Ovarian Vein Insufficiency
Ovarian Vein Insufficiency
WHAT IS
Ovarian Vein Insufficiency?
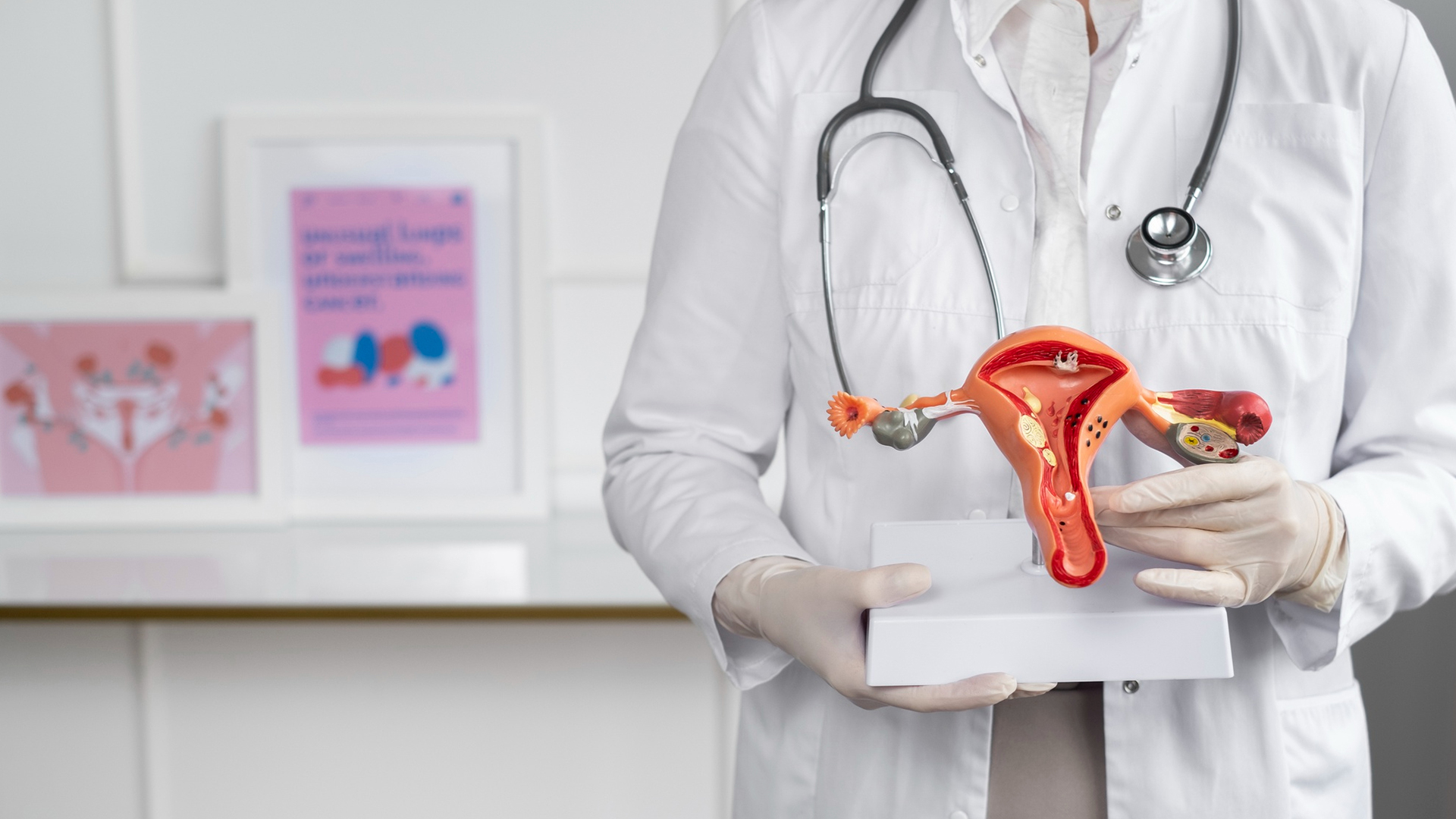
This condition results in pelvic pain and swelling due to weak or leaky ovarian veins. In order to relieve discomfort and restore normal venous flow, malfunctioning veins are closed off by vein embolization.
causes
Multiple pregnancies and hormonal influences
Congenital valve absence or dysfunction
Family history and anatomical factors
Surgery on the abdomen or pelvis
Outflow obstruction
Additional factors
symptoms
Chronic dull, aching, or "dragging" pain in the lower back
pressure, heaviness, and occasionally a feeling of fullness
Dyspareunia, or pain during or after sexual activity
varicose veins in their legs
urinary retention
Unusual pelvic or vaginal symptoms
Examining the abdomen or pelvis reveals tenderness
Emotional effects such as depression or anxiety

if untreated?
Chronic pelvic pain

The most frequent outcome is persistent, frequently getting worse pelvic pain, which can linger for months or even years and have a major negative influence on day-to-day functioning and mental health.
Progressive varicose veins

If left untreated, pelvic venous reflux causes varicose veins in the pelvis, vulva, inner thighs, buttocks, and occasionally lower limbs to grow and enlarge. These veins can become more uncomfortable and unsightly over time.
Superficial thrombophlebitis

Redness, tenderness, and swelling may result from dilated veins becoming inflamed or forming blood clots.
Hemorrhage

Rarely, enlarged veins may burst, causing pelvic or vaginal bleeding.
Skin alterations

Prolonged venous congestion can cause eczema, swelling, skin discoloration, and, in extreme situations, ulcers close to the afflicted areas.
Effect on sexual and urinary function

Prolonged pain and congestion can impair bladder function, result in frequent urination, and cause discomfort during sexual activity.
Psychological distress

Because of the delayed diagnosis, persistent symptoms are frequently linked to anxiety, depression, and distress.
Recurrence risk

Untreated vein insufficiency can result in more severe or recurrent pelvic symptoms, which may eventually necessitate more invasive procedures. The condition may also worsen over time, particularly in women who have had multiple pregnancies.

diagnosis
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text. Lorem Ipsum is simply dummy text of the printing and typesetting industry
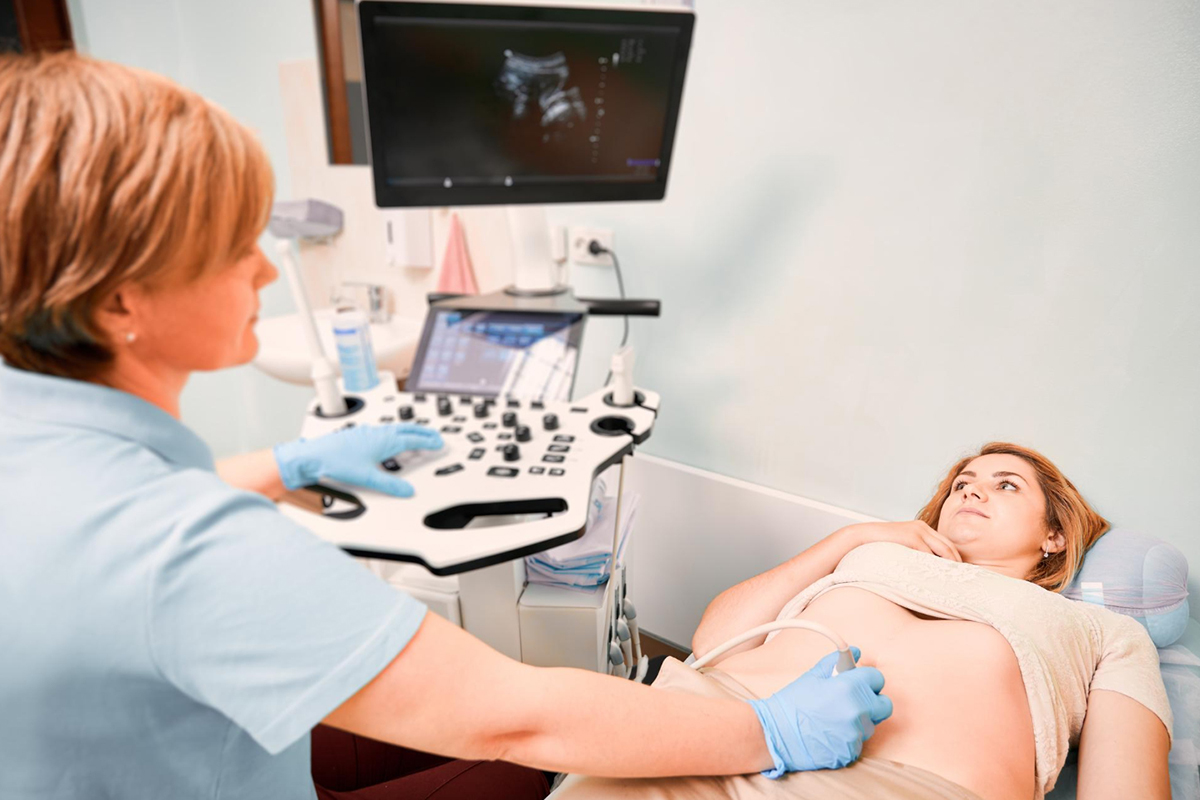
Ultrasound
-
 Dilated, tortuous pelvic veins, usually larger than 4 mm in diameter, are detected by ultrasound. exhibits communication with pelvic varicosities, venous reflux, and slow blood flow (≤ 3 cm/s). By revealing variations in flow or diameter, dynamic maneuvers like Valsalva can increase sensitivity. Veins and cystic adnexal masses can be distinguished using Color Doppler.
Dilated, tortuous pelvic veins, usually larger than 4 mm in diameter, are detected by ultrasound. exhibits communication with pelvic varicosities, venous reflux, and slow blood flow (≤ 3 cm/s). By revealing variations in flow or diameter, dynamic maneuvers like Valsalva can increase sensitivity. Veins and cystic adnexal masses can be distinguished using Color Doppler.
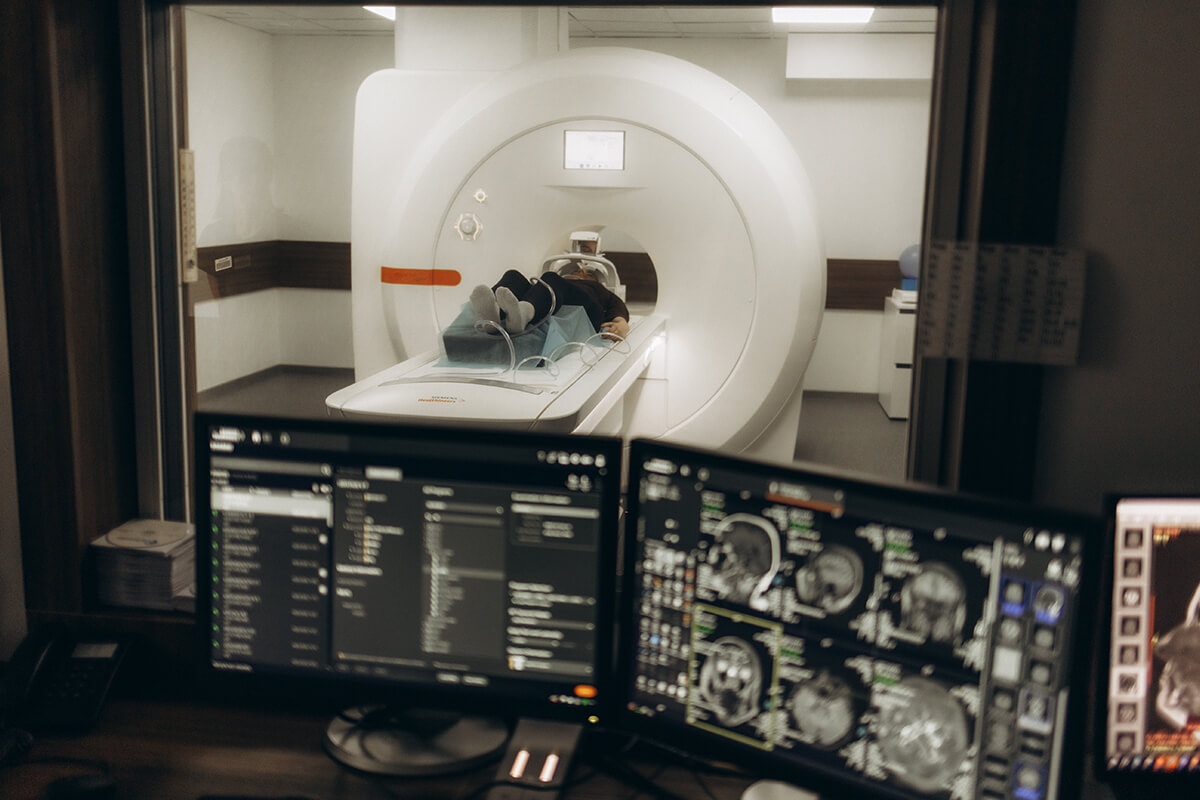
MRI and MR Venography (MRV)
-
 Serpentine flow voids (T1), heterogeneous signal intensity brought on by slow flow (T2), and delayed enhancement of tortuous, dilated vessels are all visible on MRI and MR Venography (MRV). Time-resolved MR angiography describes pelvic varicosities and distinguishes between anterograde and retrograde venous flow. Ovarian and hypogastric vein insufficiency can be detected noninvasively and with high sensitivity.
Serpentine flow voids (T1), heterogeneous signal intensity brought on by slow flow (T2), and delayed enhancement of tortuous, dilated vessels are all visible on MRI and MR Venography (MRV). Time-resolved MR angiography describes pelvic varicosities and distinguishes between anterograde and retrograde venous flow. Ovarian and hypogastric vein insufficiency can be detected noninvasively and with high sensitivity.
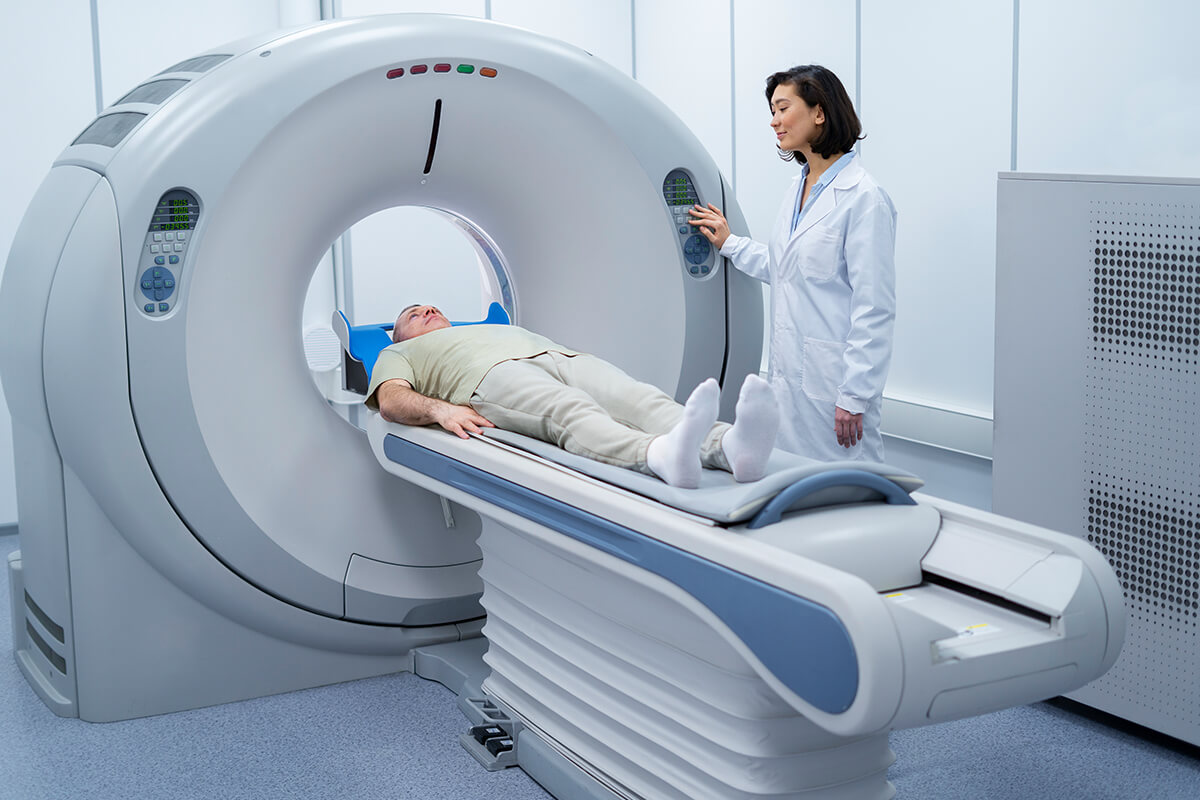
CT Venography
-
 Demonstrates dilated ovarian and pelvic veins and can detect abdominal or pelvic pathology that is present concurrently. Diagnostic criteria include parauterine veins with a diameter of ≥4 mm, dilated ovarian veins with a diameter of >8–10 mm, and congestion throughout the pelvic plexus. Though less popular with young women because of radiation exposure, it is especially helpful for anatomical mapping.
Demonstrates dilated ovarian and pelvic veins and can detect abdominal or pelvic pathology that is present concurrently. Diagnostic criteria include parauterine veins with a diameter of ≥4 mm, dilated ovarian veins with a diameter of >8–10 mm, and congestion throughout the pelvic plexus. Though less popular with young women because of radiation exposure, it is especially helpful for anatomical mapping.
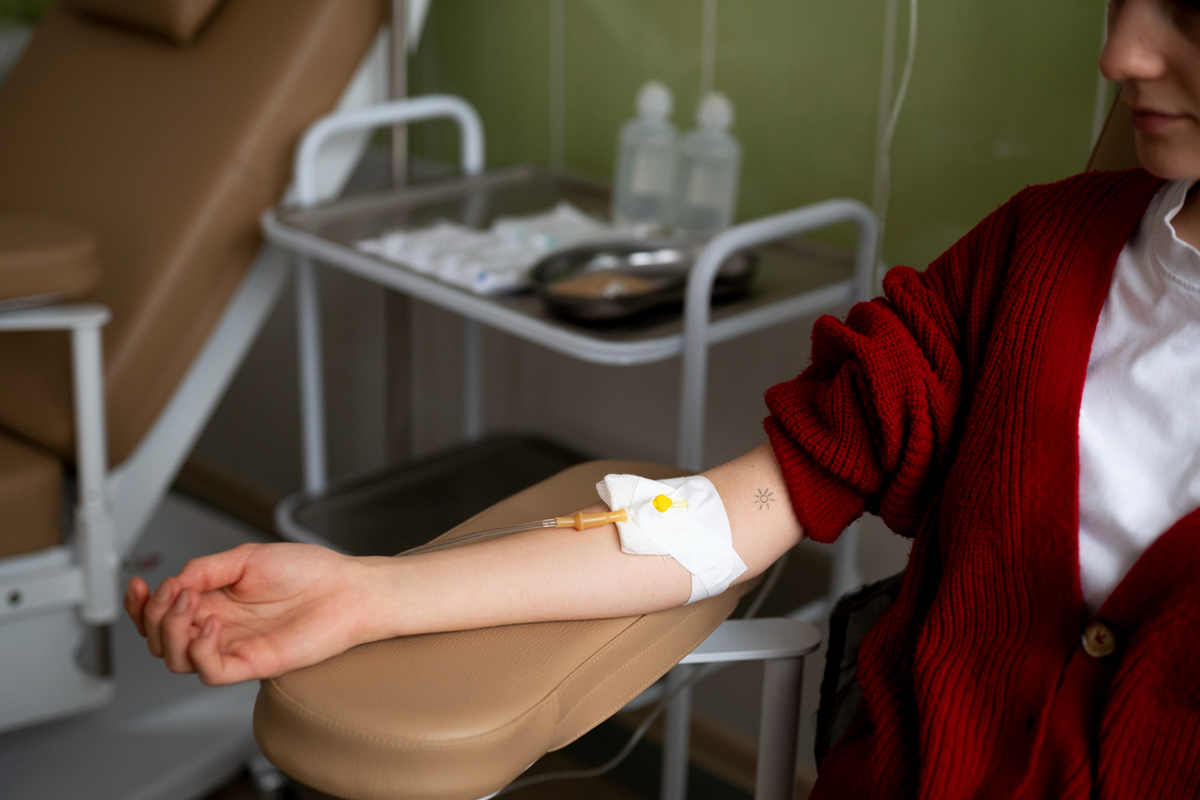
Catheter Venography
-
 The gold standard for conclusive diagnosis. Direct visualization of pelvic congestion, reflux, dilatation, and venous anatomy can be done in conjunction with therapeutic procedures such as embolization, determining the vein's diameter, the level of congestion, and the time it takes for the contrast to vanish (scoring system).
The gold standard for conclusive diagnosis. Direct visualization of pelvic congestion, reflux, dilatation, and venous anatomy can be done in conjunction with therapeutic procedures such as embolization, determining the vein's diameter, the level of congestion, and the time it takes for the contrast to vanish (scoring system).




