1. Anesthesia and Preparation
Local anesthesia or sedative is used to prepare the patient. Vital indicators are tracked by attached monitoring devices.

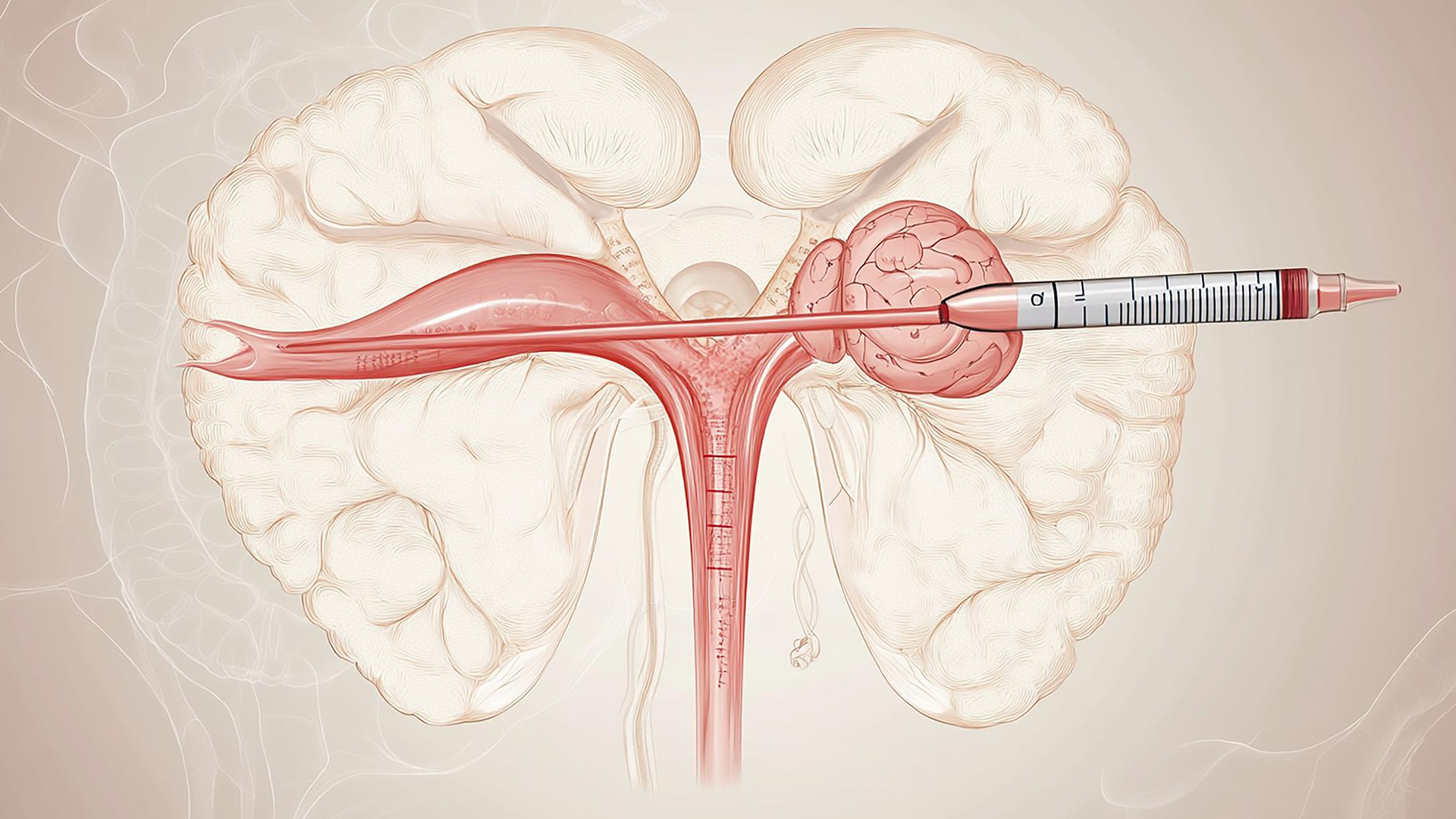
Local anesthesia or sedative is used to prepare the patient. Vital indicators are tracked by attached monitoring devices.
To reach a big vein like the femoral or internal jugular vein, a little skin incision is usually performed close to the neck or groin.
A tiny catheter is inserted via the venous system to the ovarian veins under fluoroscopic (X-ray) guidance, where it is evaluated for reflux or dilatation.
To see vein anatomy and verify reflux or varicosities in the ovarian or pelvic veins, contrast dye is injected.
To block the incompetent ovarian vein and any related pelvic veins that are causing symptoms, embolic materials including coils, plugs, liquid sclerosing agents, or glue are inserted through the catheter.
Further venograms (imaging) verify that reflux has stopped and that vein blockage has been successful. Techniques for balloon occlusion can be utilized to enhance targeting and stop embolic agent movement.
To stop bleeding, the catheter is removed and pressure is administered at the access site. The tiny cut on the skin is covered.
Patients are typically released the same day after being monitored for problems for a few hours.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.

Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Pain due to pelvic venous insufficiency, as evidenced by reflux or dilatation of the ovarian and pelvic veins, are said to have Pelvic Congestion Syndrome (PCS).
Women who have pelvic varicosities, vulvar varices, or leg varicosities of pelvic origin due to ovarian vein reflux, as determined by diagnostic imaging techniques like venography or Doppler ultrasonography.
Individuals with Lower Limb Varicosities Associated with Pelvic Venous Disease Symptoms
As part of comprehensive venous treatment, certain individuals with lower limb varicose veins that are partially caused by pelvic venous insufficiency are chosen for ovarian vein embolization.
Candidates are those with proven venous insufficiency who have not responded to pharmacologic treatments, such as hormone therapy or analgesics.
Venous diameter more than 6 mm, reflux lasting longer than 20 seconds, pelvic venous congestion, or filling of pelvic varices with reflux are the criteria used to make the diagnosis.
The majority of individuals who meet the aforementioned criteria are candidates; however, active pelvic infections and contrast material allergies are contraindications.

OVE results in less discomfort, fewer complications, and shorter hospital stays because it is carried out through a tiny skin puncture without requiring extensive surgery.

With reported success rates of over 80–85% worldwide, OVE effectively cures pelvic congestion syndrome (PCS), alleviating varicosities, pelvic heaviness, and chronic pelvic discomfort.

OVE is a practical substitute for surgical treatments because patients frequently return home the same day and swiftly resume their regular activities.

OVE has a reduced risk of blood loss, infection, and other surgical problems because it does not require open surgery.

Patient well-being and physical function are enhanced when varicose veins and chronic pelvic pain are relieved.

focuses on symptoms caused by dysfunctional ovarian and pelvic veins, which are challenging to treat medically.

OVE typically requires fewer hospital resources and is more economical than surgery. If needed, it can be done again.

There are no obvious scars or long-term cosmetic issues because the surgery simply leaves a tiny puncture hole.