Uterine Fibroids
Uterine Fibroids
WHAT IS
UTERINE FIBROIDS?
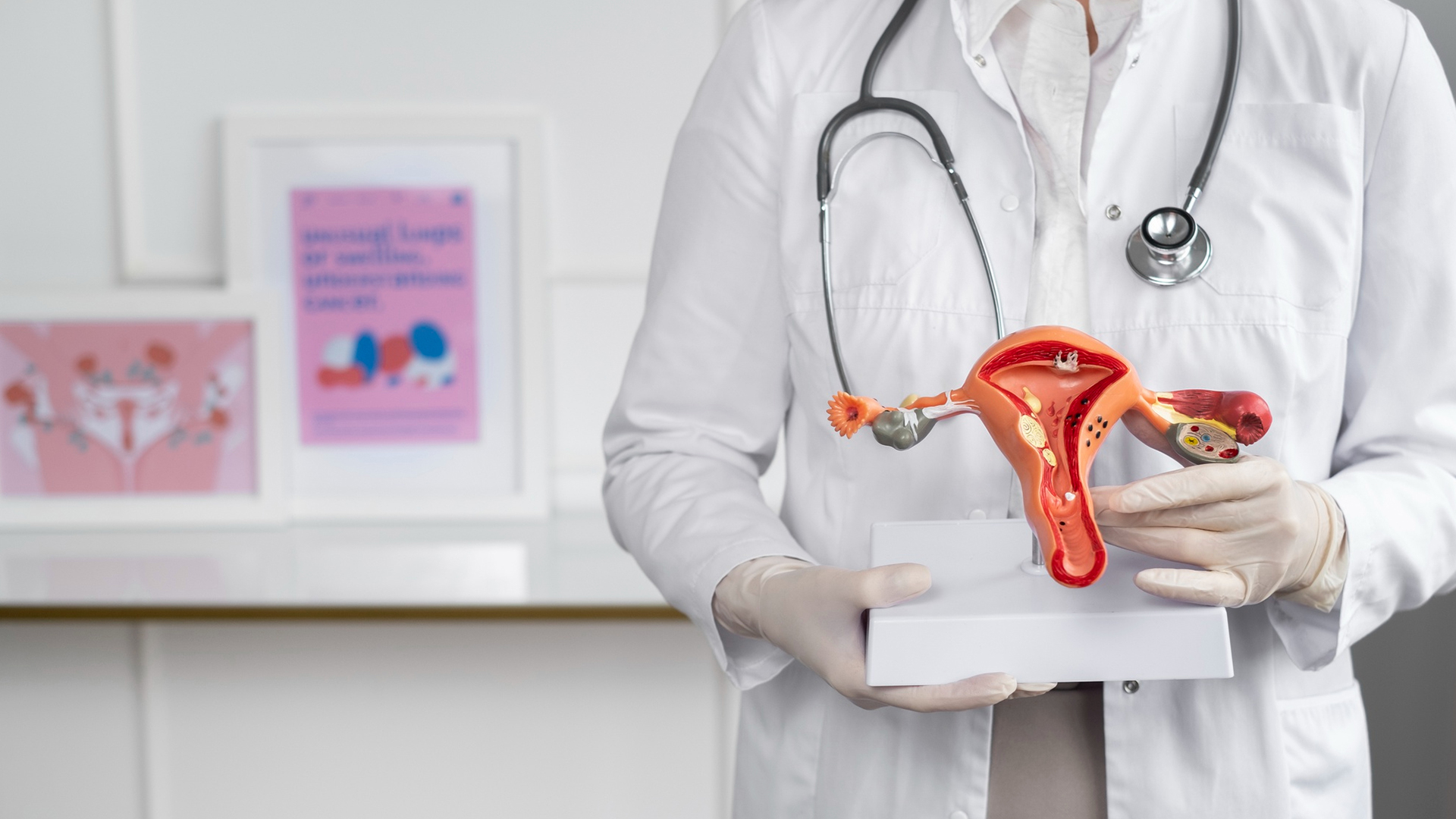
They are non-cancerous growths in the uterus that can cause pressure symptoms, pelvic pain, and heavy menstrual bleeding. By blocking the fibroids’ blood supply, interventional radiology provides uterine artery embolization (UAE), a minimally invasive procedure that reduces fibroids and alleviates their symptoms. The majority of women report considerable symptom relief with this approach, which also protects the uterus and speeds up recovery.
causes
Hormones
Genetic alterations
Growth factors
Extracellular matrix
symptoms
Heavy or prolonged menstrual bleeding
Periods that last longer than normal
Bleeding between periods
Pelvic pressure or pain
Frequent urination or difficulty emptying the bladder
Constipation or difficulty with bowel movements
Pain during sexual intercourse
Lower back pain or leg pain
Enlarged or swelling of the abdomen
Ongoing tiredness and weakness
Rarely, sudden severe pain if a fibroid outgrows

if untreated?
Progressively worsening symptoms

Symptoms that get worse over time: Abdominal distension, pelvic pain, pressure symptoms (on the bladder and bowel), and heavy menstrual bleeding can all get worse and interfere with everyday activities and emotional health.
Iron deficiency and chronic anemia

Ongoing severe bleeding can lead to chronic anemia, which can cause weakness, exhaustion, dyspnea, and heightened vulnerability to infections.
Pregnancy issues and infertility

Fibroids can impede the uterus, raise the risk of preterm labor, cause miscarriages, and result in complications like fetal growth restriction and placental abruption.
Adjacent organ compression

Large fibroids may put pressure on the rectum (resulting in constipation), the bladder (causing frequent, urgent, or retention urination), or the ureters (causing hydronephrosis or kidney damage).
Chronic pelvic pain

Ongoing pain and discomfort can make it difficult to go about daily tasks.
Degeneration and acute pain

Necrosis, degeneration, and abrupt, intense pain that may necessitate emergency care can occur when fibroids outgrow their blood supply.
Rare complications

Hematological alterations and, in rare cases, malignant transformation may increase the risk of venous thromboembolism.

diagnosis
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text. Lorem Ipsum is simply dummy text of the printing and typesetting industry
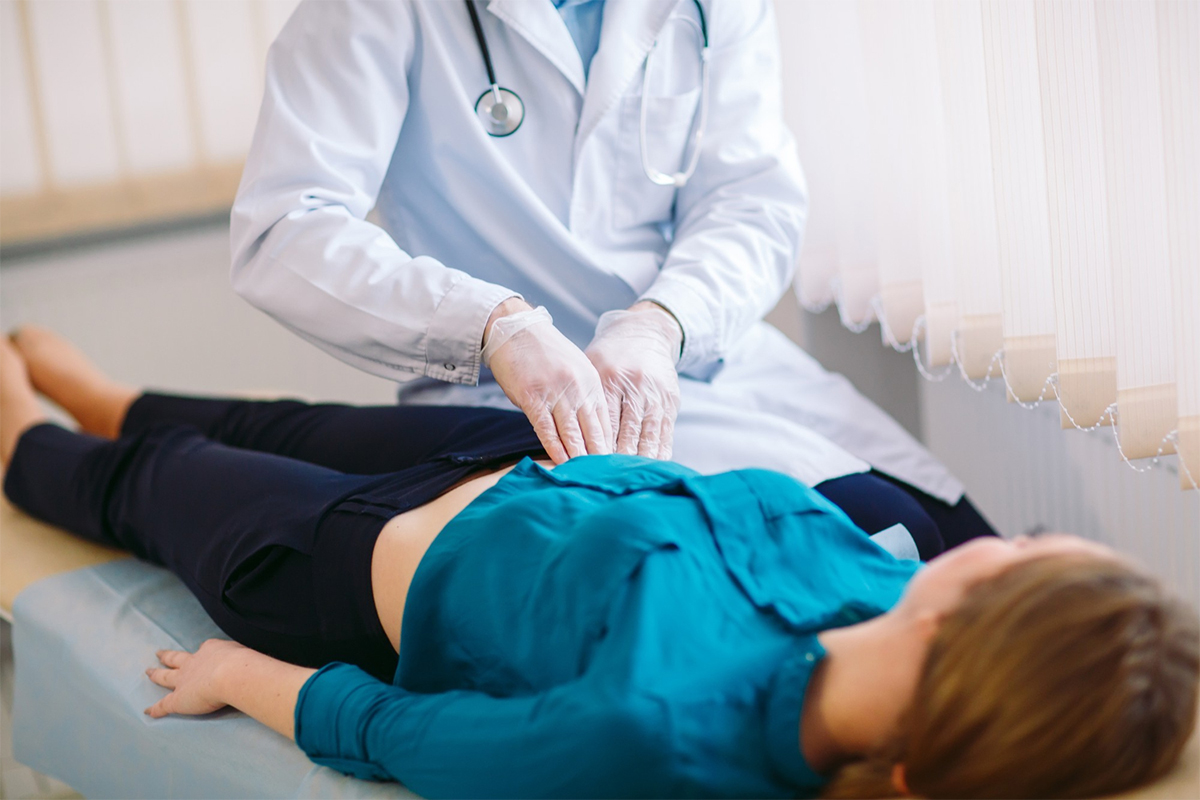
Pelvic examination
-
 During a routine pelvic exam, a medical professional may feel for an enlarged or irregularly shaped uterus, which may raise suspicions of fibroids.
During a routine pelvic exam, a medical professional may feel for an enlarged or irregularly shaped uterus, which may raise suspicions of fibroids.
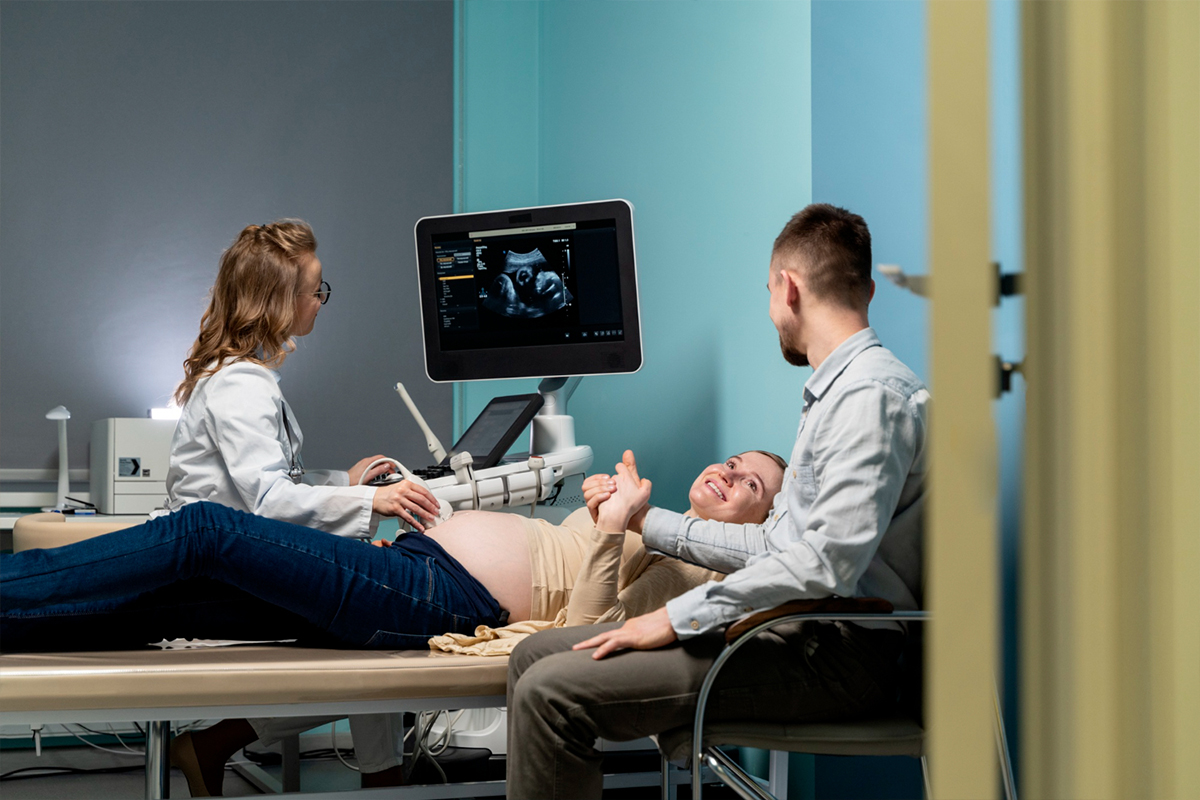
Transvaginal and transabdominal ultrasound
-
 This first-line imaging test maps and measures fibroids in the uterus by using sound waves. It is widely accessible, non-invasive, and very good at finding fibroids.
This first-line imaging test maps and measures fibroids in the uterus by using sound waves. It is widely accessible, non-invasive, and very good at finding fibroids.

Hysteroscopy
-
 To directly view the uterine cavity and submucosal fibroids, a thin instrument called a hysteroscope which combines a light and a camera, is passed through the vagina and cervix into the uterus. This process is especially helpful for assessing infertility and abnormal uterine bleeding symptoms.
To directly view the uterine cavity and submucosal fibroids, a thin instrument called a hysteroscope which combines a light and a camera, is passed through the vagina and cervix into the uterus. This process is especially helpful for assessing infertility and abnormal uterine bleeding symptoms.
MRI
-
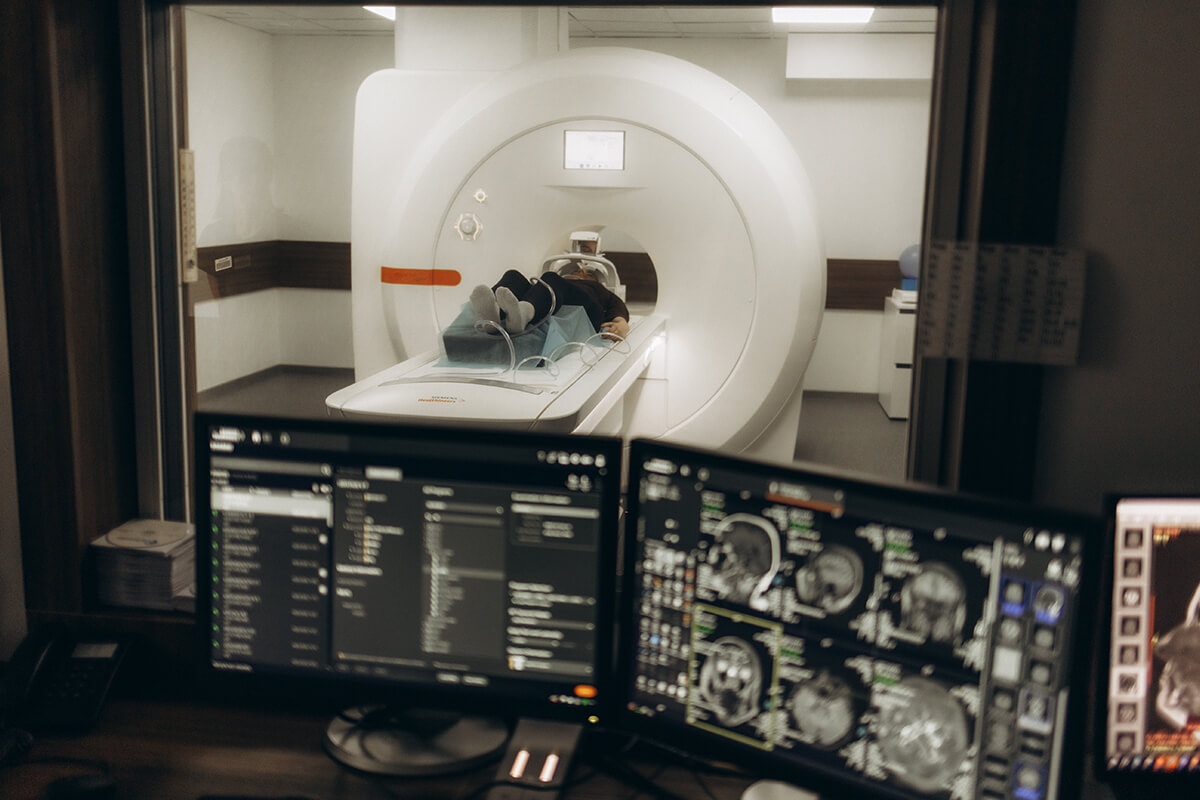
 For large or numerous fibroids, when precise mapping is necessary for treatment planning, or when ultrasound results are unclear, magnetic resonance imaging, or MRI, is utilized. Fibroids can be distinguished from other growth types using MRI.
For large or numerous fibroids, when precise mapping is necessary for treatment planning, or when ultrasound results are unclear, magnetic resonance imaging, or MRI, is utilized. Fibroids can be distinguished from other growth types using MRI.
Hysterosonography
-
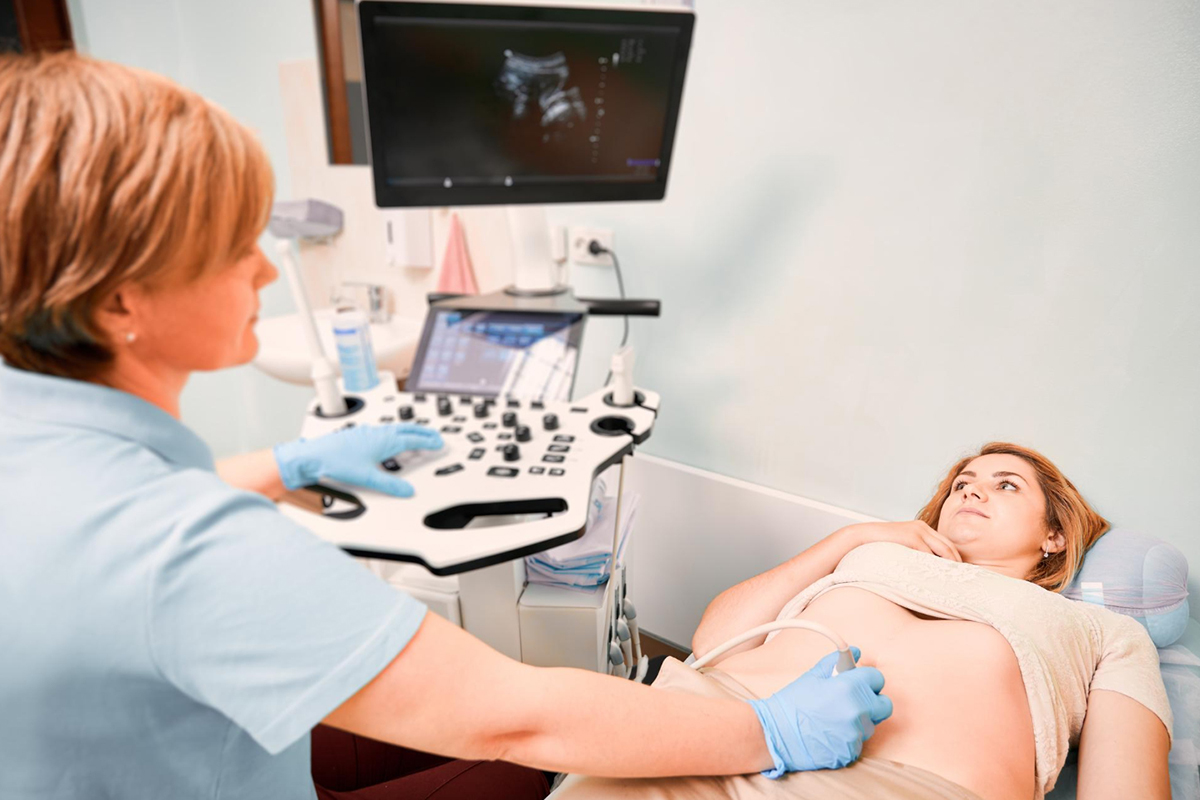
 Saline infusion sonography, also known as hysterosonography, is a type of specialized ultrasound that uses saline to improve uterine cavity visualization and identify submucosal fibroids.
Saline infusion sonography, also known as hysterosonography, is a type of specialized ultrasound that uses saline to improve uterine cavity visualization and identify submucosal fibroids.
Hysterosalpingography
-
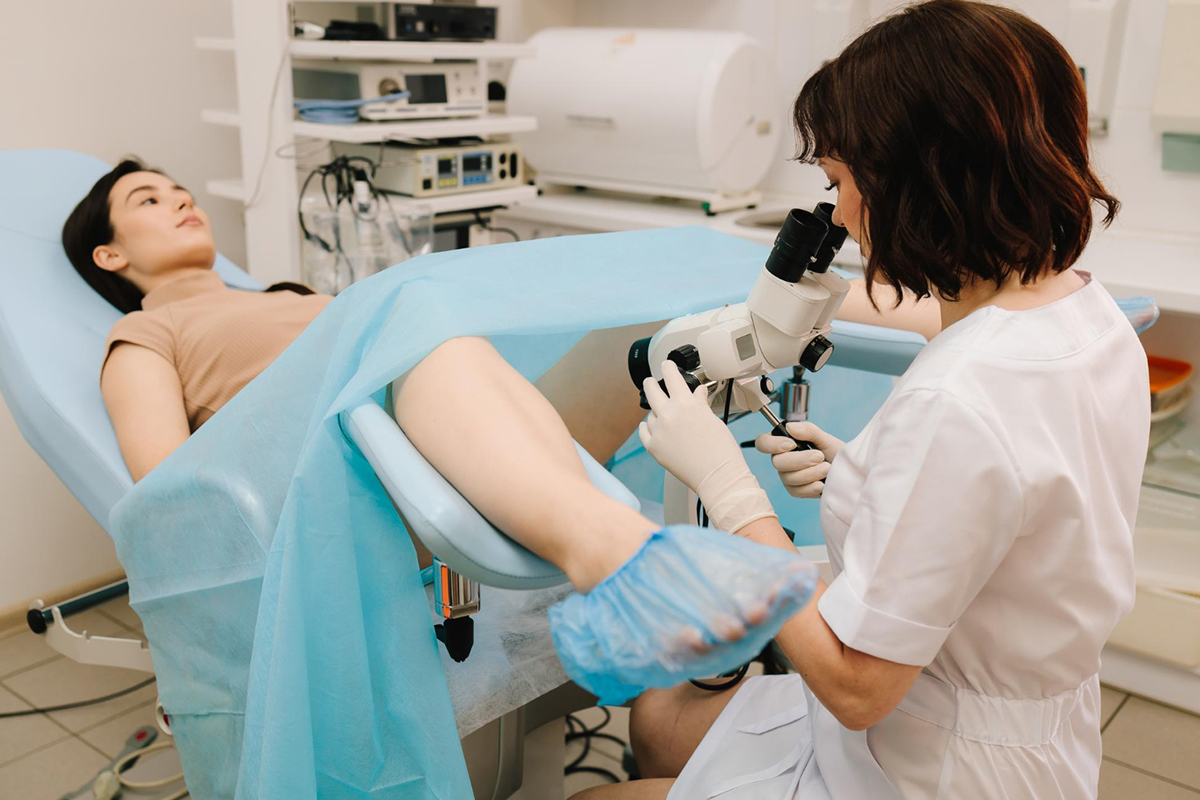
 This procedure evaluates the uterus and fallopian tubes using X-rays and a dye. It is useful for identifying fibroids that protrude into these areas and for infertility workups.
This procedure evaluates the uterus and fallopian tubes using X-rays and a dye. It is useful for identifying fibroids that protrude into these areas and for infertility workups.

Blood tests
-
 Used to check for anemia brought on by fibroids-induced heavy menstrual bleeding.
Used to check for anemia brought on by fibroids-induced heavy menstrual bleeding.




