1. Patient Preparation
The access site, typically the right internal jugular or common femoral vein—is prepared and covered sterilely while the patient is in a supine position. When necessary, conscious sedation and local anesthetic are given.

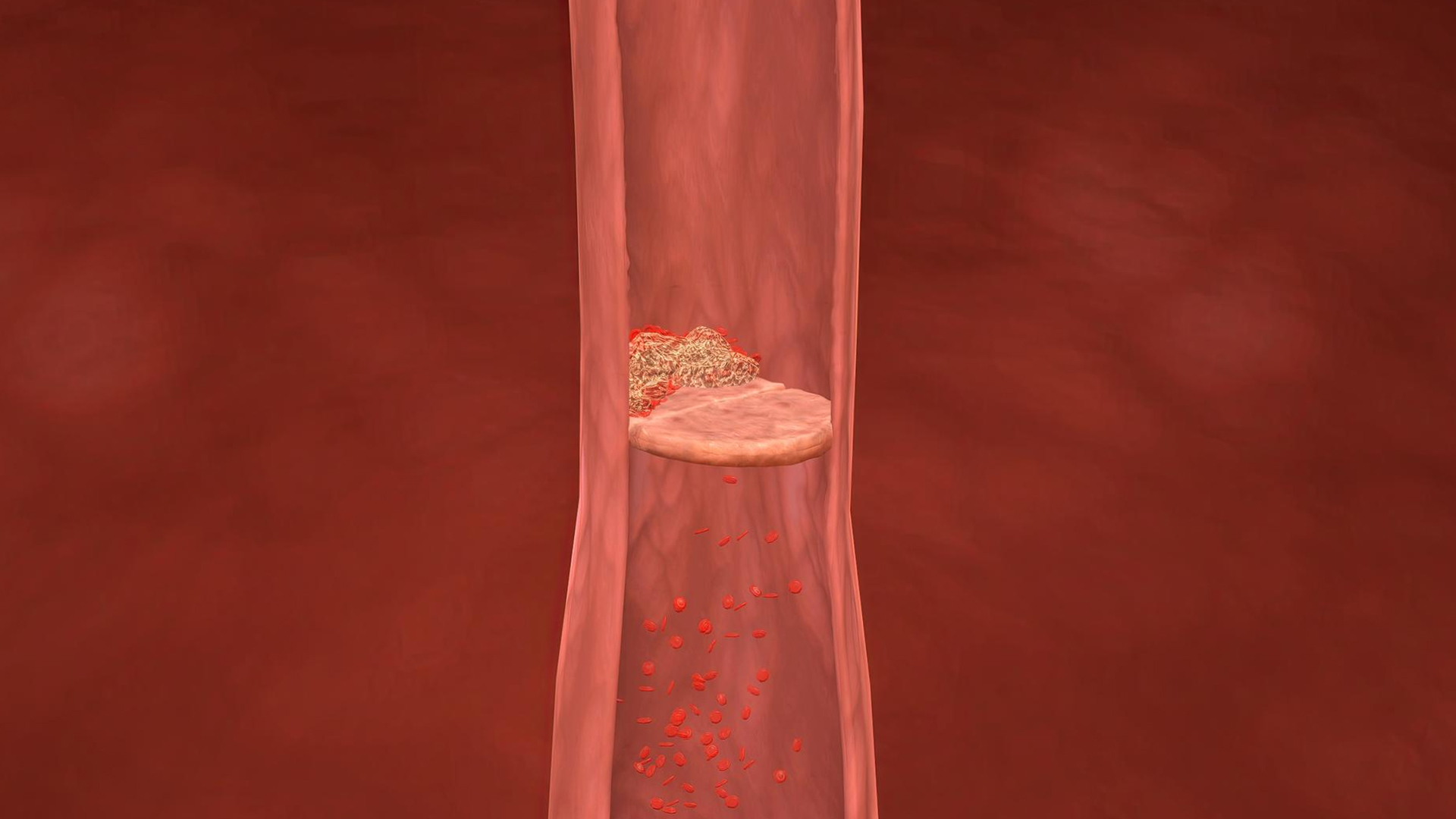
The access site, typically the right internal jugular or common femoral vein—is prepared and covered sterilely while the patient is in a supine position. When necessary, conscious sedation and local anesthetic are given.
A guidewire is advanced through the needle into the venous system up to the inferior vena cava under fluoroscopic guidance after a needle is put into the chosen vein (femoral or jugular) using ultrasound guidance.
In order to see the anatomy of the vena cava, verify patency, rule out thrombus, and locate the renal vein to direct filter implantation, a catheter is inserted into the IVC and contrast dye is administered.
To create a conduit for the filter delivery system, a vascular sheath is positioned over the guidewire. The manufacturer's instructions are followed when loading and preparing the IVC filter on its delivery device.
Usually infrarenal (below renal veins), the filter delivery system is progressed via the sheath into the IVC to the proper level. Fluoroscopy is used to confirm proper placement.
The filter expands and attaches itself to the vena cava wall after being freed from the delivery system. Deployment is closely monitored to prevent tilting or migration.
To verify filter location, IVC and renal vein extension, and patency, post-deployment venography is carried out.
The guidewire and delivery sheath are taken off. Manual compression or closure devices are used to achieve hemostasis at the venous puncture site.
The patient is usually released on anticoagulant treatment or in accordance with therapeutic indication after being observed for problems including bleeding or thrombosis at the access site.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Patients with deep vein thrombosis (DVT) or pulmonary embolism (PE) who are not eligible for anticoagulant medication because of bleeding risk or other medical conditions frequently have IVC filters implanted.
In order to stop emboli from entering the lungs, patients who experience recurrent PE or DVT despite receiving sufficient anticoagulation may benefit from filter implantation.
IVC filters may be administered as a preventive measure to patients who are immobilized as a result of trauma, major surgery, or who are at high risk of developing VTE and cannot be anticoagulated.
As a temporary approach to stop further emboli in critically ill patients while definitive treatment is being administered.
those having spinal surgery, bariatric surgery, or other procedures that are contraindicated for anticoagulation and have an increased risk of VTE.
Filters lower the risk of PE by preventing big emboli from moving from the legs or pelvis to the lungs.
Permanent filters may be used for long-term anticoagulation contraindications, while retrievable filters are frequently employed when anticoagulation is anticipated to be temporarily stopped.

IVC filters greatly lower the risk of potentially deadly PE in patients who are unable to take anticoagulation or who have not responded to pharmacological therapy by successfully capturing big venous clots and preventing them from reaching the lungs.

Critical in patients with acute DVT/PE who cannot be anticoagulated because of bleeding hazards or recent surgery, trauma victims, or immobilized patients.

While permanent filters offer long-term care for certain patients, retrievable filters enable temporary protection at times when anticoagulation is contraindicated.

Filters may be helpful in preventing additional embolic events in patients who have recurrent thromboembolism despite anticoagulation.

When incorporated into comprehensive venous thromboembolism management, the use of IVC filters in carefully chosen patients is linked to improved overall clinical outcomes and a reduction in mortality from acute PE in hospital settings.