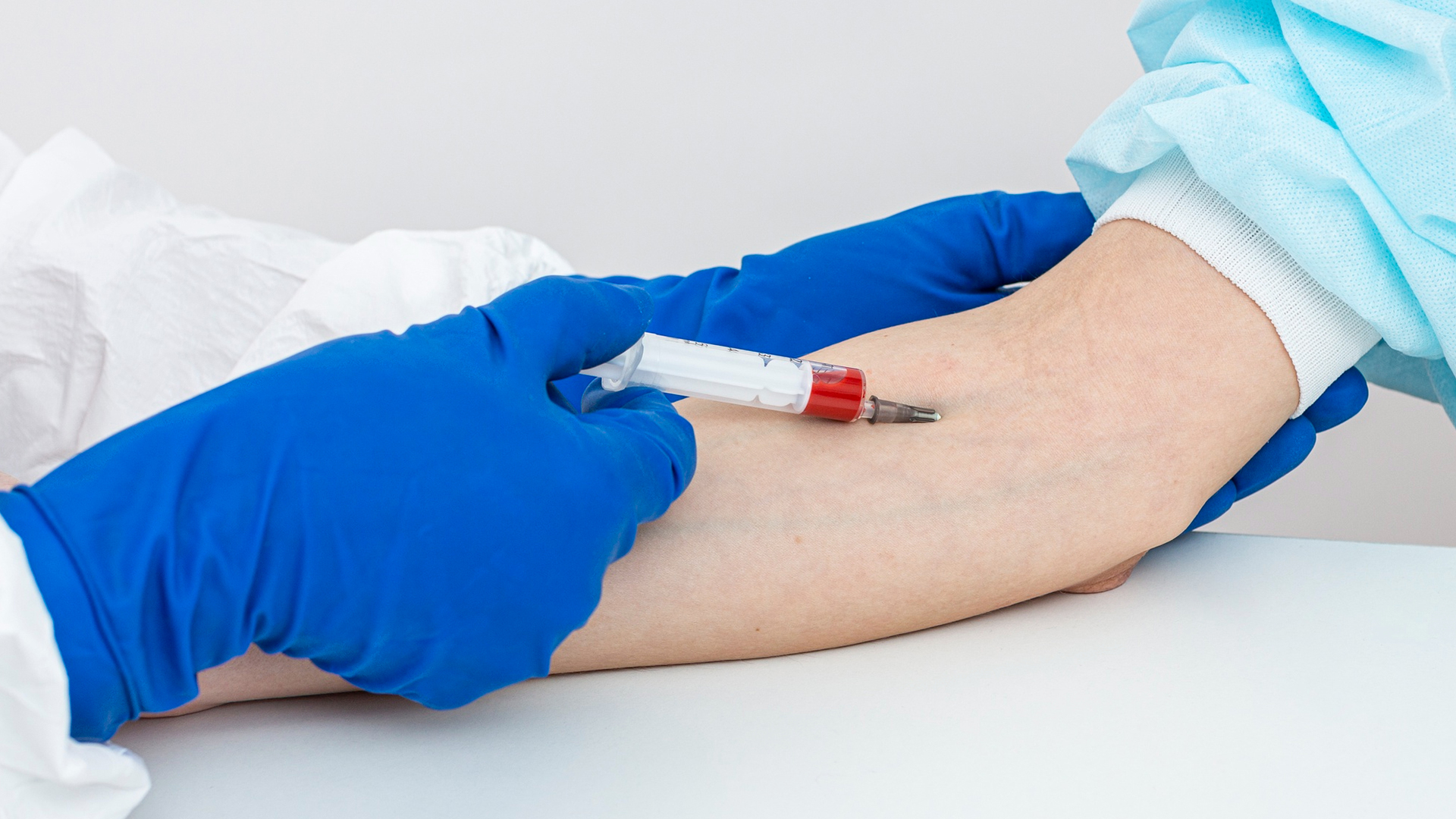
A vascular sheath is inserted after a little incision is made in the groin (usually the femoral artery) or occasionally the wrist. This allows a catheter to be inserted into the artery system.
A microcatheter is carefully inserted by guidewire into the cerebral arteries using fluoroscopic (X-ray) imaging, all the way to the precise location of the thrombus (clot) inside the brain channel. To prevent vascular damage, precise navigation is essential.
Gentle angiography is used to identify the position and extent of the blockage once the microcatheter tip has been verified at the clot site.
Via the microcatheter, thrombolytic drugs (such urokinase or alteplase) are gradually injected into the thrombus or very close to it. Clot burden, location, and patient-specific parameters affect the infusion rate and total dose. Dissolving the clot and restoring flow are the objectives.
To evaluate clot breakdown and artery reopening, periodic angiograms and/or continuous fluoroscopic monitoring are performed. The catheter may be repositioned to optimize lysis if needed. Depending on the size and reaction of the clot, the process could take minutes to hours.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Acute ischemic stroke patients experience neurological symptoms as a result of a clot obstructing blood flow to brain tissue.
It should ideally be completed within 4.5 hours of the onset of symptoms, but depending on sophisticated brain imaging, it may take up to 9 hours or longer in certain situations.
It is possible to treat clots in both minor arteries and major vessels (such the MCA and ICA).
used as a first-line therapy to break up clots and restore blood flow, particularly in cases when mechanical thrombectomy is not recommended, is not available, or is used as an adjuvant.

In order to minimize brain tissue damage, IV thrombolysis stimulates the body’s fibrinolytic system to swiftly dissolve the clot and restore blood flow to the afflicted brain region.

Compared to patients who do not receive treatment, those who receive IV thrombolysis during the treatment window are substantially more likely to experience little to no disability three months after their stroke.

Treatment for wake-up strokes or up to nine hours after onset is now possible thanks to advancements in imaging, which increases the number of patients who can benefit.

IV thrombolysis improves recanalization rates and results in major artery occlusions by acting as a bridge or adjunct to thrombectomy.

IV therapy is minimally intrusive and can be administered to individuals with mild to severe stroke and a variety of vascular occlusions.

According to meta-analyses, patients receiving thrombolysis have significantly lower death or dependence rates at three to six months.

Stressing the crucial “time is brain” principle, it can be quickly provided in emergency or pre-hospital settings (such as mobile stroke units).