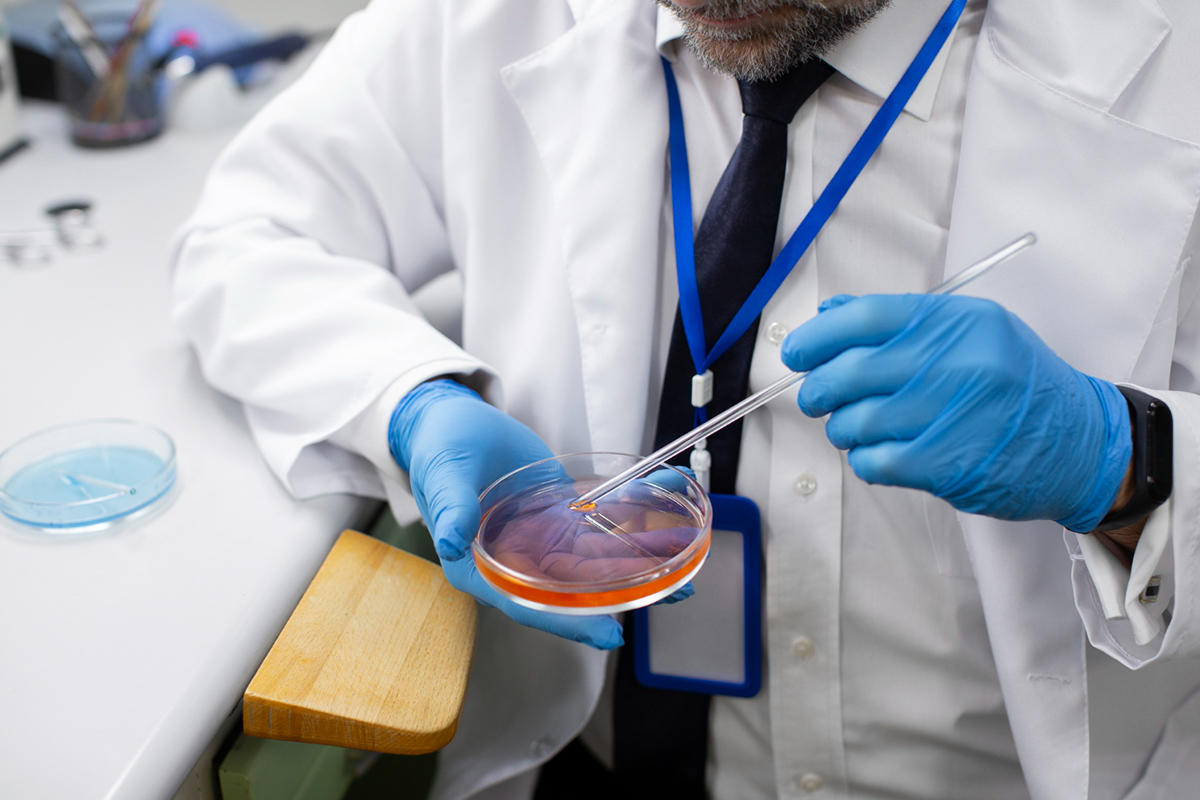
1. Preparing for the Procedure
Verify the location and features of the cyst using ultrasound. Ask the patient for informed consent after discussing the risks, advantages, and options.

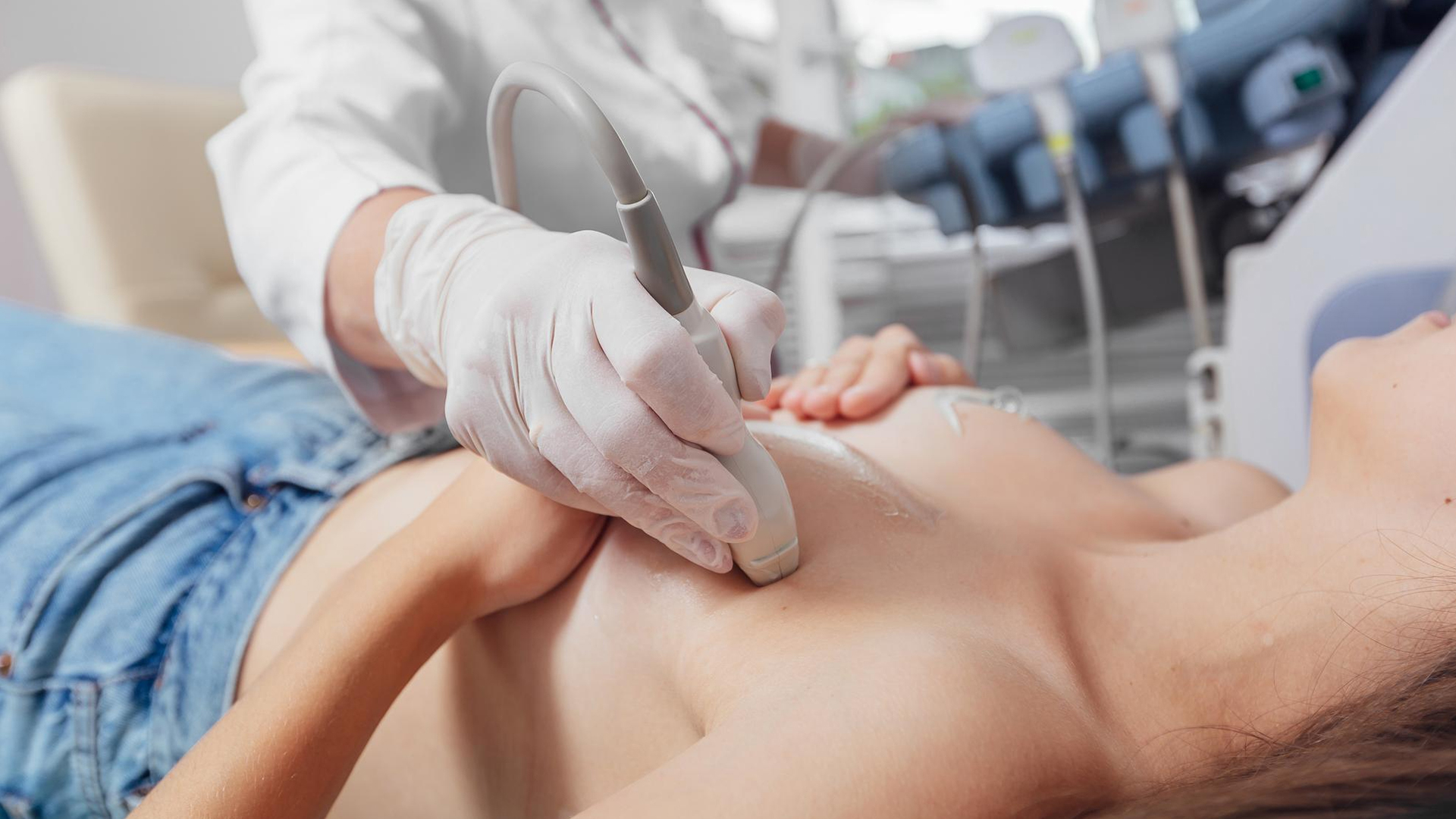
Verify the location and features of the cyst using ultrasound. Ask the patient for informed consent after discussing the risks, advantages, and options.
In order to reveal the target breast area, the patient lies comfortably, usually supine or slightly twisted.
Apply sterile drapes after cleaning the skin surrounding the cyst with an antiseptic solution.
Although a tiny amount of lidocaine may be injected around the aspiration site if necessary, local anesthetic is typically not needed.
Locate the cyst exactly in real time by placing the ultrasound transducer on the breast.
Make sure the needle tip is precisely positioned inside the cyst by inserting a tiny needle (often 21–22 gauge) into the skin under ultrasound guidance.
Using a syringe attached to the needle, carefully aspirate cyst fluid while keeping an eye on the ultrasonography to verify cyst collapse.
The fluid may be submitted for cytological or microbiological study if it seems worrisome (for example, bloody or hazy).
To stop the bleeding and avoid a hematoma, remove the needle and provide direct manual pressure to the area.
Cover the entrance site with a sterile dressing. Give directions for aftercare, including recommendations for follow-up and indications of infection or recurrence.
Lorem Ipsum is simply dummy text of the printing and typesetting industry.





Any solid mass found on ultrasound that is indicative of cancer, particularly those with a BI-RADS score of 4 or 5.
Ultrasound-identified lesions that cannot be touched physically necessitate image-guided localization.
when the lump is palpable and can be precisely located with ultrasound help.
Subtle tissue abnormalities that are challenging to identify clinically can be biopsied with the aid of ultrasound guidance.
typically in addition to mammography, particularly if ultrasonography reveals microcalcifications or if the results of the mammography are worrisome.
Where stereotactic or MRI-guided biopsies may be less feasible, ultrasound provides greater access to lesions near the chest wall or nipple.
to accurately distinguish between benign and malignant tumors, offering direction for further treatment.
This rapid, minimally invasive, radiation-free technique is appropriate for outpatient settings.

minimizes tissue damage and leaves almost no scars by requiring only a tiny needle and a tiny skin puncture rather than a surgical incision.

enhances biopsy accuracy and safety by offering real-time visualization for accurate needle positioning.

uses sound waves for imaging, which makes it safe for repeated treatments and pregnant women.

With local anesthesia, the surgery usually takes less than an hour, resulting in little discomfort and a quick recovery.

produces trustworthy tissue samples for histological diagnosis, supporting prompt and precise treatment choices.

Both palpable and non-palpable breast lesions, such as those close to the axilla, nipple, or chest wall, are effectively treated.

less expensive than MRI-guided or surgical biopsies, which lessens the burden on patients and healthcare expenses.

Patients can resume their regular activities more quickly following a shorter recovery period than following a surgical biopsy.