Intracranial Hemorrhage Of Unknown Etiology
Intracranial Hemorrhage Of Unknown Etiology
WHAT IS
INTRACRANIAL HEMORRHAGE OF UNKNOWN ETIOLOGY?
This is when there is bleeding in the brain that can’t be immediately linked to a known cause, like an accident or an aneurysm. It can cause a sudden headache, neurological problems, and a high risk of quickly getting worse.
causes
Hematological disorders
Brain tumors
Infections
Systemic conditions
Drug abuse
Trauma
Idiopathic or cryptogenic
symptoms
Sudden, severe headache
Nausea and vomiting
Lethargy or confusion
Sudden weakness or numbness
Loss of consciousness or decreased alertness
Seizures
Difficulty speaking or understanding speech
Vision changes or temporary loss of vision
Difficulty with balance or coordination
Stiff neck
Sensitivity to light
Dizziness or feeling lightheaded
Paralysis or numbness in limbs or face
Coma in severe cases

if untreated?
High Mortality

Untreated hemorrhage carries a high risk of death.
Hematoma Expansion

Continued bleeding or rebleeding can increase hematoma size, worsening brain injury and mass effect.
Brain Damage

Increased intracranial pressure from the bleed can cause brain tissue compression, ischemia, swelling, and herniation, leading to permanent neurological deficits or death.
Neurological Disability

Survivors often have significant disabilities, including paralysis, speech difficulties, cognitive impairment, and seizures.
Secondary Complications

Such as hydrocephalus, infections, deep vein thrombosis, and systemic complications can worsen outcomes.
Poor Prognosis

Factors predicting poor outcomes include large hemorrhage volume, low Glasgow Coma Scale at presentation, infratentorial location, intraventricular hemorrhage, and older age.
Long-term Impact

Even survivors have increased long-term mortality and risk of recurrent strokes or hemorrhages.

diagnosis
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text. Lorem Ipsum is simply dummy text of the printing and typesetting industry
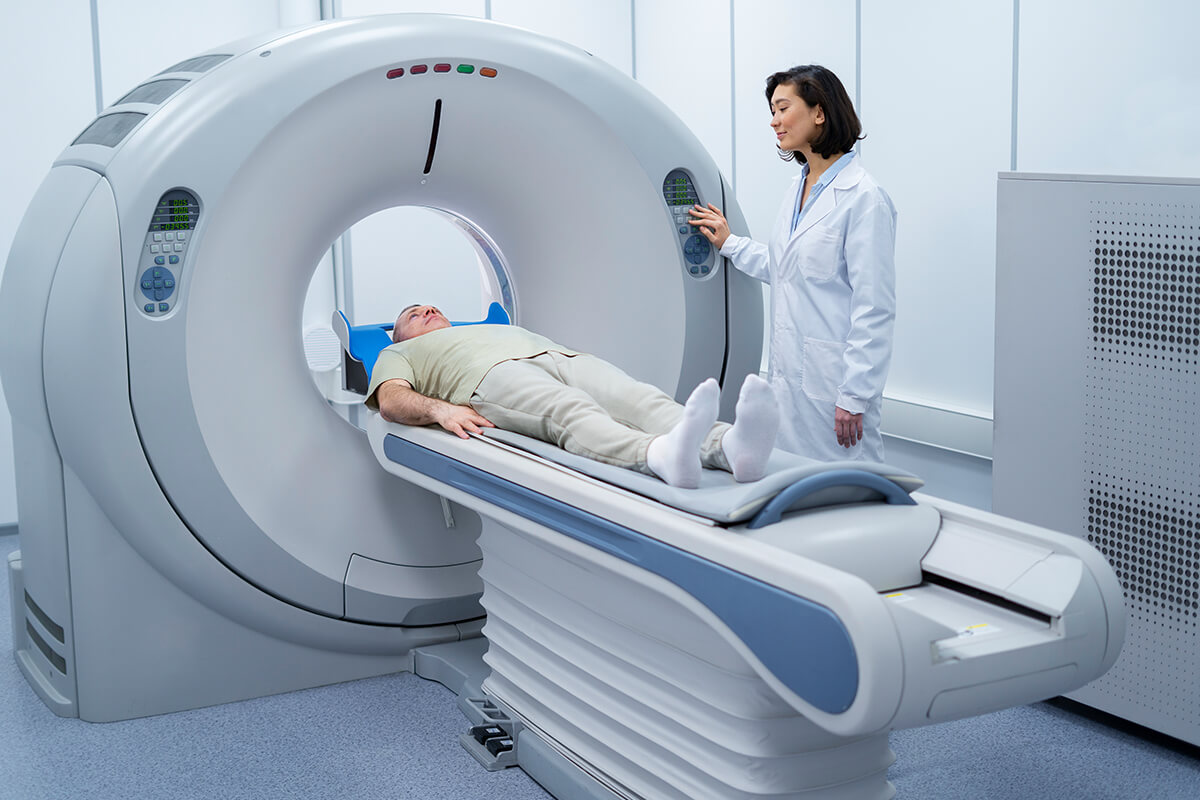
CT Angiography (CTA)
-
 Done to investigate vascular abnormalities like aneurysms, arteriovenous malformations (AVMs), or other vascular lesions that may cause hemorrhage, especially if initial CT suggests vascular pathology.
Done to investigate vascular abnormalities like aneurysms, arteriovenous malformations (AVMs), or other vascular lesions that may cause hemorrhage, especially if initial CT suggests vascular pathology.
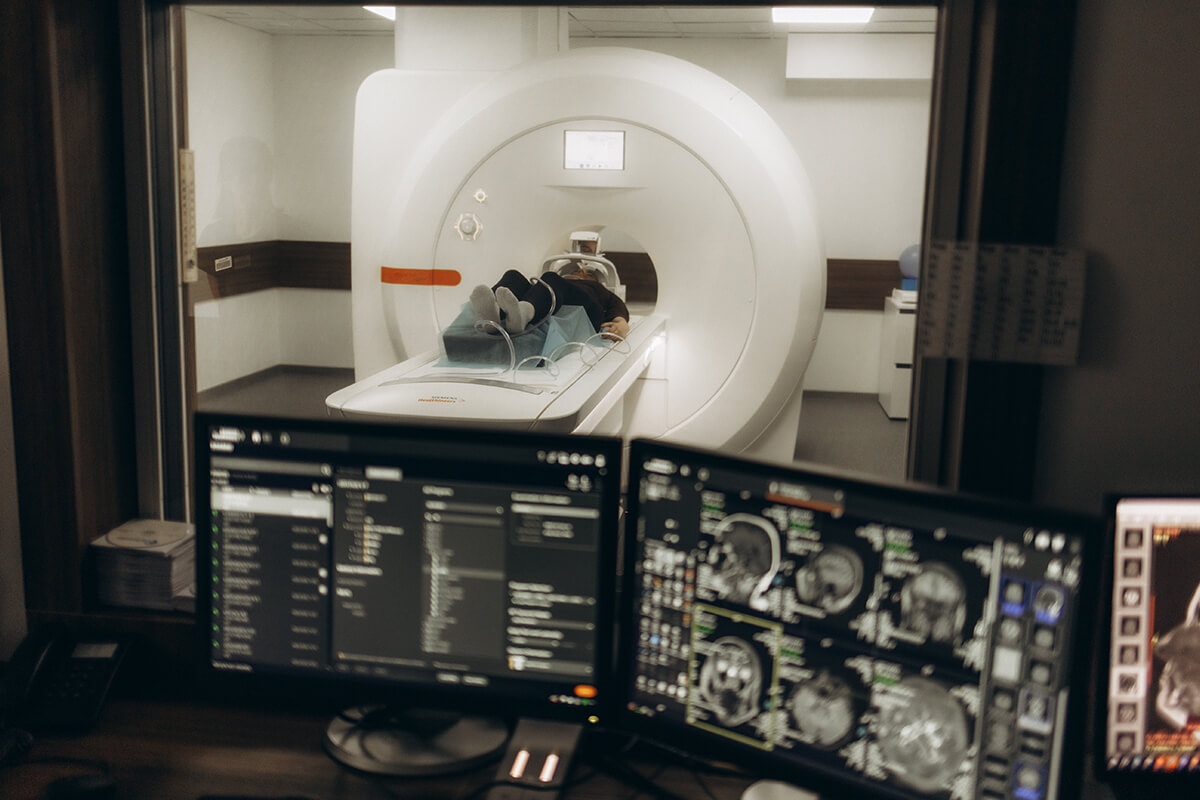
Magnetic Resonance Imaging (MRI) and Magnetic Resonance Angiography (MRA)
-
 MRI helps detect older hemorrhages, small lesions, or subtle vascular malformations missed on CT. MRA further evaluates blood vessels noninvasively.
MRI helps detect older hemorrhages, small lesions, or subtle vascular malformations missed on CT. MRA further evaluates blood vessels noninvasively.
Digital Subtraction Angiography (DSA)
-
 The gold standard for identifying vascular causes of hemorrhage, particularly AVMs, aneurysms, DAVFs, or vasculitis. It provides dynamic, detailed vessel visualization and is often performed if CTA/MRA is inconclusive.
The gold standard for identifying vascular causes of hemorrhage, particularly AVMs, aneurysms, DAVFs, or vasculitis. It provides dynamic, detailed vessel visualization and is often performed if CTA/MRA is inconclusive.

Laboratory tests
-
 Blood coagulation studies, toxicology screen, and other relevant labs are done to identify coagulopathies or systemic causes.
Blood coagulation studies, toxicology screen, and other relevant labs are done to identify coagulopathies or systemic causes.

Lumbar puncture
-
 Sometimes performed if subarachnoid hemorrhage is suspected but CT is negative.
Sometimes performed if subarachnoid hemorrhage is suspected but CT is negative.




