1. Pre-Procedure Assessment
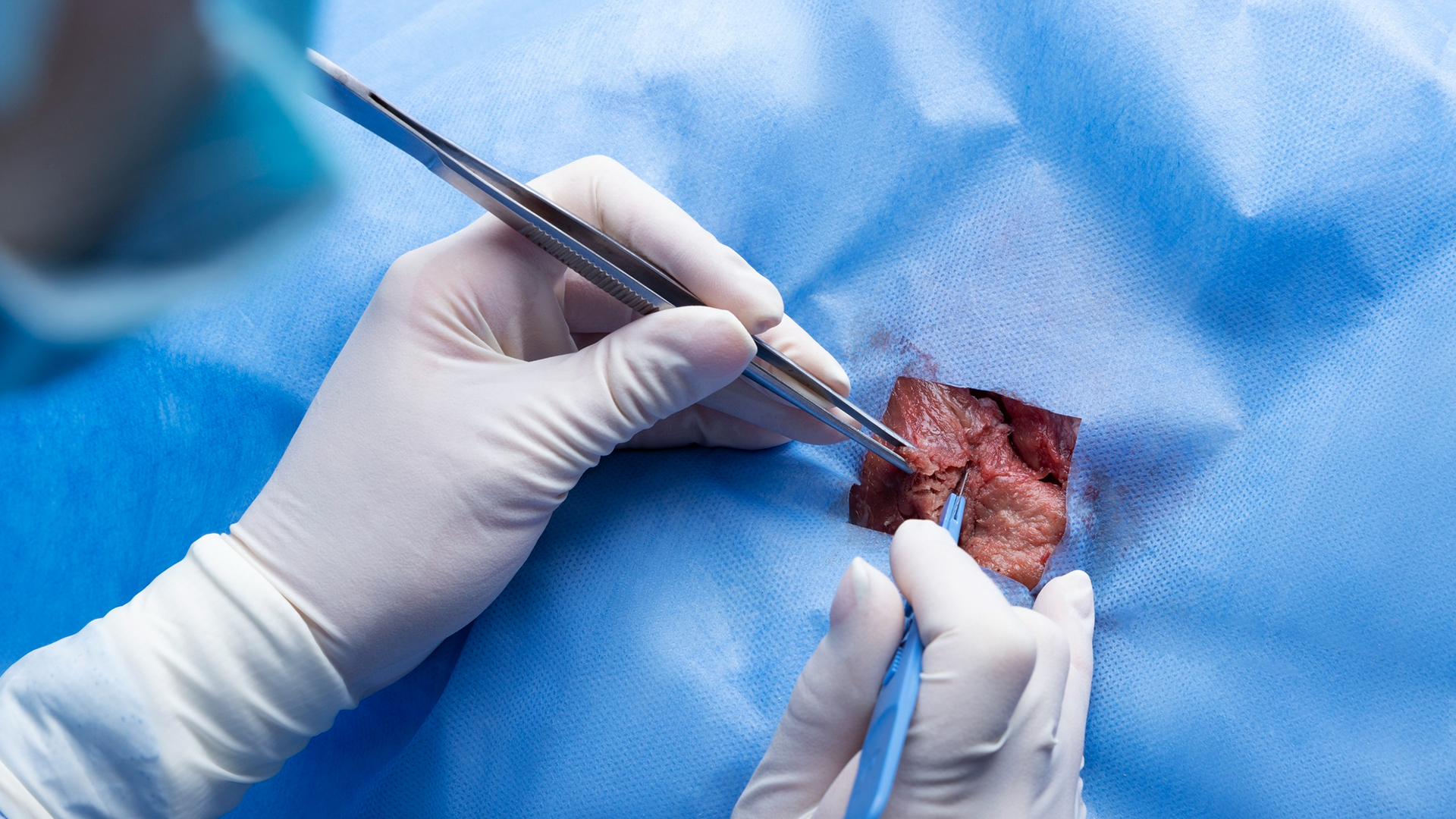
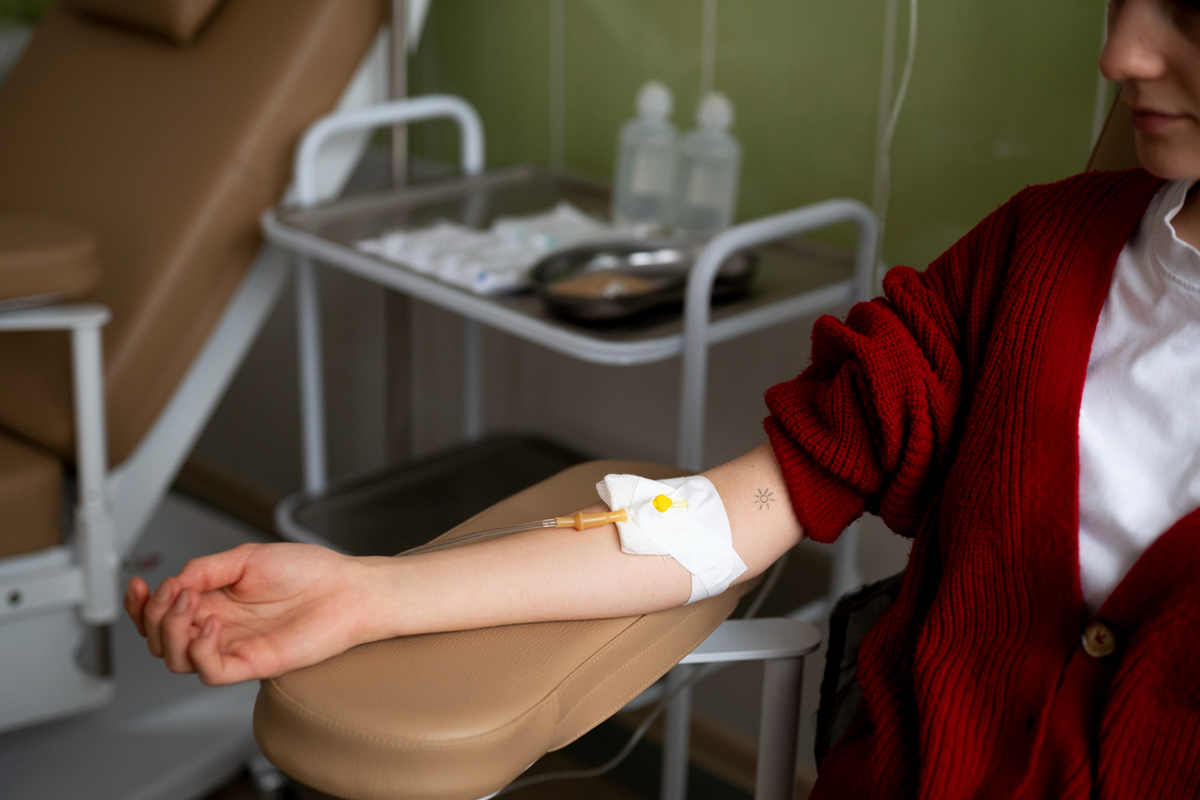
In order to examine the characteristics of the tumor and the blood flow to the liver, this stage entails comprehensive imaging such as CT or MRI. To find the arteries supplying the tumor and any aberrant blood vessel connections that could allow radioactive particles to enter non-target organs, an angiographic mapping is performed.