Peripheral Vascular Disease
Peripheral Vascular Disease
WHAT IS PERIPHERAL VASCULAR DISEASE?
When blood flow in the peripheral arteries and veins, particularly in the legs, narrows or becomes blocked, it is known as peripheral vascular disease (PVD). It frequently results in symptoms such as walking-related leg pain or cramping, numbness or coldness in the legs or feet, slow-healing sores, and changes in the color or texture of the skin. Serious side effects like ulcers, infections, and in extreme situations, gangrene, which may necessitate amputation, can result from PVD. The accumulation of fatty plaques in the blood vessels, known as atherosclerosis, is the most frequent cause.

condition treated
Varicose Veins
Large, twisted veins that frequently cause pain, weight, swelling, and obvious bulging are known as varicose veins. These veins are most frequently found in the legs. They are caused by weak vein valves and, if left untreated, can result in ulcers, skin changes, and occasionally chronic venous insufficiency. Sclerotherapy, compression, and minimally invasive ablation are among the available treatments.
condition treated
Deep Vein Thrombosis (DVT)
A blood clot that forms in a deep vein, usually in the leg, causes deep vein thrombosis (DVT), which manifests as pain, swelling, redness, and warmth. If the clot spreads to the lungs, DVT can result in dangerous side effects like pulmonary embolism. Anticoagulants and occasionally catheter-based removal are the mainstays of prevention and treatment.
condition treated
Peripheral Arterial Occlusive Disease
Reduced blood flow as a result of atherosclerotic (narrowed) arteries in the limbs, particularly ib the legs, is known as peripheral arterial occlusive disease. Common symptoms include claudication, or leg pain when walking, and in more severe cases, gangrene or ulcers. Exercise, medicine, and angioplasty or stenting are all part of the treatment.
condition treated
Arteriovenous Fistulas
An irregular artery-vein junction can result in tumultuous blood flow, pain, swelling, and an increased risk of heart strain. Congenital or acquired, it occasionally necessitates surgical repair or interventional closure.
condition treated
Critical Limb Ischemia
A severe, persistent blood shortage in the leg causes tissue death (gangrene), open sores (ulcers), or chronic pain at rest. If nothing is done, amputation might be required. Wound care and revascularization are part of the treatment.
condition treated
Renal Artery Stenosis
High blood pressure and possible kidney damage are caused by the narrowing of the arteries supplying the kidneys. Imaging is used for diagnosis, and surgery, stenting, or angioplasty may be used for treatment.
condition treated
Mesenteric Ischemia
Acute, excruciating abdominal pain may result from mesenteric ischemia, which is a blockage of blood flow to the intestines. Weight loss and digestive symptoms are possible outcomes of chronic cases. Emergency revascularization or surgery is necessary in acute cases.
condition treated
May-Thurner Syndrome
This condition, which manifests as swelling, pain, and occasionally skin changes, increases the risk of DVT in the left leg when the right iliac artery compresses the left iliac vein. Stenting the compressed vein to restore flow may be part of the treatment.
how Interventional
Radiology helps??

1
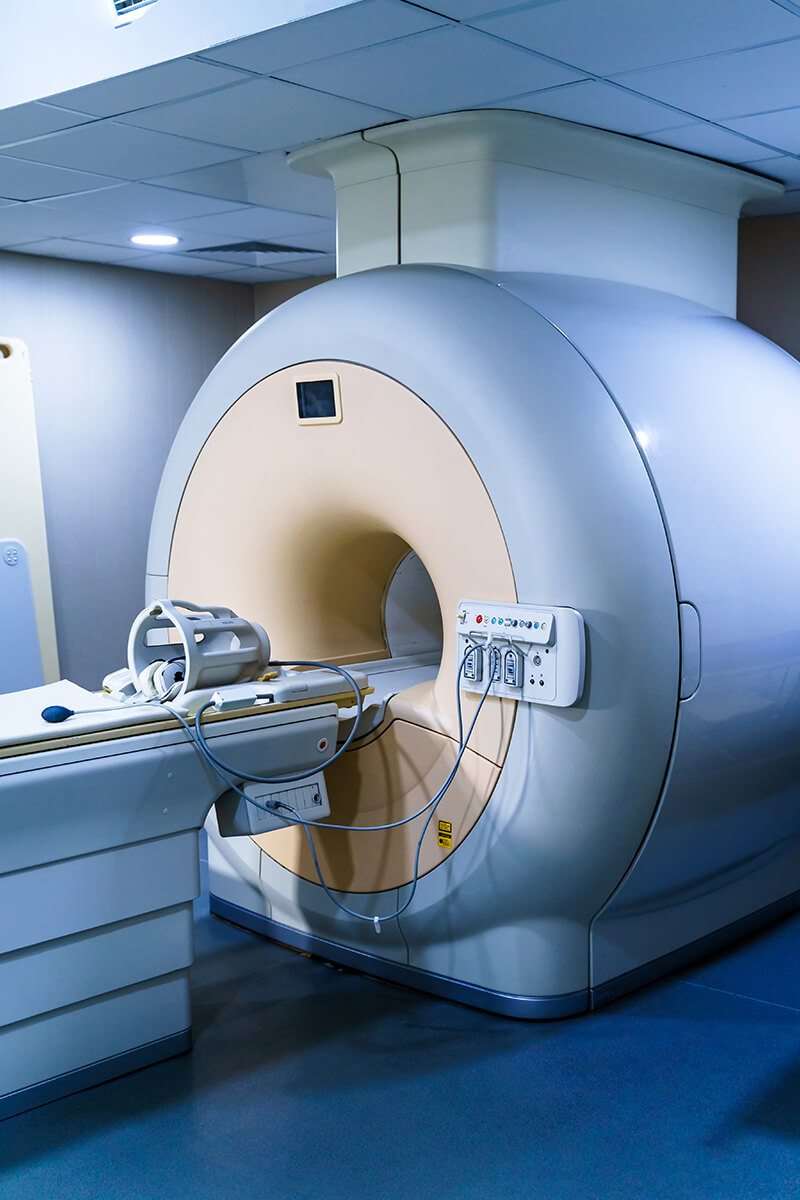
Imaging-Based Diagnosis
In order to precisely diagnose illnesses and direct treatments in real time, interventional radiology depends on high-resolution imaging techniques like ultrasound, CT, and MRI. This allows medical professionals to see precisely where and how to intervene.

2
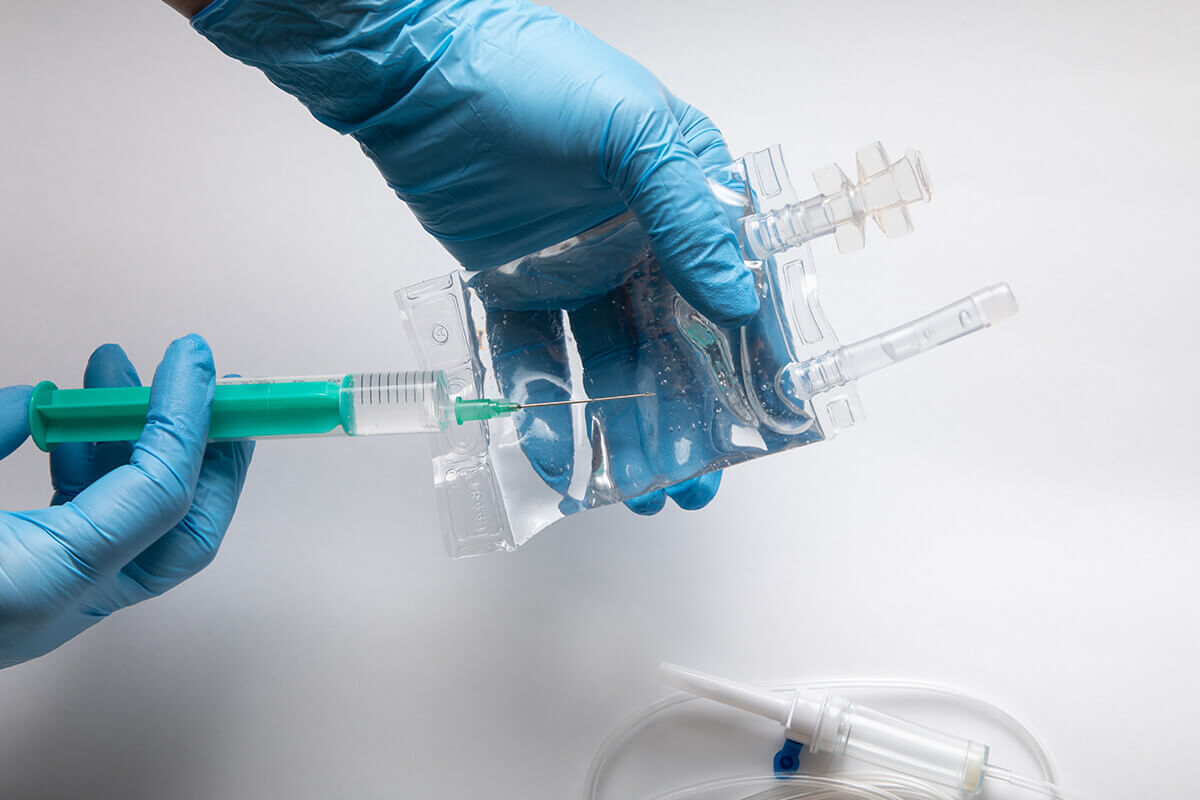
Accuracy and Precision
Interventional radiologists can target only the problematic area while preserving healthy tissues with unparalleled precision thanks to advanced imaging. This precision results in less adverse effects and more effective treatments.
3
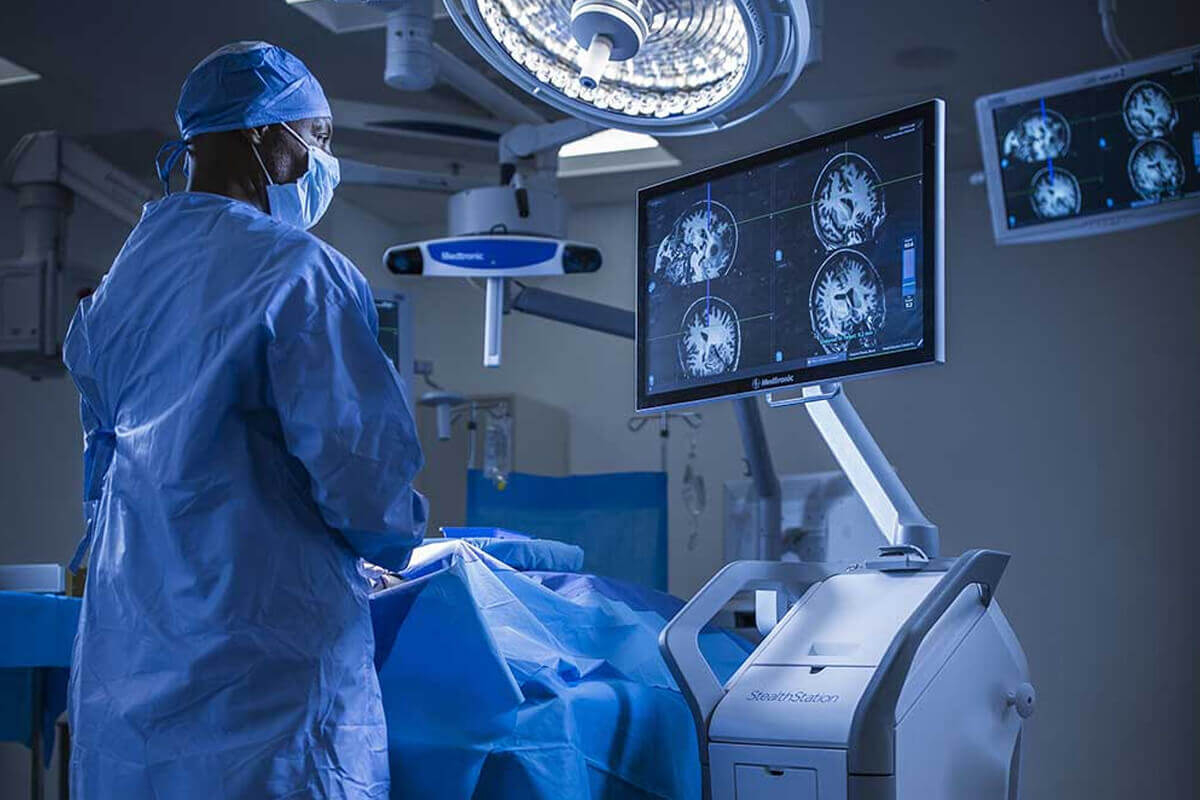
Modern Advanced Alternative
Interventional radiology provides a modern substitute for traditional surgery by performing minimally invasive procedures that lessen trauma and encourage quicker healing with the use of state-of-the-art technology.
4
Trusted for Multiple Conditions
This area is a reliable option for many specialties where less invasive methods are advantageous for both diagnosis and treatment because it treats a broad range of ailments, including cancer, vascular disease, and chronic pain.
why choose IR?
Need Any Help? We're Here To Help You!
No Stitches, No Cuts
Because the majority of IR procedures are carried out through small incisions or naturally occurring body openings, there is less discomfort and scarring because there is no need for large surgical cuts, stitches, or staples.

Minimally Invasive Procedure
Treatment is directed directly at the cause of the illness using imaging and micro-instruments, reducing bodily trauma and enabling the majority of procedures to be performed as outpatients.

Less Risk, Less Pain
Compared to traditional surgery, IR’s delicate, accurate technique results in much less pain both during and after the procedure, as well as a lower risk of infection, blood loss, and other complications.

Quick Recovery
Shorter hospital stays, quicker recovery, and an early return to regular activities are all advantages for patients, who frequently leave the hospital the same day with little to no downtime.

Frequently Asked Questions
What is Interventional radiology?
Interventional radiology (IR) is a branch of medicine that offers minimally invasive options for diagnosing and treating a range of conditions by using sophisticated imaging (such as X-rays, CT scans, MRIs, or ultrasounds) to guide tiny instruments inside the body.
What conditions is IR able to treat?
Vascular diseases, cancers, varicose veins, blocked arteries or veins, women's health conditions (such as fibroids), and many other conditions can all be managed with the aid of interventional radiology. Across various organ systems, it is reliable for both therapeutic and diagnostic procedures.
What are IR's primary advantages?
Less pain, less scarring, a decreased risk of infection, a quicker recovery, and the fact that most procedures don’t require general anesthesia or lengthy hospital stays are some advantages.
During my procedure, will I be awake?
The majority of IR procedures involve mild sedation and local anesthesia, which leaves patients pain-free and comfortable but either awake or slightly sleepy throughout the procedure.
How secure are IR practices?
Because interventional radiology is less invasive than traditional surgery, there is a lower chance of complications. Interventional radiologists have received specialized training to guarantee patient safety and employ risk-reduction strategies, such as cautious radiation management when necessary.
How much time does recovery take?
In contrast to open surgery, which frequently takes a few days to recover, most patients return home the same day or within 24 hours and are able to resume their regular activities much more quickly.
Does seeing an interventional radiologist require a referral?
Although some IR clinics may accept self-referrals, a referral from a primary care physician or specialist is usually helpful. For specific requirements, always check with the clinic.
Does insurance cover IR procedures?
Health insurance covers the majority of well-known IR treatments, though specifics may differ. Depending on the particular procedure, the clinic staff can assist in elucidating coverage and costs.




